Why a Suboxone Treatment Plan is Your Roadmap to Recovery
A Suboxone treatment plan is your roadmap to recovery from opioid use disorder. It’s a structured, medically supervised approach that combines the medication Suboxone with counseling and support. This isn’t just replacing one drug with another; it’s a proven medical treatment that gives you back control. In fact, people with opioid use disorder are 50% less likely to die when treated long-term with medications like Suboxone.
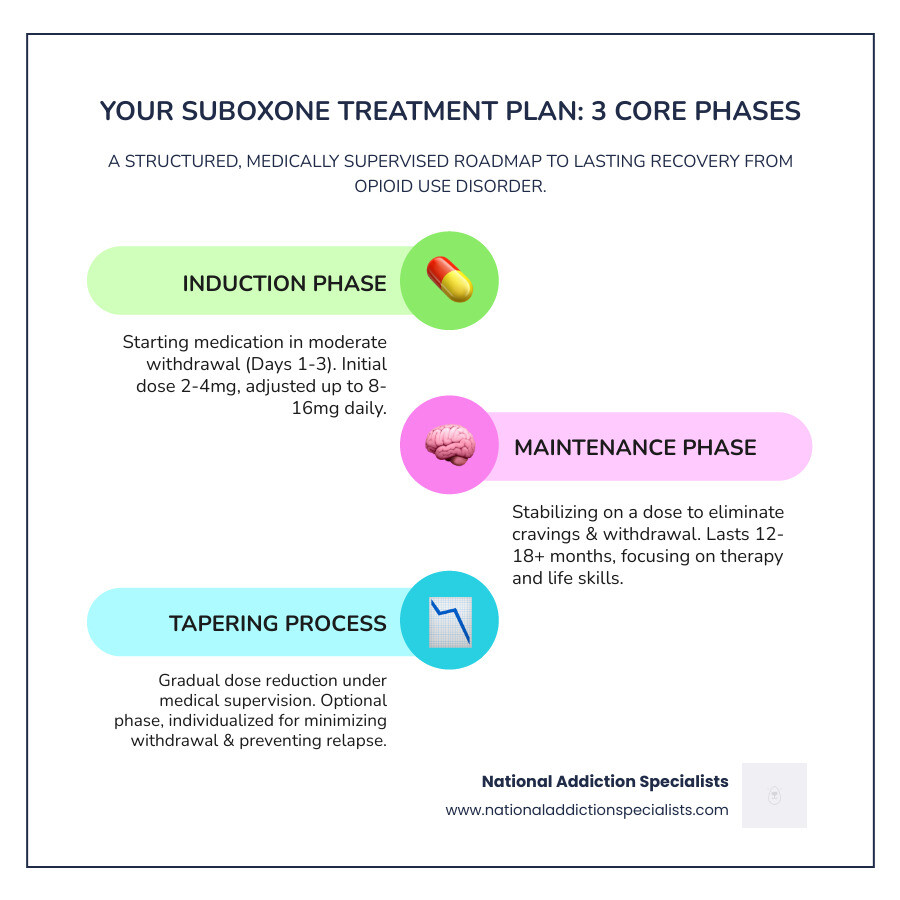
The plan generally follows three phases:
- Induction Phase: Starting the medication to manage withdrawal.
- Maintenance Phase: Stabilizing on a dose that eliminates cravings.
- Ongoing Support: Using counseling to address the root causes of addiction.
Medication alone isn’t enough. A comprehensive plan addresses both the physical dependence and the underlying psychological factors. I’m Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists, where I’ve helped thousands of patients steer their Suboxone treatment plans through accessible telehealth services. In this guide, I’ll walk you through what to expect on your path to recovery.
Common Suboxone treatment plan vocab:
Understanding Suboxone: The Foundation of Your Treatment
Before you can fully appreciate how a Suboxone treatment plan works, it helps to understand what you’re actually taking and why it’s so effective. Think of Suboxone as a carefully designed tool that gives your brain what it needs to heal—without the dangers of the opioids that brought you here.
What is Suboxone and How Does It Work?
