Everything You Need to Know About Kratom
What You Need to Know About Kratom Before Using It
Kratom is a plant-based substance from Southeast Asia that acts like a stimulant at low doses and like an opioid at high doses — and it carries serious risks that most people don’t fully understand before trying it.
Here’s a quick overview of the key facts:
| Topic | Key Facts |
|---|---|
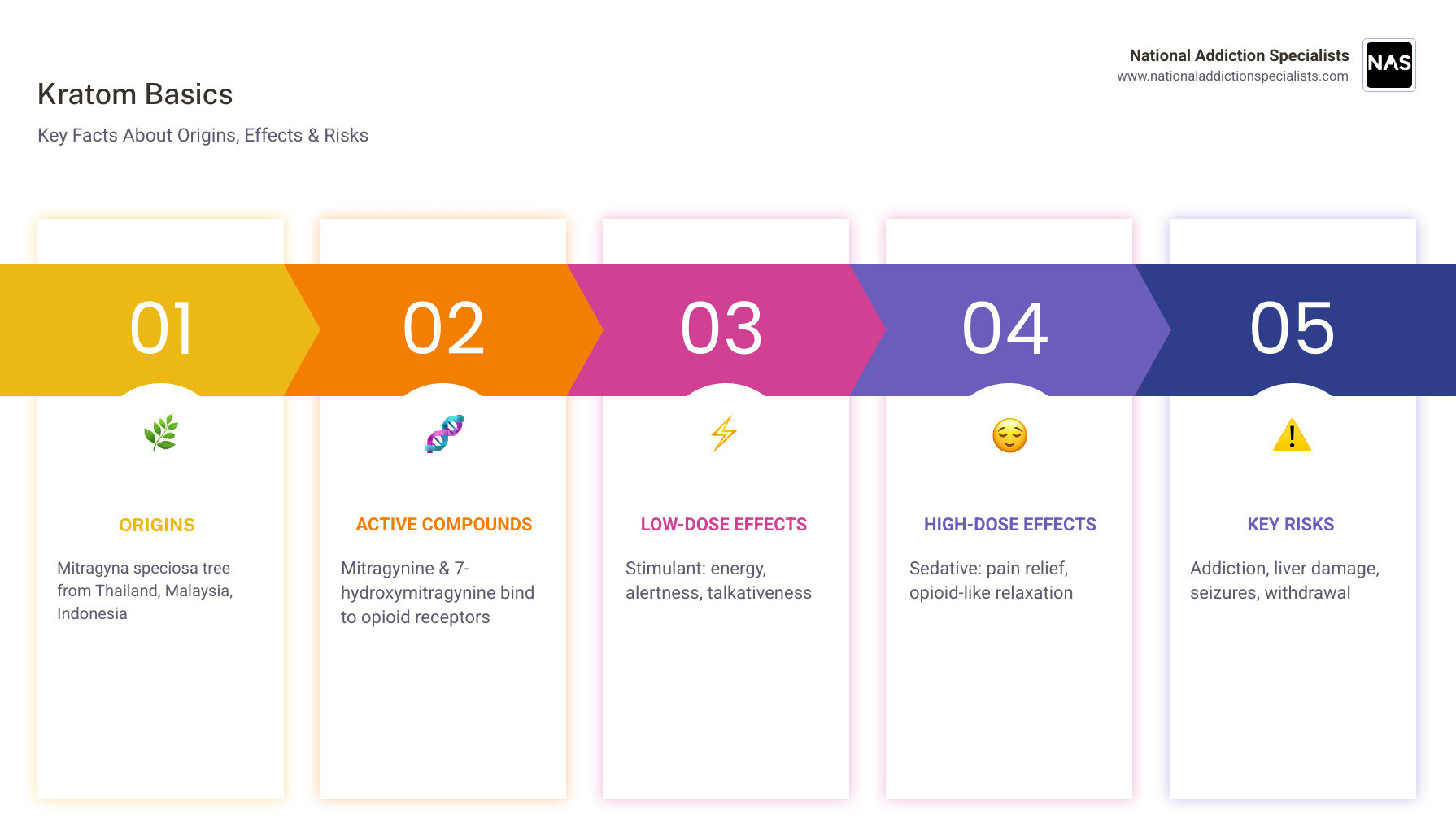
| What it is | Leaves of the Mitragyna speciosa tree, native to Thailand, Malaysia, and Indonesia |
| Active compounds | Mitragynine and 7-hydroxymitragynine (bind to opioid receptors) |
| Low-dose effects | Increased energy, alertness, talkativeness |
| High-dose effects | Sedation, pain relief, opioid-like effects |
| Key risks | Addiction, liver damage, seizures, psychosis, withdrawal |
| Legal status (US) | Not federally controlled, but flagged by FDA and DEA; some states restrict it |
| FDA approved? | No — not approved for any medical use |
| Who uses it | Estimated 1.7 million Americans (2021); 15 million people worldwide |
Kratom is increasingly used in the US to self-manage pain and opioid withdrawal — but the research on its safety is still very limited, and health authorities have raised serious red flags about its risks and the quality of products on the market.
