The Suboxone-Subutex Showdown: A Guide to Opioid Addiction Medications
Why Understanding Your Medication Options Matters
Suboxone for opioid addiction is an FDA-approved medication combining buprenorphine and naloxone to treat opioid use disorder. Here’s a quick overview:
- What it does: Reduces withdrawal symptoms and cravings while blocking the euphoric effects of other opioids.
- How effective: Lowers fatal overdose risk by approximately 50% and significantly improves treatment retention.
- Key difference from Subutex: Contains naloxone to deter misuse, while Subutex is buprenorphine only.
- Treatment duration: Individualized and often long-term, similar to managing other chronic conditions.
- Access: Available through traditional clinics and increasingly via telehealth services.
If you or a loved one is struggling with opioid use disorder, know that effective, evidence-based help is available. Medication-assisted treatment with drugs like Suboxone leads to higher rates of abstinence and clinical stability. However, understanding your options—Suboxone vs. Subutex, treatment duration, insurance, and privacy—can be daunting.
This guide provides clear answers. We’ll explore the science behind these medications, what to expect during treatment, and how telehealth is making recovery more accessible and discreet than ever.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists. I’ve dedicated my career to treating Suboxone for opioid addiction and have seen how the right medication and support can transform lives.
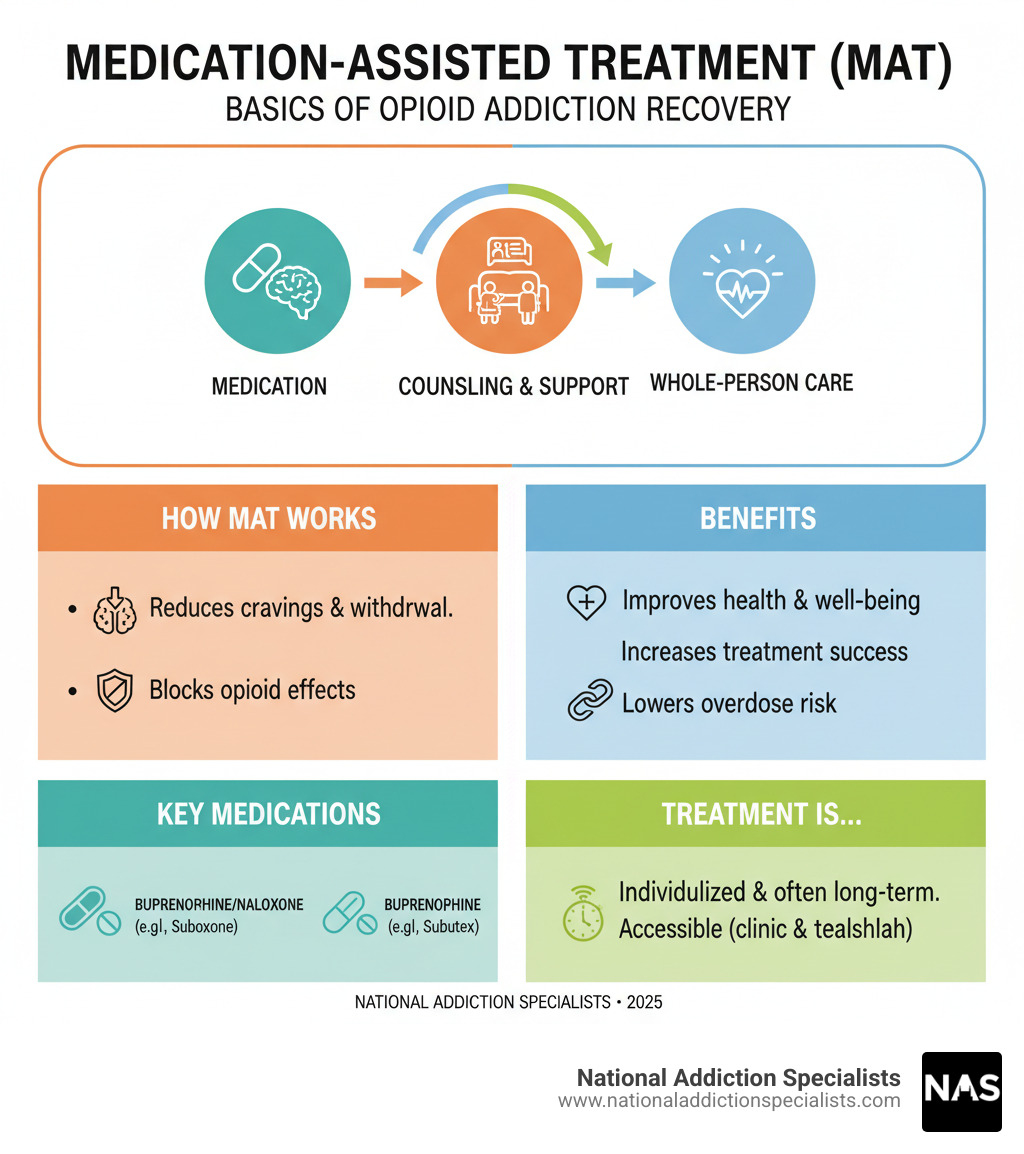
Suboxone for opioid addiction terms to remember:
What Are Suboxone and Subutex? Unpacking the Medications
Suboxone and Subutex are key medications in Medication-Assisted Treatment (MAT), which combines medication with counseling to treat opioid use disorder. Let’s break down how they work.
