Yes, You Can Withdraw From Suboxone: A Complete Guide
Understanding Suboxone Withdrawal: What You Need to Know

Can you withdraw from Suboxone? Yes, you can withdraw from Suboxone, and understanding the process is crucial for anyone considering stopping this medication. While Suboxone (buprenorphine/naloxone) is an effective treatment for opioid dependence, it can cause withdrawal symptoms when discontinued.
Quick Answer:
- Withdrawal is possible when stopping Suboxone
- Symptoms typically last 7-10 days for physical symptoms, up to 30 days for psychological symptoms
- Gradual tapering under medical supervision is safest
- Cold turkey cessation can be dangerous and increases relapse risk
- Professional guidance significantly improves success rates
Withdrawal from Suboxone happens because your body has adapted to the medication. When you stop taking it suddenly, your system needs time to readjust. The good news? With proper medical support and a structured tapering plan, you can safely discontinue Suboxone and minimize uncomfortable symptoms.
The severity and duration of withdrawal varies from person to person. Factors like your dosage, how long you’ve been taking Suboxone, and your overall health all play a role. Physical symptoms generally peak within the first 72 hours and resolve within 10 days, while psychological symptoms like cravings and depression may persist for a month or longer.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists. Through my work treating thousands of patients with substance use disorders, I’ve guided many individuals through the question of can you withdraw from Suboxone safely and successfully, developing personalized tapering protocols that minimize discomfort and maximize long-term recovery outcomes. This guide will walk you through everything you need to know about safely withdrawing from Suboxone, from understanding the timeline to managing symptoms effectively.
Handy can you withdraw from suboxone terms:
Can You Withdraw From Suboxone Safely?
The journey to recovery from opioid use disorder often involves medication-assisted treatment (MAT) with Suboxone. This medication, a combination of buprenorphine and naloxone, plays a crucial role in stabilizing individuals and reducing cravings and withdrawal symptoms from other opioids. However, when the time comes to discontinue Suboxone, the question naturally arises: can you withdraw from Suboxone safely and effectively? The answer is a resounding yes, but the key lies in a carefully planned and medically supervised approach.

Attempting to stop Suboxone abruptly, often referred to as “cold turkey,” carries significant risks and is strongly discouraged. Instead, a gradual tapering schedule guided by a healthcare professional is the safest and most effective method. This measured approach allows your body and brain to slowly adjust to decreasing levels of the medication, minimizing the intensity and duration of withdrawal symptoms.
Here are the critical aspects to consider regarding safe Suboxone withdrawal:
- Medical Supervision is Essential: Never attempt to withdraw from Suboxone without the guidance of a qualified medical professional. This is paramount to your safety and success. Our team at National Addiction Specialists, serving patients across Tennessee and Virginia, specializes in creating personalized tapering plans that prioritize your well-being.
- Tapering, Not Cold Turkey: A slow, controlled reduction in dosage is the gold standard for Suboxone cessation. This helps mitigate severe withdrawal symptoms and reduces the likelihood of relapse.
- Individualized Plans: Every person’s journey is unique. Your medical history, duration of Suboxone use, dosage, and any co-occurring mental health conditions will all influence your personalized tapering schedule.
The Dangers of Quitting Cold Turkey
While the desire to be free from all medications is understandable, quitting Suboxone cold turkey can lead to a host of unpleasant and potentially dangerous consequences. These risks often outweigh any perceived benefits of a rapid cessation.
Here are some of the primary dangers associated with abruptly stopping Suboxone:
- Severe Withdrawal Symptoms: Abrupt discontinuation can trigger intense and prolonged opioid withdrawal symptoms. Because buprenorphine (the active opioid component in Suboxone) is long-acting, withdrawal symptoms can be delayed in onset but can also be more protracted and severe than with shorter-acting opioids. These symptoms can include profound physical discomfort and significant psychological distress, making the experience incredibly challenging and increasing the risk of early failure.