I’m Dr. Chad Elkin, board-certified in Addiction Medicine and founder of National Addiction Specialists, and I regularly treat patients who have developed a dependence on Kratom after using it to manage opioid withdrawal or chronic pain. Understanding what this substance actually does to your body is the first step toward making safer choices.
What is Kratom and Where Does it Come From?
To understand Kratom, we have to look toward the lush, tropical rainforests of Southeast Asia. Scientifically known as Mitragyna speciosa, this evergreen tree is a surprisingly close relative of the coffee plant (the Rubiaceae family). While it shares a family tree with your morning latte, its effects on the human brain are far more complex.
The tree is indigenous to countries like Thailand, Malaysia, Indonesia, Myanmar, and Papua New Guinea. In these regions, the plant has been known by many names for centuries, including thang, kakuam, thom, ketum, and biak. It was first formally described by Western botanists in 1839, but local communities had been using the leaves as part of their traditional medicine and social fabric long before then.

Common Forms of Kratom Available
In its native environment, you might see someone simply pluck a fresh leaf and chew it. However, because Kratom has traveled across the globe to the United States, it has been processed into several different forms to make it easier to ship and sell. According to Britannica, the most common forms you’ll find in shops or online include:
- Dried Leaves: Often crushed or kept whole to be brewed into tea.
- Powder: The most prevalent form, created by grinding dried leaves into a fine dust. This is often mixed into drinks or food.
- Capsules: Gelatin or veggie capsules filled with powder to avoid the plant’s notoriously bitter taste.
- Concentrated Extracts: These are potent liquids or resins that distill the plant’s alkaloids into a much smaller, stronger dose.
- Tablets: Compressed powder forms similar to standard over-the-counter pills.
Traditional vs. Modern Consumption
Historically, Kratom was the “blue-collar” herb of Southeast Asia. Manual laborers, such as farmers and timber workers, would chew the leaves to stave off exhaustion, boost energy, and numb the physical pain of a long day’s work. It was even used as a snack for guests or in religious rituals.
In contrast, modern consumption in the U.S. is often driven by self-medication. People frequently turn to Kratom as a “natural” alternative for managing chronic pain, anxiety, or depression. Perhaps most notably, it has gained a massive following among those trying to manage the grueling symptoms of opioid withdrawal. However, because these products are often sold as dietary supplements, they lack the rigorous testing and oversight that we expect from medicine.

The Short-Term and Long-Term Effects of Kratom
The reason Kratom is so unique—and so confusing—is its dual nature. It contains over 40 active compounds, but the two heavy hitters are mitragynine and 7-hydroxymitragynine. These alkaloids interact with the opioid receptors in your brain, but the “vibe” changes completely depending on how much you take.
| Dosage Level | Primary Effects | Typical Experience |
|---|---|---|
| Low Dose (1–5g) | Stimulant-like | Increased energy, social talkativeness, alertness, suppressed appetite. |
| High Dose (5–15g) | Opioid-like | Pain relief, sedation, euphoria, reduced anxiety. |
| Very High Dose (>15g) | Extreme Sedation | Can lead to “nodding out,” heavy drowsiness, and increased risk of side effects. |
Physiological Impact at Different Dosages
At low doses, users often report feeling more “up.” It’s a bit like a strong cup of coffee without the jitters, leading to increased physical energy and a desire to be social. However, as the dose increases, the pharmacology shifts. The alkaloids begin to bind more heavily to the mu-opioid receptors, which is why WebMD notes its use for pain relief.
While this might sound like a miracle plant, the body pays a price. The onset of these effects usually happens within 5 to 10 minutes and can last anywhere from 2 to 5 hours. During this time, the brain is being flooded with signals that can lead to a quick build-up of tolerance.
Potential Health Risks of Kratom Use
We often hear the word “natural” and assume “safe,” but that isn’t the case here. The Virginia Department of Health and other health authorities have documented a wide range of adverse effects.