Buprenorphine: The Core of Treatment
Both Suboxone and Subutex contain buprenorphine, a partial opioid agonist. Think of opioid receptors in your brain as locks. Full opioids like heroin are keys that turn the lock completely, causing a high. Buprenorphine is a key that only turns the lock partway. It activates opioid receptors just enough to reduce cravings and alleviate withdrawal symptoms without producing a dangerous high.
This partial activation gives buprenorphine two key safety features:
- A ceiling effect: After a certain dose, its effects plateau, making it much harder to overdose on buprenorphine alone compared to full opioids.
- A blocking effect: Buprenorphine binds tightly to opioid receptors, blocking other opioids from attaching. This means if someone uses other opioids while on buprenorphine, they won’t feel the expected euphoric effects, which helps prevent relapse.
In my practice, I’ve seen buprenorphine help people feel “normal” again—not high, just stable—so they can focus on recovery. Learn more about this cornerstone medication here: What is Buprenorphine?
The Role of Naloxone in Suboxone
The key difference between Suboxone and Subutex is naloxone, an opioid antagonist that blocks opioid receptors. In Suboxone, naloxone acts as a misuse deterrent.
When you take Suboxone as prescribed (dissolving it under your tongue), the buprenorphine is absorbed, but the naloxone remains mostly inactive. However, if someone tries to inject Suboxone to get high, the naloxone activates and immediately blocks opioid receptors. This triggers severe, immediate withdrawal symptoms, known as precipitated withdrawal, making the medication much less appealing to misuse.
This built-in safeguard is designed to ensure the medication is used safely. For more details on how naloxone works in addiction treatment, visit: More on Naloxone’s role
Suboxone vs. Subutex: The Key Difference
The presence of naloxone is the main distinction between these two medications.
| Feature | Suboxone (Buprenorphine/Naloxone) | Subutex (Buprenorphine only) |
|---|---|---|
| Composition | Buprenorphine + Naloxone | Buprenorphine only |
| Misuse Potential | Lower risk due to naloxone deterrent | Higher theoretical risk if injected |
| Common Use Cases | Standard treatment for most patients with OUD | Primarily during pregnancy or if naloxone is contraindicated |
Suboxone is the most commonly prescribed option for Suboxone for opioid addiction treatment because the naloxone component makes it safer from a misuse standpoint.
Subutex (buprenorphine-only) is less common but is the preferred choice during pregnancy to avoid exposing the fetus to naloxone. It may also be used for patients with a rare sensitivity to naloxone.
Both are effective tools, and your provider will help determine the right choice for your specific situation. For a deeper comparison, check out: Suboxone vs Subutex
The Comprehensive Guide to Suboxone for Opioid Addiction
Suboxone for opioid addiction is a cornerstone of modern recovery because it is a scientifically-backed medication that offers a real path forward when combined with counseling and support.
How Does Suboxone Work to Treat Opioid Addiction?