- Precipitated Withdrawal: While Suboxone contains naloxone to deter misuse, taking Suboxone too soon after using a full opioid agonist can cause precipitated withdrawal, which is very rapid and intense. Similarly, if Suboxone is misused (e.g., injected), the naloxone can induce immediate and severe withdrawal. While this is less likely when discontinuing prescribed Suboxone, the body’s reaction to sudden removal of the partial agonist can still be harsh.
- High Risk of Relapse: The intense discomfort of unsupervised cold turkey withdrawal significantly increases the likelihood of relapse to illicit opioid use. When faced with severe symptoms, the temptation to use opioids to alleviate the pain becomes incredibly strong. Relapse after Suboxone withdrawal is particularly dangerous because your opioid tolerance will have decreased. This means that using the same amount of opioids you once did can easily lead to a fatal overdose.
- Exacerbated Psychological Distress: The psychological symptoms of withdrawal, such as anxiety, depression, and irritability, are often more severe with abrupt cessation. This can trigger or worsen pre-existing mental health conditions, creating a vicious cycle that makes sustained recovery incredibly difficult.
The Benefits of a Supervised Taper
A medically supervised tapering schedule is not just the safer option; it’s the smarter path to long-term success when asking can you withdraw from Suboxone. This approach is designed to minimize discomfort and provide the necessary support for a lasting recovery.
Here’s why a supervised taper is so beneficial:
- Minimizes Withdrawal Symptoms: By gradually reducing the dosage over time, your body has the opportunity to adapt to lower levels of buprenorphine. This significantly lessens the intensity of both physical and psychological withdrawal symptoms, making the process much more manageable. While some discomfort is often unavoidable, a taper aims to keep it at a tolerable level.
- Stabilizes Brain Chemistry: Opioids, including buprenorphine, affect the brain’s reward system and neurotransmitter balance. A slow taper allows your brain chemistry to gradually re-regulate, helping to prevent the severe imbalances that contribute to intense cravings and mood disturbances during abrupt withdrawal. This gradual adjustment supports the natural healing process of your brain.
- Reduces Relapse Risk: Because the withdrawal experience is less severe and more controlled, the urge to relapse is significantly diminished. You’re better equipped to manage any residual discomfort and focus on building healthy coping mechanisms rather than being overwhelmed by intense cravings.
- Provides Medical Support: During a supervised taper, your healthcare provider can prescribe additional medications, such as clonidine or Lucemyra (lofexidine hydrochloride), to further alleviate specific withdrawal symptoms like nausea, muscle aches, or restlessness. This targeted symptomatic relief is a cornerstone of comfortable withdrawal.
- Integrates Behavioral Therapy and Counseling: Our approach at National Addiction Specialists emphasizes that medication is just one part of the recovery puzzle. A supervised taper is often integrated with addiction counseling services and behavioral therapies. This comprehensive support addresses the underlying psychological aspects of addiction, helping you develop coping strategies, manage triggers, and build a strong foundation for long-term sobriety. We believe that without therapy, sustained abstinence can be incredibly challenging.
