Counting Sheep Safely While on Suboxone
Sleep Trouble on Suboxone Is More Common Than You Think
Suboxone and sleep aids are a combination that many people in recovery need to think carefully about — because the wrong choice can be dangerous, and the right one can make a real difference.
Here is a quick overview of the safest options:
| Sleep Aid | Type | Safe with Suboxone? |
|---|---|---|
| Low-dose doxepin (3-6mg) | Prescription | Yes — first-line option |
| Ramelteon (8mg) | Prescription | Yes — second-line option |
| Melatonin | OTC supplement | Generally yes, with provider guidance |
| Magnesium glycinate | OTC supplement | Generally yes |
| Valerian root / L-theanine | OTC supplement | Generally yes, short-term |
| Benzodiazepines (e.g., Xanax, Valium) | Prescription | No — serious overdose risk |
| Z-drugs (Ambien, Lunesta) | Prescription | No — respiratory depression risk |
| Alcohol | — | No — dangerous CNS depressant |
| Antipsychotics (e.g., quetiapine) | Prescription | Not recommended |
Sleep problems during opioid recovery are not a sign that something is going wrong. They are actually very common. Studies show that between 70% and 85% of people on opioid maintenance therapy report poor sleep quality. Whether it is trouble falling asleep, waking through the night, vivid dreams, or daytime fatigue — these are real, recognized side effects that deserve a real solution.
The challenge is that not all sleep aids are safe to combine with Suboxone® (buprenorphine/naloxone). Some carry serious risks, including slowed breathing and overdose. Knowing which options are safe — and which to avoid — is essential for anyone navigating recovery.
I’m Chad Elkin, MD, board-certified in Addiction Medicine and founder of National Addiction Specialists, and I’ve spent years helping patients manage the full picture of opioid use disorder — including the complex relationship between suboxone and sleep aids. In the sections below, I’ll walk you through what the evidence says, what’s safe, and what to watch out for.

Suboxone and sleep aids vocabulary:
Why Sleep Disturbances Occur During Recovery
When we start treatment with Suboxone, our brains are essentially going through a massive renovation. For a long time, opioid receptors were flooded with full agonists (like heroin, oxycodone, or fentanyl). Suboxone, which contains buprenorphine and naloxone, steps in to stabilize those receptors, but the transition isn’t always seamless for our internal clock.
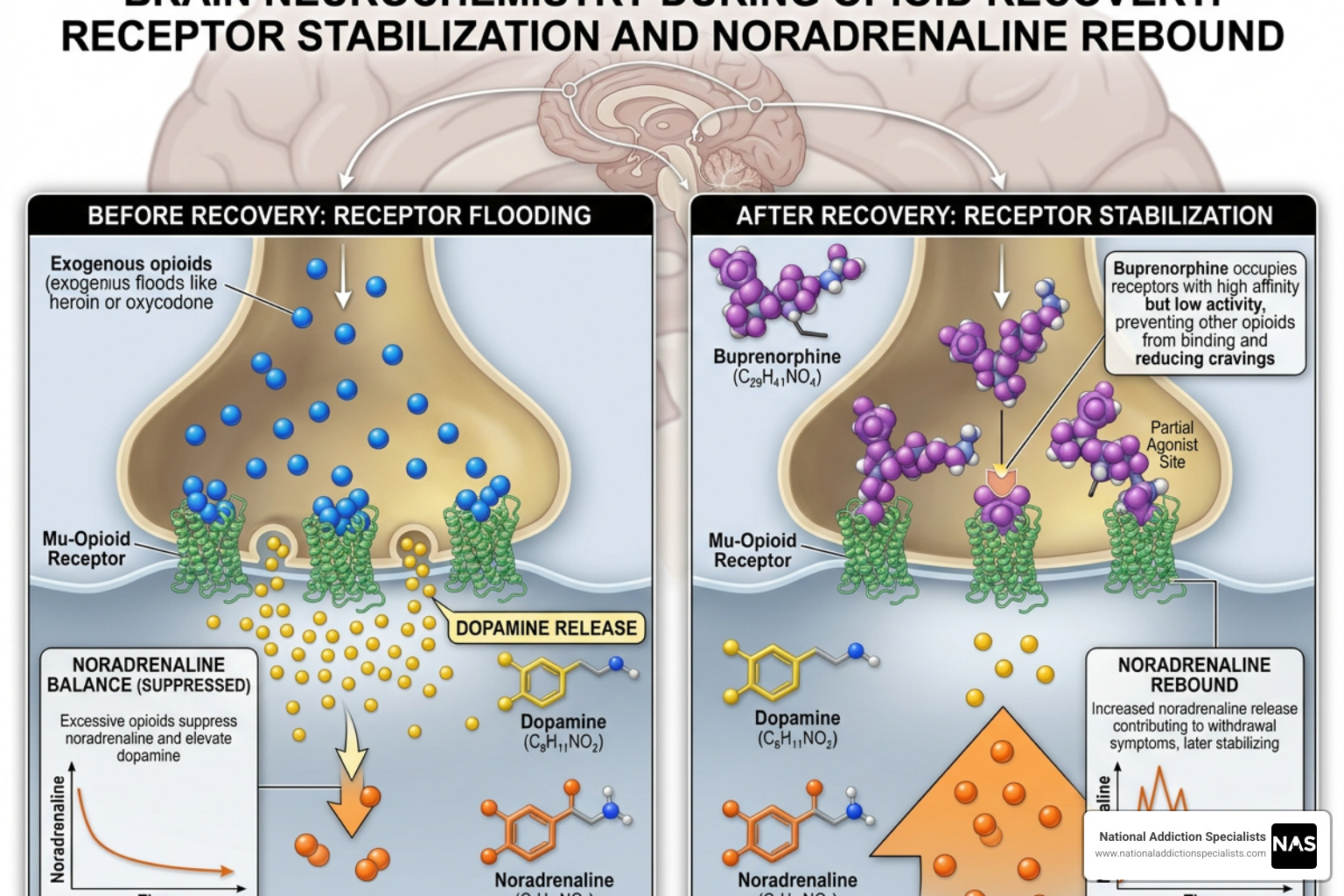
Several scientific factors contribute to why we might toss and turn. Buprenorphine is a partial opioid agonist. While it is much safer than full opioids, it still interacts with the same pathways that regulate sleep and alertness. One key player is noradrenaline. During active use, opioids suppress noradrenaline; when we transition to Suboxone or lower our dose, a “rebound” of noradrenaline can occur, making us feel hyper-alert or restless at night.