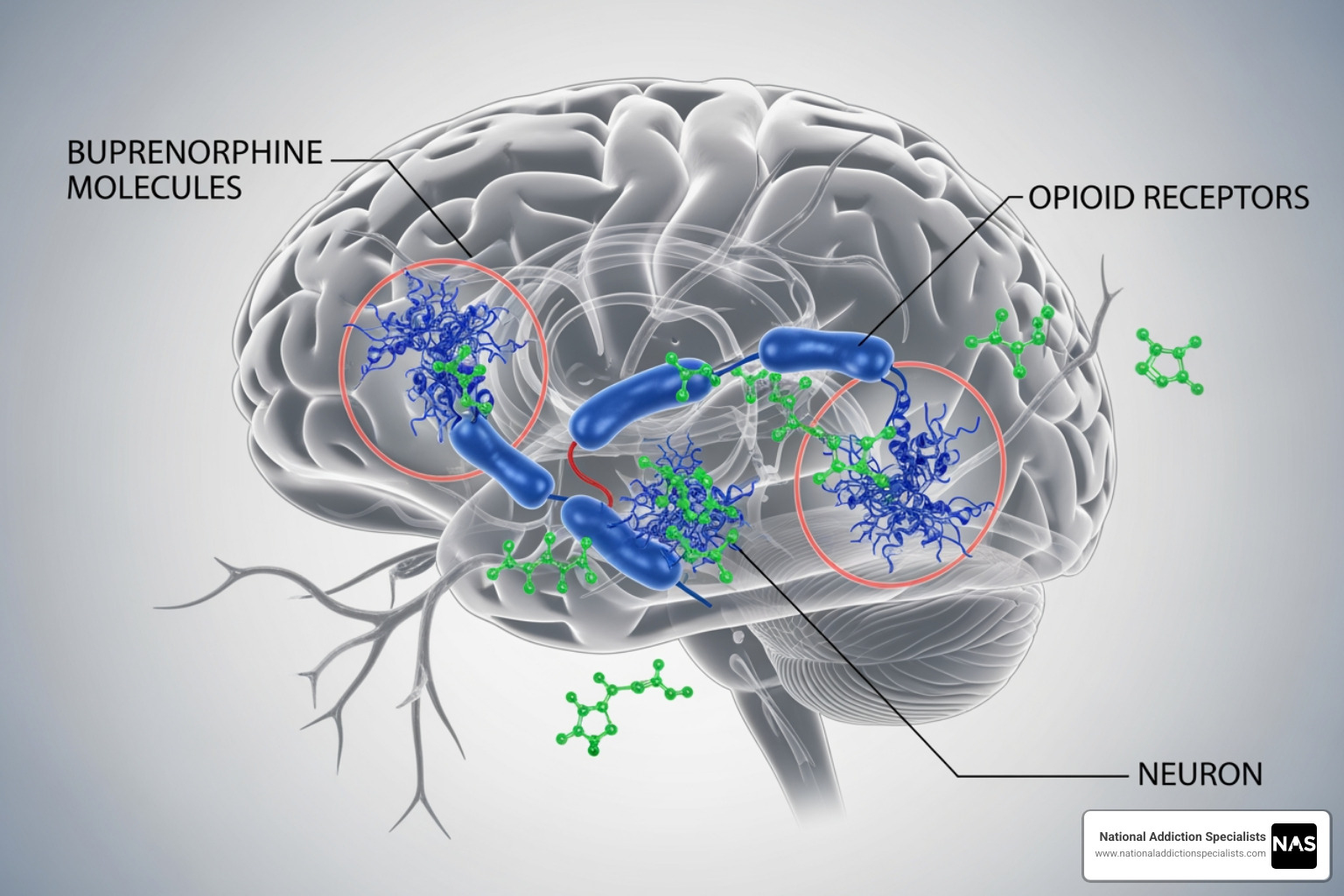
As explained earlier, buprenorphine is a partial agonist that fits into the brain’s opioid receptors. This action accomplishes three critical things:
- Alleviates withdrawal symptoms: It satisfies the brain’s receptors enough to stop the muscle aches, nausea, and other miseries of withdrawal.
- Blocks euphoric effects of other opioids: By occupying the receptors, buprenorphine prevents other opioids like heroin or fentanyl from producing a high, making relapse less rewarding.
- Reduces cravings: This is perhaps the most significant effect. One study showed that after starting Suboxone, patients’ craving scores dropped from over 62 to just 29.8, compared to 55.1 for a placebo group. This frees you to focus on rebuilding your life.