- Flexible and Personalized: Tapering schedules are not one-size-fits-all. While some schedules might last 7 to 28 days, the best approach is often flexible and custom to your individual response. Your provider will work with you, adjusting the taper rate based on how you feel and how well your symptoms are managed, ensuring a comfortable and effective process.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
https://www.nationaladdictionspecialists.com/new-patient-packet/
The Suboxone Withdrawal Timeline and Symptoms
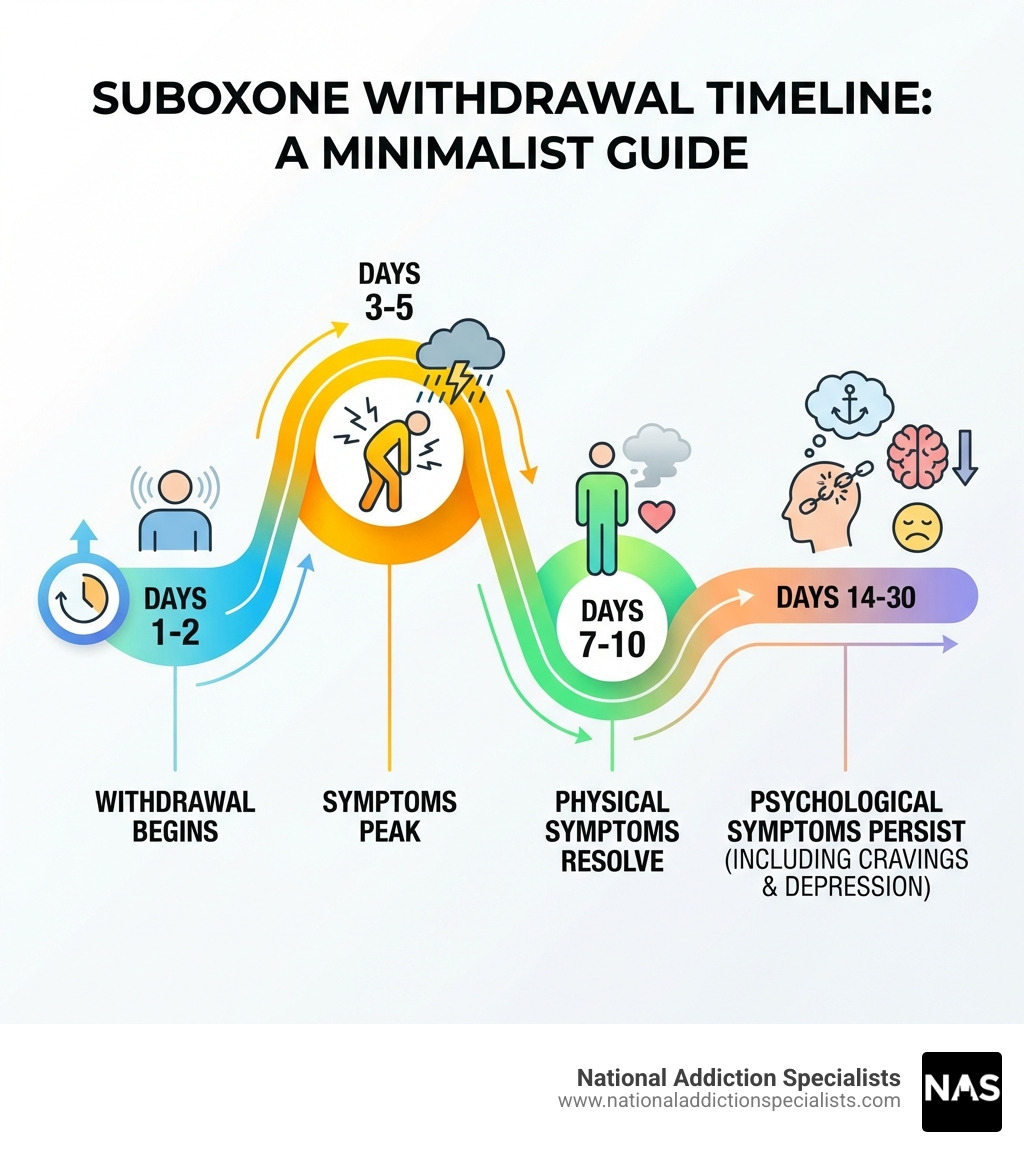
Understanding the timeline and typical symptoms of Suboxone withdrawal can help you prepare for the process and know what to expect. While individual experiences vary, there’s a general pattern to how symptoms unfold.
Here’s a general overview:
| Symptom Category | Onset | Peak | Duration (Typical) |
|---|---|---|---|
| Physical | 24-72 hours after last dose | Days 3-5 | 7-10 days |
| Psychological | Days 2-4, often intensifies later | Weeks 2-4 | 1 month or longer |
Physical Symptoms of Suboxone Withdrawal
The physical symptoms of Suboxone withdrawal are often compared to a severe flu. They typically begin within 24 to 72 hours after your last dose, peak around days three to five, and generally subside within 7 to 10 days. The first 72 hours are usually the most challenging for physical discomfort.
