What to Expect: Navigating Suboxone Withdrawal Symptoms
Understanding What Happens When You Stop Taking Suboxone
What are the withdrawal symptoms of suboxone? When you stop taking Suboxone, you may experience both physical and psychological symptoms as your body adjusts to the absence of the medication.
Common Suboxone withdrawal symptoms include:
Physical Symptoms:
- Nausea and vomiting
- Muscle aches and pains
- Headaches
- Sweating and chills
- Insomnia and fatigue
- Digestive problems
- Fever
- Runny nose and teary eyes
Psychological Symptoms:
- Anxiety and restlessness
- Depression
- Irritability and mood swings
- Drug cravings
- Difficulty concentrating
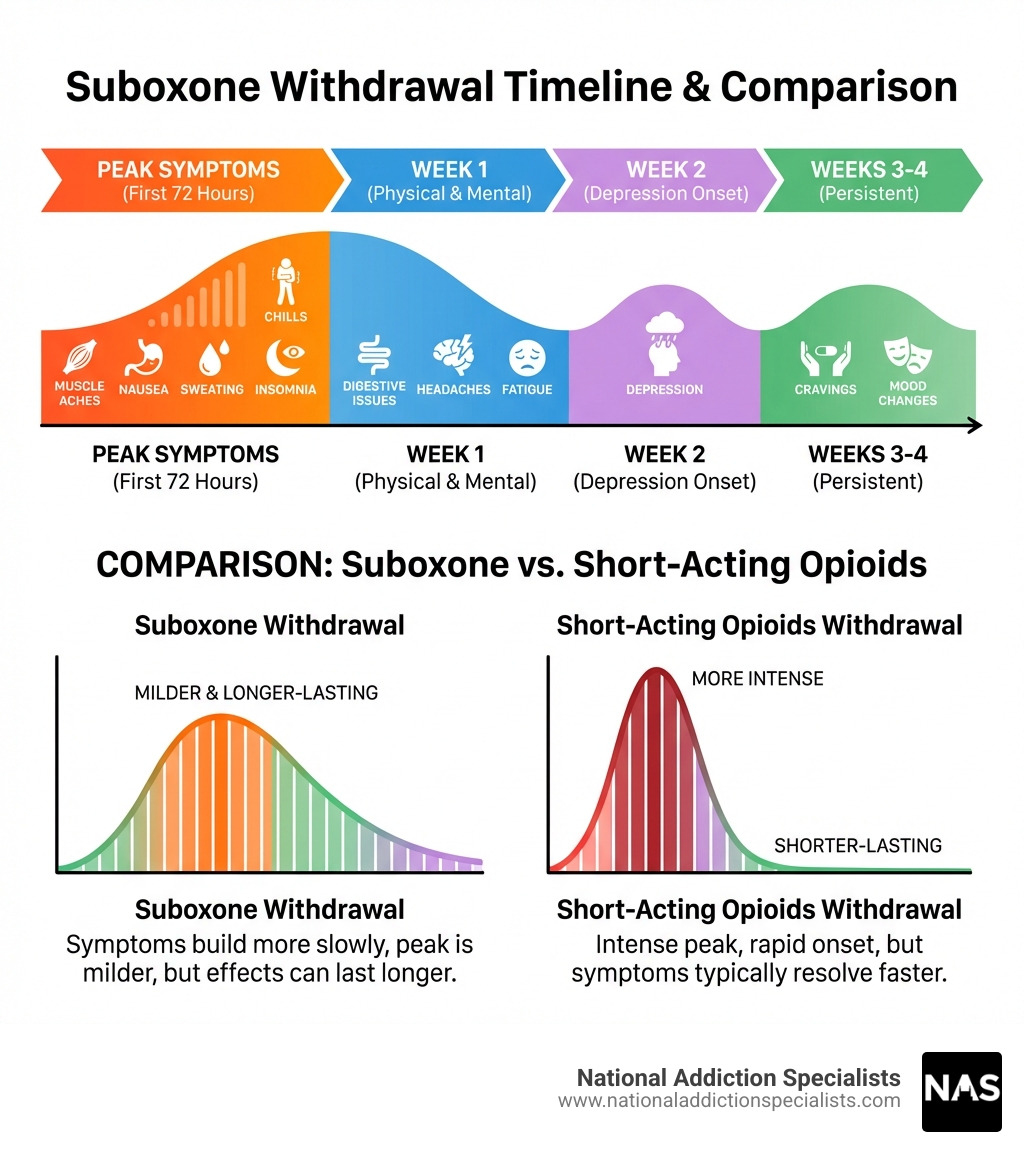
Timeline:
- Symptoms typically begin 2-4 days after your last dose
- Peak around days 3-5
- Physical symptoms usually resolve within 7-10 days
- Psychological symptoms like cravings and depression may persist for several weeks or longer
Nobody talks enough about what it feels like facing these symptoms. It’s rough. Nights feel endless with insomnia despite exhaustion. Mood swings can take you from fine to angry or tearful over small things.