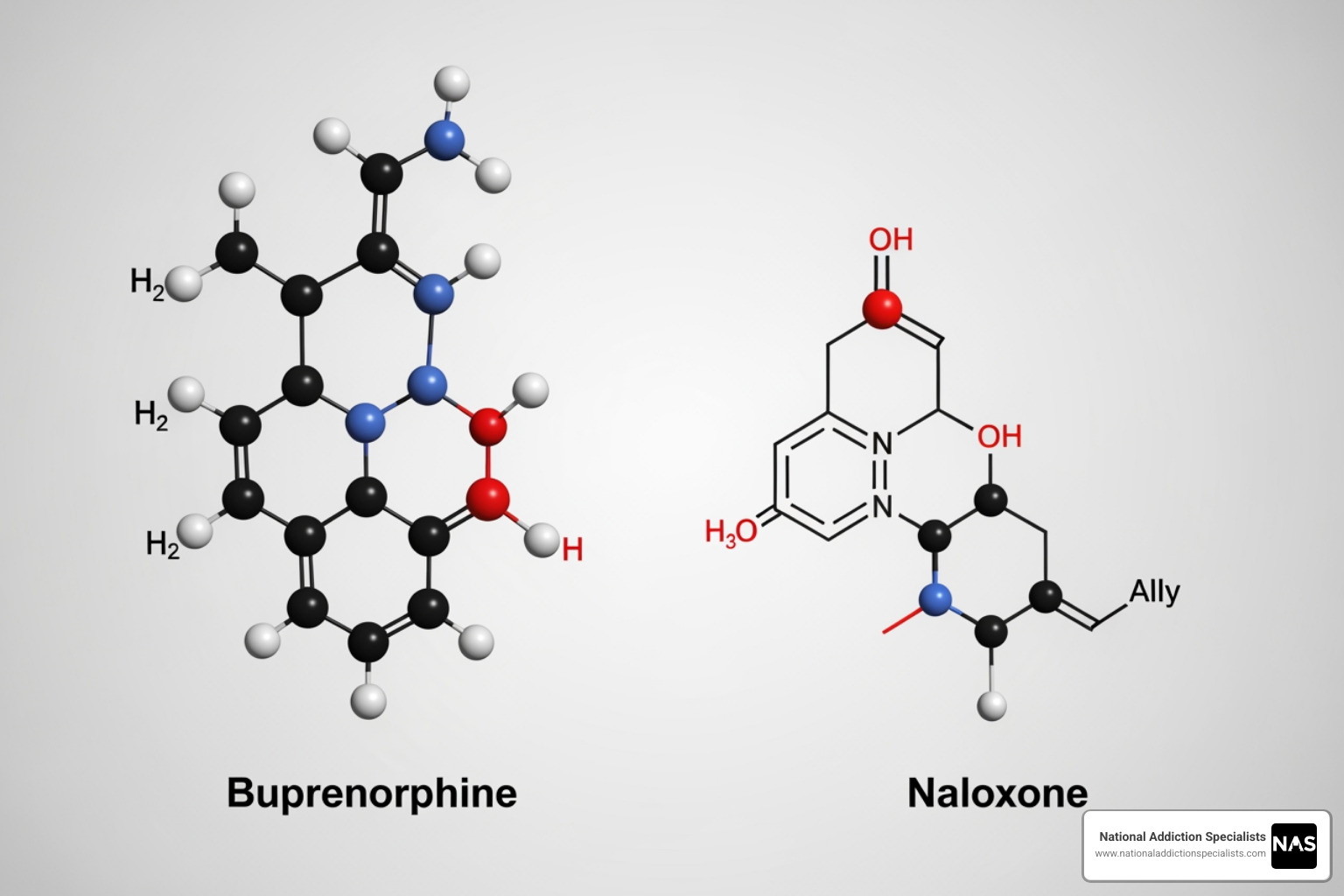
Suboxone is an FDA-approved medication for opioid use disorder containing two active ingredients: buprenorphine and naloxone.
- Buprenorphine: This is the main component. As a partial opioid agonist, it activates the brain’s opioid receptors just enough to stop cravings and withdrawal symptoms, but not enough to cause a high. This creates a “ceiling effect,” which significantly reduces the risk of overdose compared to full opioids like heroin or fentanyl. You can learn more about the science on our page on How Suboxone Opioid Treatment Works.
- Naloxone: This is an opioid antagonist included to deter misuse. When Suboxone is taken as prescribed (dissolved under the tongue), naloxone is not absorbed. However, if the medication is injected, the naloxone activates and can cause immediate, unpleasant withdrawal symptoms.
Together, these ingredients provide a stable foundation for recovery. Learn more about this approach on our Medication Assisted Treatment page.
Benefits of a Medically Supervised Suboxone Plan
A medically supervised Suboxone treatment plan offers life-changing benefits:
- Reduces Overdose Risk: People in long-term treatment with buprenorphine are 50% less likely to die from an overdose.