This dual action of satisfying and blocking receptors is what makes Suboxone so effective. You can learn more about the mechanics here: How Suboxone Treatment Works
The Proven Benefits of Suboxone Treatment
The evidence supporting Suboxone for opioid addiction is overwhelming, and the World Health Organization includes buprenorphine on its list of essential medicines. Key benefits include:
- Lowered overdose risk: Suboxone lowers the risk of a fatal overdose by approximately 50%.
- Improved treatment retention: Patients on buprenorphine are far more likely to stay in treatment, which is strongly linked to long-term success.
- Reduced illicit opioid use: Clinical trials consistently show that patients taking Suboxone dramatically reduce or stop using other opioids.
- Greater clinical stability: With cravings and withdrawal managed, patients can improve their physical and mental health, repair relationships, and return to work or school.
- Broader access: Unlike methadone, which requires daily clinic visits, Suboxone can be prescribed in a physician’s office or via telehealth, making treatment more accessible.
Learn more about these advantages here: Benefits of Suboxone Treatment
The Three Phases of Buprenorphine Treatment
Suboxone treatment follows a structured, three-phase approach to ensure safety and effectiveness:
- The Induction Phase: This is the medically monitored start of treatment. Buprenorphine is initiated once you are in mild to moderate withdrawal to avoid causing precipitated withdrawal. The goal is to find a starting dose that relieves your symptoms.
- The Stabilization Phase: During this phase, your dose is fine-tuned to find the optimal level that controls cravings and withdrawal with minimal side effects. This process is individualized and is not rushed.
- The Maintenance Phase: Once stable, you continue on your dose long-term. This phase provides the support needed to build a new life through counseling, new habits, and skill development. It can last for months or years, depending on your needs.
This personalized approach ensures your treatment is medically sound and adapted to your progress. To learn more about our comprehensive treatment program, visit: Medication Assisted Treatment Program
Navigating Treatment: What to Expect on Your Journey
Starting treatment is a brave step. Let’s walk through the practical considerations of what to expect regarding side effects, treatment duration, and cost.
Potential Side Effects and Safety Precautions
While most people tolerate Suboxone well, it’s important to be aware of potential side effects, which are often mild and temporary. These can include nausea, constipation, headaches, sweating, or trouble sleeping. More seriously, there are critical safety precautions:
- Precipitated Withdrawal: This can occur if you start Suboxone too soon after using other opioids. We prevent this by carefully assessing your withdrawal level (using the COWS scale) before your first dose.
- Risk of Overdose When Mixed: Never mix Suboxone with alcohol or benzodiazepines (like Xanax or Klonopin). This combination can cause fatal respiratory depression. Be completely transparent with your provider about all substances you use.
- Dental Health: Long-term use of sublingual buprenorphine can be acidic and cause dry mouth, leading to tooth decay. Regular dental check-ups and good oral hygiene are essential.
- Medical Supervision: Your safety is our priority. We start with a low dose, monitor you closely, and ensure you know how to store your medication safely, especially away from children.
For more details, see: What to Expect Suboxone Side Effects and Dangers of Mixing Suboxone and Alcohol.
How Long Does Suboxone Treatment Last?
There is no one-size-fits-all timeline for Suboxone treatment. Opioid use disorder is a chronic disease, similar to diabetes or high blood pressure, which often requires ongoing management. The idea that Suboxone is a short-term fix is a myth unsupported by science.
In fact, studies show that patients who remain on buprenorphine longer have significantly better outcomes, including lower rates of illicit opioid use and greater stability. Many people stay on the medication for years, or even indefinitely, because it is the most effective way to support their long-term recovery.
The decision on treatment duration is made between you and your provider, based on your progress and well-being. The goal is a healthier, stable life, not a race to get off medication. Explore this topic more here: How Long Should I Stay on Suboxone?
Insurance Coverage for Suboxone for Opioid Addiction
Cost should not be a barrier to life-saving treatment. Accessing Suboxone for opioid addiction is more affordable than many people think.
- Most Insurance Plans: The Affordable Care Act (ACA) requires most plans to cover substance use disorder treatment, including Suboxone.
- Medicaid: In Tennessee and Virginia, Medicaid typically covers Suboxone treatment. We proudly accept it at National Addiction Specialists.
- Medicare: Medicare also generally covers Medication-Assisted Treatment, including Suboxone.