Furthermore, research published in Drug and Alcohol Dependence highlights that sleep distress is common across all stages of recovery. Many patients also experience suboxone-withdrawal symptoms early on, such as restless legs or anxiety, which directly interfere with the ability to drift off. It is also worth noting that other suboxone-side-effects like night sweats can make for a very uncomfortable evening.
Impact on Sleep Architecture and Quality
It isn’t just about how long we sleep, but how we sleep. Opioids are notorious for disrupting “sleep architecture” — the natural stages of light and deep sleep we need to feel refreshed. Specifically, buprenorphine can increase sleep latency (the time it takes to fall asleep) and has been shown in studies to reduce both REM (Rapid Eye Movement) and non-REM sleep cycles.
This suppression of REM sleep is why some people report fewer dreams, while others experience incredibly vivid or intense dreams as the body tries to “catch up” on REM sleep. The result is often daytime fatigue, even if you felt like you were in bed for eight hours.
Suboxone and Sleep Apnea Risks
We must also address a more serious concern: disordered breathing. A 2013 study found that 63% of participants taking buprenorphine/naloxone for opioid use disorder had at least mild disordered breathing.
Opioids are central nervous system depressants, which means they can slow down the signal the brain sends to the body to breathe. This can worsen Obstructive Sleep Apnea (where the airway is physically blocked) or lead to Central Sleep Apnea (where the brain “forgets” to signal a breath). If you find yourself gasping for air at night or waking up with a pounding headache, it is vital to discuss these symptoms with us immediately.
Safe and Effective Suboxone and Sleep Aids
The good news is that you don’t have to suffer through sleepless nights. There are several suboxone and sleep aids combinations that are considered safe when managed by a professional.
First-Line Pharmacological Options
When lifestyle changes aren’t enough, we often look at specific medications that have a low risk of interfering with your breathing or your recovery.
- Low-dose Doxepin (3-6mg): This is widely considered the safest first-line prescription option. At these very low doses, it acts primarily as a histamine blocker rather than an antidepressant, helping you stay asleep without significant respiratory risk.
- Ramelteon (8mg): This is a unique prescription medication that mimics melatonin. It has zero abuse potential and doesn’t cause the “hangover” feeling many other sedatives do.
- Melatonin: This natural hormone is a popular choice. Research suggests it is gentle and non-addictive, making it a great starting point for many on Suboxone.
- Magnesium Glycinate: Often used to help with restless legs and muscle tension, magnesium can be a soothing addition to a nighttime routine.
For more detailed answers on common medication questions, you can always check our suboxone-treatment-faq.
Secondary Options for Persistent Insomnia
If the first-line options don’t do the trick, we might consider other non-addictive alternatives:
- Trazodone: While some guidelines suggest caution due to potential side effects, Trazodone is frequently used at low doses because it isn’t a controlled substance and doesn’t typically lead to misuse.