- Restores Stability: By managing cravings and withdrawal, Suboxone allows you to regain clarity and focus on daily life, work, and family.
- Improves Treatment Retention: Patients on Suboxone are more likely to stay in treatment, a key predictor of long-term success.
- Enables Deeper Healing: With physical symptoms managed, you can focus your energy on counseling and therapy to address the root causes of addiction.
- It’s a Proven Standard of Care: Buprenorphine is recognized by the World Health Organization as an essential medicine for treating opioid addiction.
For a more detailed look at these advantages, read our article on the Benefits of Suboxone Treatment for Opioid Addiction.
Ready to experience these benefits for yourself? Make an appointment today—please don’t hesitate to take this important step toward recovery.
The Core Phases of a Comprehensive Suboxone Treatment Plan
Think of your Suboxone treatment plan as a roadmap with clear milestones along the way. Your journey typically moves through several distinct phases: induction (getting started), stabilization (finding your footing), and maintenance (building your new life). A tapering phase may be considered later, but it is not a required goal. At National Addiction Specialists, we tailor every aspect of your plan to your unique situation, medical history, and recovery goals.

Key Considerations Before Starting Your Suboxone Treatment Plan
Before you take your first dose, we need to ensure everything is set up for your success and safety. This involves a comprehensive patient assessment of your medical history and substance use patterns.
Your opioid use history is critical for timing your first dose. To avoid a severe reaction called precipitated withdrawal, you must wait until you are in moderate withdrawal. The waiting period depends on the type of opioid used:
- Short-acting opioids (heroin, oxycodone): Wait at least 12 hours after your last use.
- Long-acting opioids (fentanyl, methadone): The wait is longer, often 36 to 72 hours or more.
We use the Clinical Opiate Withdrawal Scale (COWS) to measure your symptoms. A score of 17 or higher usually means you are ready to start. We may also conduct a physical exam and lab work, such as a drug test and pregnancy test, to create the safest plan for you.
If you’re ready to take this important first step toward recovery, please don’t hesitate. Make an appointment today.
Phase 1: The Induction Phase
The induction phase is where your recovery truly begins, typically lasting 1 to 3 days. Under medical guidance, you’ll take your first doses of Suboxone to relieve withdrawal symptoms. At National Addiction Specialists, this can often be done safely at home via telehealth.
Your initial dose will be small, usually 2mg to 4mg. Most patients feel better within 30 to 45 minutes. On Day 1, the total dose may be increased up to 8mg/2mg, given in divided doses. By Day 2, we typically transition to a single daily dose of up to 16mg/4mg. Your medical team monitors you closely and adjusts the dosage to keep you comfortable, following scientific research on Suboxone dosing guidelines.
Phase 2: The Maintenance Phase
After induction, you enter the maintenance phase. Here, we find the right dose—the average is 16mg daily, but it varies—that eliminates your cravings and withdrawal symptoms without side effects. Many patients start feeling “normal” around Day 5 and often experience a hopeful “honeymoon” stage around week 2.
Research recommends staying on Suboxone for at least 12 to 18 months. For many, long-term treatment is the safest and most effective choice. The goals of this phase are to eliminate cravings, prevent withdrawal, and allow you to focus on therapy and rebuilding your life while your brain chemistry normalizes.
Phase 3: The Tapering Process
After a significant time in maintenance, some people consider tapering off Suboxone. This is entirely optional and not the right choice for everyone. If you and your doctor agree to it, tapering involves a very gradual dose reduction over weeks or months. Medical supervision is absolutely critical, as stopping abruptly can cause severe withdrawal and increase relapse risk. Relapse rates can exceed 50% when buprenorphine is discontinued, so this process requires robust counseling and a strong relapse prevention plan.
Integrating Support: The Holistic Approach to Recovery
While Suboxone is highly effective for the physical symptoms of opioid use disorder, lasting recovery also requires skills, support, and healing beyond medication.

The Crucial Role of Counseling and Therapy
Medication creates stability; therapy builds the life skills to keep it. Effective options include:
- Cognitive Behavioral Therapy (CBT): Identify and change thought patterns and behaviors linked to use.
- Individual therapy: Address stress, trauma, and co-occurring conditions in a private setting.
- Group therapy: Learn from peers, reduce isolation, and increase accountability.
Explore more on our Importance of Counseling and Therapy in Suboxone Treatment page and our Counseling Program.