Common physical symptoms include:
- Nausea and Vomiting: Often accompanied by stomach cramps and digestive distress like diarrhea.
- Muscle Aches and Body Aches: Widespread discomfort, feeling like your bones ache.
- Insomnia: Difficulty falling or staying asleep, restless sleep.
- Sweating and Chills: Alternating sensations of being hot and cold, often with goosebumps.
- Headaches: Ranging from mild to severe.
- Lethargy and Fatigue: Feeling extremely tired and lacking energy.
- Runny Nose and Watery Eyes: Similar to cold symptoms.
- Restlessness and Tremors: An inability to sit still, twitching, or shaking.
Healthcare professionals often use the Clinical Opiate Withdrawal Scale (COWS) for symptom assessment to objectively measure the severity of withdrawal and guide treatment. This tool helps ensure that your tapering plan is effective and that any discomfort is adequately managed.
Psychological Challenges and Drug Cravings
While the acute physical symptoms usually resolve within the first week to ten days, the psychological challenges of Suboxone withdrawal can persist much longer. Psychological dependence and cravings are significant problems that often last for a month or longer after stopping Suboxone. This is a critical period that requires ongoing support to prevent relapse.
Common psychological symptoms and challenges include:
- Anxiety: Feelings of unease, worry, or nervousness.
- Depression: Low mood, loss of interest in activities, and feelings of hopelessness. Depression is particularly common during the second week of withdrawal and can persist for weeks or even months.
- Irritability and Agitation: Feeling easily annoyed, frustrated, or restless.
- Concentration Difficulties: Trouble focusing, brain fog, or impaired cognitive function.
- Drug Cravings: Intense urges or desires to use opioids. These cravings can be powerful and are a primary driver of relapse.
- Mood Swings: Rapid and unpredictable changes in emotional state.
- Guilt and Regret: These feelings can be particularly strong and may be linked to past behaviors related to addiction.
This extended period of psychological symptoms and cravings highlights why long-term support, including therapy and counseling, is so vital. Without addressing these underlying issues, the risk of relapse remains high, even after the physical discomfort has passed.
How to Manage Suboxone Withdrawal Symptoms Effectively
Navigating Suboxone withdrawal can be challenging, but with the right strategies and support, it’s a journey you can successfully complete. Effective management combines professional medical care with personal coping mechanisms and lifestyle adjustments.
Professional Medical Management
The cornerstone of successful Suboxone withdrawal is professional medical management. Our team at National Addiction Specialists in Tennessee and Virginia provides comprehensive medication-assisted treatment (MAT) programs that include supervised tapering and ongoing support.
Here’s what professional medical management entails:
- Physician Guidance: A qualified physician will assess your individual situation, including your history of Suboxone use, dosage, and overall health, to develop a personalized tapering schedule. This schedule will gradually reduce your Suboxone dose over weeks or months, allowing your body to adjust.
- Medication to Ease Symptoms: Your doctor may prescribe non-opioid medications to alleviate specific withdrawal symptoms. For example, clonidine can help reduce anxiety, muscle aches, sweating, and restlessness. Lucemyra (lofexidine hydrochloride) is another FDA-approved non-opioid medication specifically designed to manage opioid withdrawal symptoms and can be started immediately after your last Suboxone dose.
- Regular Monitoring: Throughout the tapering process, your medical team will regularly monitor your symptoms, adjust your medication as needed, and provide emotional support. This close supervision ensures your safety and comfort.
- Integrated Treatment Plan: At National Addiction Specialists, we believe in a holistic approach. Your medical management will be integrated with behavioral therapy and counseling to address the psychological aspects of addiction and build sustainable coping strategies.