The good news? Withdrawal from Suboxone is typically milder than withdrawal from full opioid agonists like heroin or oxycodone, thanks to buprenorphine’s unique properties as a partial opioid agonist. The symptoms build more slowly but can last longer, especially the emotional effects.
As Dr. Chad Elkin, founder and Medical Director of National Addiction Specialists with board certification in Addiction Medicine, I’ve helped countless patients steer what are the withdrawal symptoms of suboxone safely through medically supervised tapering and comprehensive support. Understanding what to expect is your first step toward managing the process with confidence and minimizing discomfort.
Glossary for what are the withdrawal symptoms of suboxone:
Understanding Suboxone and Why Withdrawal Occurs
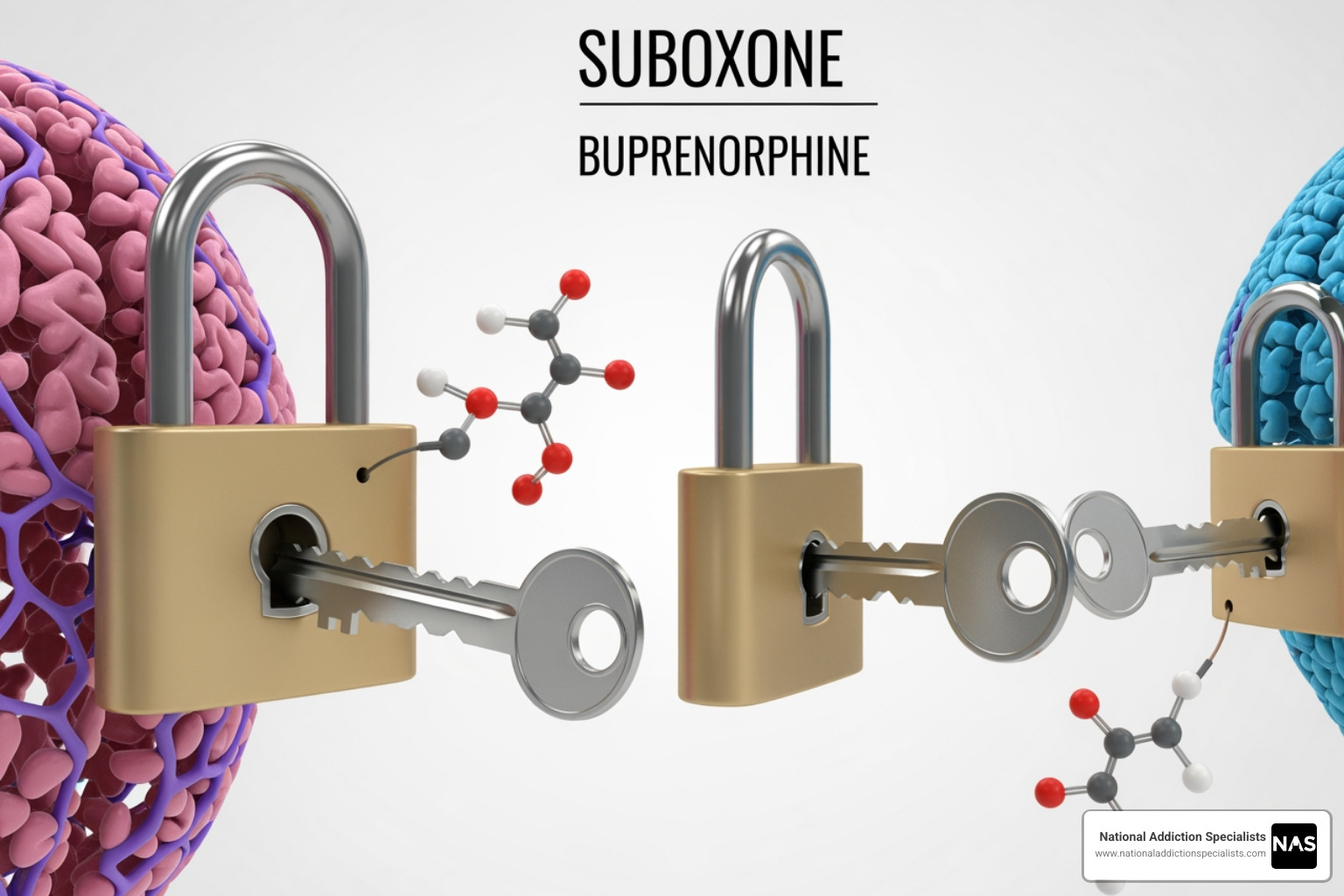
To understand why we feel so “off” when we stop Suboxone, we first have to look at what the medication is actually doing in our brains. Suboxone is a combination of two medicines: buprenorphine and naloxone. It is designed to help us stay stable and healthy by reducing or stopping the use of other, more dangerous opioids.