Our team can help you verify your insurance benefits before your first appointment to ensure treatment is accessible and affordable. For more information, visit: Does Insurance Cover Suboxone Treatment? and Medicaid Suboxone Treatment.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Debunking Myths and Setting the Record Straight
Misinformation about Suboxone for opioid addiction can prevent people from seeking life-saving care. Let’s separate the myths from the facts.
Myth: “You’re just trading one addiction for another.”
- Reality: Opioid use disorder is a medical brain disease. Taking Suboxone is not an addiction; it’s a medical treatment, just like taking insulin for diabetes. It allows people to stabilize their lives and function normally.
Myth: “It’s just a crutch.”
- Reality: Suboxone is a tool that provides necessary support while a person heals. It manages the physical symptoms that would otherwise make recovery nearly impossible, much like a crutch supports a broken leg.
Myth: “People abuse Suboxone all the time.”
- Reality: Suboxone is designed to be difficult to misuse. The naloxone deters injection, and buprenorphine has less euphoric effect than other opioids. When misuse occurs, it’s often a sign of desperation from those unable to access proper treatment.
Myth: “You can overdose on Suboxone just like other opioids.”
- Reality: Due to buprenorphine’s “ceiling effect,” it is extremely difficult to fatally overdose on Suboxone alone. Overdoses almost always involve mixing it with other depressants like benzodiazepines or alcohol.
Myth: “You should only be on Suboxone for a short time.”
- Reality: This contradicts all medical research. Opioid use disorder is a chronic condition, and long-term maintenance on Suboxone is often the most effective path to recovery. Studies show better outcomes for those who stay on medication longer.
Don’t let these myths hold you back from considering a treatment that has helped millions. Read more here: Myths About Using Suboxone Opioid Addiction.
The Rise of Telehealth in Addiction Recovery
Telehealth has revolutionized addiction treatment, making comprehensive Suboxone for opioid addiction care more accessible than ever. It has become one of our most powerful tools for reaching people who need help.
How Online Suboxone Doctors Increase Access to Care
For years, barriers like distance, work schedules, and fear of stigma kept people from receiving care. Telehealth eliminates these obstacles.
- Overcoming Geographic Barriers: Patients in rural Tennessee and Virginia can now connect with our expert providers from home, regardless of their location.
- Convenience and Privacy: Receive high-quality medical care without taking time off work, arranging childcare, or traveling. Appointments are conducted from the comfort and privacy of your own space.
- Reducing Stigma: The anonymity of receiving care at home removes the fear of being seen or judged, encouraging more people to take the first step.

Recent regulatory changes, like the elimination of the “X-waiver” and extended telehealth flexibilities, have further expanded access, allowing more providers to prescribe buprenorphine remotely. Learn more here: Telemedicine in Suboxone Treatment.
What to Expect from a Virtual Suboxone Clinic
At National Addiction Specialists, our virtual clinic provides comprehensive, supportive care with the added benefits of telehealth. Here’s how it works:
- Virtual Consultations: You’ll have thorough, private video appointments with board-certified addiction medicine specialists to create your personalized treatment plan.
- E-prescribing to Local Pharmacies: We send your Suboxone prescription electronically to your preferred local pharmacy in Tennessee or Virginia for convenient and discreet pickup.
- At-Home Drug Screening: We monitor your progress with private at-home tests to ensure your treatment is safe and effective.
- Integrated Virtual Counseling: Our program includes access to virtual therapy and support groups with licensed specialists to address the emotional and psychological aspects of recovery.
Our model is designed to make recovery as accessible and supportive as possible. Learn more about our services: Online Suboxone Clinic and Virtual Addiction Counseling.
Conclusion: Your Path to Recovery Starts Here
Recovery from opioid addiction is a journey, and Suboxone for opioid addiction and Subutex are powerful, evidence-based tools that can make that journey successful. These medications provide a stable foundation, managing the physical cravings and withdrawal so you can focus on healing.
With the rise of telehealth, expert care from providers like National Addiction Specialists is more accessible than ever. You can receive compassionate, life-saving treatment from the privacy of your home in Tennessee or Virginia. The hardest part is taking the first step, but you don’t have to do it alone.
Take the First Step
Recovery is possible, and help is available. Our team at National Addiction Specialists understands what you’re going through and is ready to guide you.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Your path to recovery starts with the decision to reach out. Schedule Addiction Treatment and take that first step toward the life you deserve.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.