- Hydroxyzine: An antihistamine that also helps with anxiety, it can be useful for those whose racing thoughts keep them awake.
- L-Theanine & Valerian Root: These herbal supplements can offer mild relaxation, but should only be used short-term and after a quick chat with your provider.
Medications and Substances to Avoid
While we want you to sleep, safety is our absolute priority. Certain substances, when mixed with Suboxone, can create a “perfect storm” for respiratory depression.
The Risk of Respiratory Depression
The biggest danger comes from combining Suboxone with other Central Nervous System (CNS) depressants.
- Benzodiazepines (Xanax, Klonopin, Valium): These are the most dangerous to mix with Suboxone. Both drugs slow down the central nervous system, and taking them together significantly increases the risk of a fatal overdose.
- Z-drugs (Ambien, Lunesta): While they aren’t benzos, they work on similar receptors and can still cause dangerous suboxone-and-sleepiness and breathing issues.
- Alcohol: Mixing alcohol with your medication is never safe. It increases sedation and can lead to unpredictable respiratory suppression. If you are struggling with alcohol as well, it is important to understand the impact of alcohol withdrawal on sleep patterns.
Why Antipsychotics Are Not Recommended
In the past, some doctors prescribed quetiapine (Seroquel) for sleep. However, modern guidelines strongly advise against this for insomnia. Antipsychotics can cause significant weight gain, metabolic changes, and can actually worsen restless leg syndrome — the last thing you want when you’re trying to rest.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
Non-Pharmacological Strategies for Better Rest
Sometimes the best “sleep aid” isn’t a pill at all. For those in recovery, retraining the brain to sleep naturally is a powerful tool.
Optimizing Your Sleep Environment
Your bedroom should be a sanctuary for sleep only. We recommend keeping the temperature around 65 degrees Fahrenheit — a cool room signals to your body that it is time to rest. Use blackout curtains to keep the room dark and consider a white noise machine if you live in a noisy area of Brentwood or Virginia Beach.
Crucially, you must limit screen time. The blue light from your phone or TV mimics sunlight, which stops your brain from producing its own melatonin. Try to put the phone away at least an hour before bed.
Lifestyle Habits for Recovery Success
Consistency is king. Try to go to bed and wake up at the same time every day, even on weekends. This helps regulate your circadian rhythm.
- CBT-I (Cognitive Behavioral Therapy for Insomnia): This is the “gold standard” for chronic sleep issues. It teaches you skills to change the thoughts and behaviors that keep you awake. It is highly effective for people in recovery because it involves no drugs and provides long-term results.
- Mindfulness and Meditation: Practices like deep breathing or guided imagery can lower your heart rate and prepare your mind for sleep. You can find many meditation resources online.
- Watch Your Diet: Avoid heavy or spicy meals close to bedtime, and be mindful of caffeine intake. Even a cup of coffee in the afternoon can still be in your system when you’re trying to sleep at 10 PM.
- Movement: Gentle stretching or yoga before bed can release physical tension.
If you are transitioning from other substances, you might wonder how long does alcohol withdrawal last or how it affects these habits; generally, the sooner you establish these routines, the better your long-term sleep will be.
Frequently Asked Questions about Suboxone and Sleep Aids
Are natural suboxone and sleep aids effective?
Yes, for many people, natural options like melatonin and magnesium are very effective. They are often preferred because they don’t carry the same risks of dependency or respiratory depression as prescription sedatives. However, “natural” doesn’t always mean “safe for everyone,” so always check with us before starting a new supplement.
When to ask your doctor about suboxone and sleep aids?
If your insomnia lasts more than a few weeks, or if it is affecting your ability to function during the day, it is time to talk. We can look at your Suboxone dose — sometimes taking your medication earlier in the morning can help. We also want to ensure that underlying issues like depression or anxiety are being treated, as these are major drivers of sleep problems. You can also explore SAMHSA treatment resources for additional support.
Does sleep improve over time on Suboxone?
Absolutely. One of the most encouraging studies showed that sleep disturbance scores improved significantly after 90 days of buprenorphine/naloxone treatment. As your brain stabilizes and the symptoms of early recovery fade, your natural sleep patterns often return. Recovery is a marathon, not a sprint, and your sleep will likely get better as you continue your journey.
Conclusion
At National Addiction Specialists, we know that getting a good night’s rest is a vital part of your recovery. If you are struggling with suboxone and sleep aids, you don’t have to figure it out alone. We provide personalized, telemedicine-based care across Tennessee and Virginia, including Brentwood and Virginia Beach.
Our goal is to help you find the balance you need to stay healthy, safe, and well-rested. Whether you need to adjust your medication or explore non-drug options like CBT-I, we are here to support every step of your recovery.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.