Holistic and Alternative Therapies
Beyond medical interventions, incorporating holistic and alternative therapies can significantly improve your comfort and well-being during Suboxone withdrawal and throughout your recovery. These approaches complement traditional treatment by supporting your physical and mental health.
Consider incorporating the following:
- Exercise: Regular, mild to moderate physical activity can help manage restlessness, improve mood, and promote better sleep. Even a daily walk can make a difference.
- Nutrition: A balanced, nutritious diet is crucial for supporting your body during withdrawal. Staying hydrated and eating regular, healthy meals can help stabilize blood sugar and energy levels.
- Animal-Assisted Therapy: For some, interacting with animals can provide comfort, reduce anxiety, and promote a sense of connection.
- Mindfulness and Relaxation Techniques: Practices like meditation, deep breathing exercises, and yoga can help manage anxiety, reduce stress, and improve concentration.
- Artistic Therapies: Engaging in creative activities like painting, writing, or music can be a powerful outlet for processing emotions and reducing stress.
- Peer Support Groups: Joining groups like Narcotics Anonymous (NA) or other peer support networks provides a sense of community, shared experience, and accountability. The 12-Step structure, for example, has proven beneficial for millions.
Here’s a list of lifestyle adjustments that can aid in your recovery:
- Stay Hydrated: Drink plenty of water and clear fluids.
- Eat Balanced Meals: Focus on nutrient-rich foods to support your body’s healing.
- Regular Sleep Schedule: Even if sleep is difficult, try to maintain a consistent bedtime and wake-up time.
- Engage in Hobbies: Distract yourself with activities you enjoy.
- Seek Social Support: Connect with trusted friends, family, or support groups.
- Practice Self-Care: Take warm baths, listen to calming music, or engage in other relaxing activities.
- Avoid Other Substances: Steer clear of alcohol and other drugs, as they can worsen withdrawal symptoms and increase relapse risk.
Special Considerations: Pregnancy and Long-Term Recovery
When asking can you withdraw from Suboxone, certain situations require even more careful consideration, such as pregnancy. Additionally, understanding the long-term aspects of recovery is vital for sustained sobriety.
Can You Withdraw From Suboxone During Pregnancy?
Withdrawing from Suboxone during pregnancy presents unique challenges and risks that must be carefully managed by specialized medical professionals. While the goal is always the health of both mother and baby, abrupt withdrawal from any opioid, including Suboxone, can pose significant dangers to the fetus.
- Risks of Abrupt Withdrawal to the Fetus: Rapid or unsupervised withdrawal during pregnancy can lead to severe stress on the fetus, potentially causing premature labor, fetal distress, or even miscarriage.
- Neonatal Opioid Withdrawal Syndrome (NOWS): If a mother continues to use opioids (including buprenorphine) throughout pregnancy, the baby may experience Neonatal Opioid Withdrawal Syndrome (NOWS) after birth. While NOWS is an expected and treatable condition, it requires specialized medical care for the newborn.
- Specialized Medical Care: Generally, Suboxone itself is not recommended during pregnancy. Instead, buprenorphine (without naloxone) or methadone are often considered safer alternatives for medication-assisted treatment during pregnancy, as they have a more established safety profile for the fetus and can help manage NOWS more effectively. The decision to switch medications or attempt a taper during pregnancy must be made in close consultation with an obstetrician and an addiction medicine specialist. The primary goal is to maintain stability for the mother to ensure the best possible outcome for the baby.
- Scientific research on treating opioid use disorder during pregnancy highlights the importance of continued, medically supervised treatment throughout pregnancy to prevent relapse and ensure better outcomes for both mother and child.
Factors Influencing Withdrawal Severity
The experience of Suboxone withdrawal is highly individualized. Several factors can significantly influence the duration and severity of your symptoms. Understanding these can help you and your medical team prepare a more effective and supportive withdrawal plan.