Buprenorphine is what we call a partial agonist. Think of your brain’s opioid receptors like locks. Full agonists—like heroin or oxycodone—turn the key all the way, causing a massive rush of dopamine and a high. Buprenorphine only turns the key halfway. It occupies the lock, satisfying the craving and preventing withdrawal, but it doesn’t provide the intense euphoria. This is known as the “ceiling effect,” meaning that after a certain point, taking more buprenorphine doesn’t increase its effects, which makes it much safer than traditional opioids.
However, even though it’s a partial agonist, our brains still develop a physical dependence on it over time. When we take Suboxone daily, our brain chemistry adjusts to its presence. If we stop suddenly, those “locks” are suddenly empty, and the brain sends out SOS signals—these are the withdrawal symptoms we dread.
The Role of Buprenorphine and Naloxone
The second half of the Suboxone equation is Naloxone. This ingredient is added specifically to prevent misuse. If someone tries to crush and inject Suboxone, the naloxone kicks in and immediately blocks the opioid receptors, causing “precipitated withdrawal”—which is essentially an instant, very intense version of withdrawal. When taken correctly (dissolved under the tongue), the naloxone isn’t absorbed well, and the buprenorphine does its job.
This unique combination is why Suboxone side effects are generally manageable, but it’s also why stopping “cold turkey” can be so difficult. Your body has learned to rely on that “half-turn” of the key to feel normal.
What are the withdrawal symptoms of suboxone?
When we talk about what are the withdrawal symptoms of suboxone, we are looking at a spectrum of experiences. Because Suboxone stays in your system longer than heroin or morphine, the symptoms don’t usually hit you the second you miss a dose. Instead, they creep up.
Medical professionals often use the Clinical Opiate Withdrawal Scale (COWS) to measure how intense these symptoms are. This scale looks at things like heart rate, sweating, pupil size, and bone or joint aches to determine the severity of the opioid withdrawal.
Physical and Early What Are the Withdrawal Symptoms of Suboxone
The physical side of withdrawal can feel like a particularly nasty case of the flu. In the early stages, you might notice:
- Muscle Aches and Pain: Your body might feel heavy, and your joints might ache. This is often one of the first signs that the medication is leaving your receptors.
- Digestive Distress: Nausea, vomiting, and stomach cramps are common. Your digestive system is “waking up” from the slowing effects of opioids.
- Temperature Issues: You might alternate between shivering with chills and sweating through your clothes.
- Insomnia and Fatigue: You’ll likely feel exhausted, but sleep will remain elusive. This “tired but wired” feeling is a hallmark of Suboxone withdrawal.
- Dilated Pupils and Runny Nose: Physical signs that your autonomic nervous system is overreacting.
Psychological and Emotional What Are the Withdrawal Symptoms of Suboxone
While the physical symptoms are tough, many of our patients at National Addiction Specialists find the psychological symptoms even more challenging. These include:
- Anxiety and Restlessness: You might feel like you’re vibrating or that you can’t sit still (this is sometimes called “skin crawling”).
- Depression: As your brain’s dopamine levels struggle to rebalance, a deep sense of sadness or hopelessness can set in, particularly in the second week.
- Irritability: Small annoyances can feel like major catastrophes.
- Drug Cravings: The urge to take something to make the discomfort stop can be very strong. This is why Suboxone withdrawal treatment is so important—it provides the tools to fight these urges.