Managing Side Effects and Dependence in Your Suboxone Treatment Plan
Common, often temporary side effects include constipation, headache, and nausea. Hydration, fiber, activity, and over-the-counter options may help—check with your clinician. Learn what to expect on our What to Expect with Suboxone Side Effects page.
Physical dependence (your body adapts to medication) is expected and different from addiction (compulsive use despite harm). Treating opioid use disorder with Suboxone is not replacing one addiction with another; it’s evidence-based medical care.
The Core Phases of a Comprehensive Suboxone Treatment Plan
Recovery typically progresses through induction, stabilization/maintenance, and, for some, tapering. Your plan is individualized and medically supervised to keep you safe and comfortable.
Key Considerations Before Starting Your Suboxone Treatment Plan
To avoid precipitated withdrawal, you must be in moderate opioid withdrawal before your first dose. We consider your opioid type (short- vs. long-acting), medical history, and may order labs, including a drug test and pregnancy test. Tools like the COWS score help determine readiness.
Ready to get started? Make an Appointment to Treat Addiction. Please don’t hesitate. Make an appointment today.
Phase 1: The Induction Phase
Usually 1–3 days. We start low (often 2–4 mg) and carefully increase to relieve withdrawal and cravings, aligning with scientific research on Suboxone dosing guidelines. Many people feel better within 30–45 minutes. Day 1 may total up to 8 mg/2 mg; Day 2 often consolidates to a single daily dose up to 16 mg/4 mg.
Phase 2: The Maintenance Phase
We fine-tune your dose—commonly around 16 mg/day—to eliminate cravings and withdrawal so you can focus on therapy, relationships, work, and restoring brain health. Many feel “normal” by Day 5, with increasing stability over the following weeks.
Phase 3: The Tapering Process
Tapering is optional and highly individualized. If pursued, it’s done gradually with medical supervision and a strong relapse-prevention plan, given higher relapse risk after discontinuation.
Integrating Support: The Holistic Approach to Recovery
Suboxone treats the biology of addiction; counseling and skills-based support help you rebuild daily life and protect your recovery.
The Crucial Role of Counseling and Therapy
- CBT to reframe thoughts and behaviors
- Individual therapy for coping skills and co-occurring conditions
- Group therapy for connection and accountability
Learn more: Importance of Counseling and Therapy in Suboxone Treatment and our Counseling Program.
Managing Side Effects and Dependence in Your Suboxone Treatment Plan
Constipation, headache, and nausea are the most common early side effects and are usually manageable—talk with your clinician. Physical dependence is expected and not the same as addiction. For details, see What to Expect with Suboxone Side Effects.
The Core Phases of a Comprehensive Suboxone Treatment Plan
Here’s a streamlined overview of the phases, with links to key resources you may need along the way.
Key Considerations Before Starting Your Suboxone Treatment Plan
- Be in moderate withdrawal before the first dose (to prevent precipitated withdrawal).
- Assessment may include a physical exam and labs like a Drug Test and Pregnancy Test.
- Short-acting opioids typically require a shorter wait than long-acting opioids.
Make an Appointment to Treat Addiction. Please don’t hesitate. Make an appointment today.
Phase 1: The Induction Phase
- Start low (often 2–4 mg), then adjust to comfort.
- Day 1 up to 8 mg/2 mg; Day 2 up to 16 mg/4 mg, following scientific research on Suboxone dosing guidelines.
Phase 2: The Maintenance Phase
- Find your optimal daily dose (commonly around 16 mg) to stop cravings/withdrawal and support therapy and life goals.
Phase 3: The Tapering Process
- Optional, gradual, medically supervised dose reductions with strong relapse-prevention supports.
Integrating Support: The Holistic Approach to Recovery
Medication plus psychosocial support is the gold standard. Build a plan that strengthens both.
The Crucial Role of Counseling and Therapy
- Why counseling matters: It teaches coping skills, addresses trauma, and helps manage triggers—things medication alone can’t do.
- What helps: CBT, individual therapy, and group therapy.
- Get connected: Importance of Counseling and Therapy in Suboxone Treatment and our Counseling Program.
Managing Side Effects and Dependence in Your Suboxone Treatment Plan
- Common side effects: constipation, headache, nausea—usually manageable and often improve with time. Discuss strategies with your clinician.
- Dependence vs. addiction: Physical dependence is expected with Suboxone and isn’t the same as addiction. Suboxone reduces harm, cravings, and overdose risk while you rebuild your life.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