Short-term side effects frequently include:
- Nausea and vomiting (the most common complaint)
- Itching and sweating
- Dry mouth and constipation
- Increased urination
- Tachycardia (rapid heart rate)
The long-term consequences of regular use are even more concerning. Chronic users may experience significant weight loss (anorexia), insomnia, and hyperpigmentation (darkening of the skin). More severely, Kratom has been linked to hepatotoxicity (liver damage), seizures, and even cases of psychosis. Between 2014 and 2019, U.S. poison control centers received over 3,400 reports regarding Kratom, highlighting a 52-fold increase in exposures since 2011.
Understanding Kratom Addiction and Withdrawal
Can you get addicted to Kratom? The short answer is yes. Because it hits the same receptors as morphine and oxycodone, the brain can become dependent on it to function normally. Research indicates that about 25.5% of users report symptoms that align with a Substance Use Disorder (SUD) diagnosis.
When someone tries to stop after regular use, they often fall into a cycle of dependence. They aren’t taking it to get “high” anymore; they are taking it just to feel “normal” and avoid the sickness that comes with stopping. If you find yourself in this position, Kratom treatment is available and can help you break the cycle safely.
Withdrawal Symptoms and Neonatal Risks
Kratom withdrawal is often described as a “lite” version of opioid withdrawal, but that doesn’t make it easy. Symptoms can include:
- Intense cravings
- Muscle aches and jerky limb movements
- Agitation and irritability
- Insomnia
- Diarrhea and runny nose
One of the most heartbreaking risks involves pregnancy. Health providers have seen an increase in Neonatal Abstinence Syndrome (NAS) in newborns whose mothers used Kratom. These babies are born physically dependent and suffer from jitteriness, irritability, and feeding difficulties as they go through withdrawal shortly after birth. According to UVA Health, calls to poison centers regarding these issues have skyrocketed.
The Legal Status of Kratom in 2026
As of May 2026, the legal landscape for Kratom remains a patchwork. While it is not currently listed under the federal Controlled Substances Act, the DEA has designated it as a “Drug of Concern.” The FDA has been even more vocal, warning consumers to avoid the product entirely due to the lack of approved medical uses and significant safety risks.
In our local areas, the rules are changing rapidly:
- Tennessee: Recent Tennessee legislation has tightened the reins. While not a total ban, the state has moved to regulate the sale of Kratom more strictly, pursuing further studies on its safety.
- Virginia: Similar to Tennessee, Virginia health departments continue to monitor the substance closely, with some local jurisdictions considering their own restrictions.

Regulatory Concerns and Contaminants
One of the biggest dangers of Kratom isn’t just the plant itself, but what’s in the bottle. Because it isn’t regulated like medicine, the quality varies wildly. The NCCIH has noted several major safety issues:
- Salmonella: There have been multiple outbreaks of Salmonella linked to contaminated powder.
- Heavy Metals: Testing has found high levels of lead and nickel in various products.
- Adulteration: Some “potency-boosted” extracts have been found to contain undeclared synthetic opioids or other drugs to make them feel stronger.
Frequently Asked Questions about Kratom
Is Kratom safe for pain relief or opioid withdrawal?
The FDA’s stance is clear: there is no reliable scientific evidence that Kratom is safe or effective for any medical condition. While many people use it to self-treat, they are often trading one addiction for another. For those seeking help with opioid dependence, medication-assisted treatment using FDA-approved options like Suboxone is a much safer, evidence-based path.
What are the signs of Kratom psychosis?
In cases of chronic, high-dose abuse, some individuals have experienced “Kratom psychosis.” This can manifest as hallucinations (seeing or hearing things that aren’t there), delusions (strong beliefs in things that aren’t true), and extreme confusion or aggression. This is a medical emergency and requires immediate professional intervention.
How many people use Kratom worldwide?
It’s more common than you might think. As of 2020, an estimated 15 million people worldwide use Kratom. In the U.S., a 2021 survey estimated that 1.7 million people aged 12 and older had used it in the past year. The rapid rise in use is reflected in poison control data, which saw a 52-fold increase in reported exposures between 2011 and 2017.
Conclusion
Kratom is often marketed as a harmless, natural supplement, but the reality is far more complicated. Whether you are in Brentwood, TN, or Virginia Beach, VA, it’s important to recognize that this plant has powerful, opioid-like effects that can lead to addiction and serious health complications.
At National Addiction Specialists, we understand the struggle of trying to manage pain or withdrawal on your own. We provide telemedicine-based recovery plans, including medication-assisted treatment, right from the comfort of your home in Tennessee and Virginia. Our goal is to provide confidential, expert care that helps you reclaim your life without the risks of unregulated substances.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