The Suboxone Withdrawal Timeline: What to Expect
The Suboxone withdrawal timeline is different for everyone, but it generally follows a predictable pattern. Because buprenorphine has a long half-life (meaning it stays in your body for a long time), you won’t feel the full force of withdrawal immediately.
| Phase | Timing | Primary Symptoms |
|---|---|---|
| Onset | Days 1–2 | Mild anxiety, restlessness, beginning of runny nose/tears. |
| Acute Peak | Days 3–5 | Nausea, sweating, muscle aches, insomnia, peak physical discomfort. |
| Early Subsidence | Days 7–10 | Physical symptoms begin to fade; fatigue and mood swings remain. |
| PAWS Phase | Week 2–Month 1 | Depression, drug cravings, sleep disturbances, irritability. |
The First 72 Hours
During the first three days, the medication is slowly detaching from your receptors. You might feel “okay” for the first 24 hours, but by the 48-hour mark, the physical discomfort usually begins in earnest. This is the period where most people are at risk for relapse if they aren’t in a supportive environment. If you find yourself in crisis, the SAMHSA National Helpline is a vital resource.
Weeks Two Through Four
By the second week, the “flu-like” symptoms usually start to pack their bags, but the mental battle continues. This is often when depression peaks. Your brain is essentially learning how to produce its own “feel-good” chemicals again, and that takes time. Cravings can stick around for a month or longer, which is why we emphasize long-term counseling and support.
Strategies to Manage and Minimize Symptoms
The best way to handle what are the withdrawal symptoms of suboxone is to avoid the “cold turkey” approach altogether. At National Addiction Specialists, we focus on a personalized, telemedicine-based approach that allows you to recover in the comfort of your own home in Tennessee or Virginia.
Medical Interventions and Support
We strongly recommend a medical taper. Learning how to taper off Suboxone under professional supervision is the gold standard for success. By slowly lowering the dose over weeks or even months, we give the brain time to adjust, which can make the withdrawal symptoms significantly milder.
We may also use “comfort medications” to help:
- Clonidine: A blood pressure medication that is excellent at reducing anxiety, sweating, and restlessness.
- Lucemyra: The first non-opioid FDA approved treatment specifically for managing opioid withdrawal symptoms.
- Counseling and Therapy: Addressing the “why” behind the addiction is just as important as managing the “what” of the symptoms.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
Lifestyle and Home Remedies
While medical support is key, there are things you can do at home to ease the transition:
- Hydration: Withdrawal often involves sweating and digestive issues, which can lead to dehydration. Drink plenty of water and electrolyte-rich beverages.
- Balanced Diet: Small, bland meals (like the BRAT diet: bananas, rice, applesauce, toast) can help if you’re experiencing nausea.
- Exercise: It sounds like the last thing you want to do when you’re tired, but a short walk can help release natural endorphins.
- Sleep Hygiene: Try to keep a regular schedule, avoid caffeine in the afternoon, and use relaxation techniques like deep breathing or meditation.
- Social Support: Whether it’s a 12-step meeting or just a trusted friend, don’t do this alone.
Frequently Asked Questions about Suboxone Withdrawal
Is Suboxone withdrawal worse than other opioids?
This is a bit of a “yes and no” answer. Withdrawal from short-acting opioids like heroin is often more intense—the symptoms hit like a freight train but are over relatively quickly. Because Suboxone is long-acting, the symptoms are generally milder but they last longer. For some, the duration makes it feel more difficult, while for others, the lower intensity makes it more manageable.
What are the risks of quitting cold turkey?
Quitting cold turkey is not recommended. The primary risk is relapse; when the symptoms become unbearable, the brain’s first instinct is to find relief through opioids. Because your tolerance drops during withdrawal, a relapse can easily lead to a fatal overdose. Furthermore, the extreme physical stress of cold turkey withdrawal can be dangerous for people with underlying health conditions. We always encourage checking our New Patient Packet to start a safer, supervised journey.
How long should I stay on Suboxone?
There is no “one-size-fits-all” answer to how long should I stay on Suboxone? Some people use it for a few months as a bridge to sobriety, while others remain on maintenance therapy for years. The goal is stability. We work with you to decide when—and if—tapering is right for your specific life situation.
Conclusion
Navigating what are the withdrawal symptoms of suboxone is a challenge, but it is a temporary one. With the right medical guidance, a slow taper, and a strong support system, you can move through this phase and into a life of long-term recovery.
At National Addiction Specialists, we are dedicated to making this process as smooth as possible. Our telemedicine services in Tennessee and Virginia mean you don’t have to worry about the stigma of a clinic or the stress of travel. We provide confidential, expert care that includes both medication management and the emotional support you need to succeed. Whether you are in Brentwood, Virginia Beach, or anywhere across TN and VA, we are here to help.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