Key factors include:
- Dosage Levels: Higher daily doses of Suboxone generally lead to more intense and prolonged withdrawal symptoms. The body has become more accustomed to a larger amount of buprenorphine, requiring a slower, more gradual taper.
- Duration of Use: The longer you have been taking Suboxone, the more physically dependent your body may have become. Long-term use often necessitates a more extended tapering schedule to allow for adequate physiological adjustment.
- Concurrent Alcohol or Other Drug Use: Using alcohol or other drugs alongside Suboxone can complicate the withdrawal process, intensify symptoms, and increase the risk of adverse effects. It can also mask or exacerbate underlying conditions.
- Presence of Other Medical Conditions: Pre-existing medical conditions can affect your body’s ability to cope with withdrawal. For example, chronic pain or gastrointestinal issues might be worsened during withdrawal.
- Co-occurring Mental Health Disorders: Individuals with mental health disorders such as anxiety, depression, or PTSD may experience more severe psychological withdrawal symptoms. These conditions can be exacerbated during withdrawal, making psychological support and therapy even more critical. Our team at National Addiction Specialists is equipped to provide comprehensive care that addresses both your substance use disorder and any co-occurring mental health challenges.
- Individual Metabolism: Each person metabolizes medication differently. Factors like genetics, age, and liver function can influence how quickly buprenorphine is processed and eliminated from your system, affecting the onset and duration of withdrawal.
Given these variables, a personalized approach is essential when you can you withdraw from Suboxone. Your treatment plan should be custom to your unique circumstances to ensure the safest and most comfortable withdrawal possible.
Frequently Asked Questions about Suboxone Withdrawal
We understand you likely have many questions about Suboxone withdrawal. Here, we address some of the most common concerns.
How long do the physical symptoms last?
The acute physical symptoms of Suboxone withdrawal typically begin within 24 to 72 hours after your last dose, peak around days three to five, and generally resolve within seven to ten days. While this period can be uncomfortable, it is temporary. Psychological symptoms, however, such as depression and cravings, can last for a month or longer.
Is it possible to avoid withdrawal symptoms entirely?
While it’s highly unlikely to avoid all withdrawal symptoms entirely when asking can you withdraw from Suboxone, a medically supervised and gradual tapering schedule can significantly minimize their intensity and make them much more manageable. The goal of a professional taper is to keep you as comfortable as possible, rather than eliminating symptoms entirely, which is often unrealistic. Our expert providers at National Addiction Specialists work diligently to ensure your comfort throughout the process.
What is the risk of relapse after stopping Suboxone?
The risk of relapse after stopping Suboxone is notably high, particularly in the month following cessation. This is largely due to persistent drug cravings and lingering psychological symptoms like depression. Furthermore, if you do relapse, the danger is amplified because your opioid tolerance will have significantly decreased. This means that taking the same amount of opioids you used before treatment could lead to a dangerous or fatal overdose. This is why continued therapy, counseling, and a strong support system are crucial for long-term recovery after Suboxone withdrawal.
Conclusion
The question, can you withdraw from Suboxone, is one that many individuals face on their path to long-term recovery from opioid use disorder. While the prospect of withdrawal can be daunting, it is absolutely possible to steer this transition safely and effectively with the right support. The key lies in understanding the process, avoiding the dangers of abrupt cessation, and embracing a medically supervised tapering plan.
At National Addiction Specialists, we are committed to providing compassionate, comprehensive care for individuals seeking to withdraw from Suboxone and achieve lasting sobriety. Our telemedicine-based approach allows us to deliver personalized recovery plans directly to your home, offering convenience and confidentiality. With expert providers specializing in medication-assisted treatment and counseling, we serve patients across Tennessee and Virginia, accepting Medicaid and Medicare to ensure access to vital care.
We understand that recovery is a journey, not a destination. Our team will work with you every step of the way, providing the guidance, support, and resources you need to manage withdrawal symptoms, develop coping strategies, and build a strong foundation for a fulfilling, opioid-free life. You don’t have to face this challenge alone.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.





