What to Expect During Long Term Effects of Suboxone Withdrawal
What Are the Long Term Effects of Suboxone Withdrawal?
The long term effects of Suboxone withdrawal go well beyond the first week of physical discomfort — and for many people, the psychological aftermath is the harder part to survive.
Here’s a quick overview of what to expect:
| Phase | Timeframe | Key Symptoms |
|---|---|---|
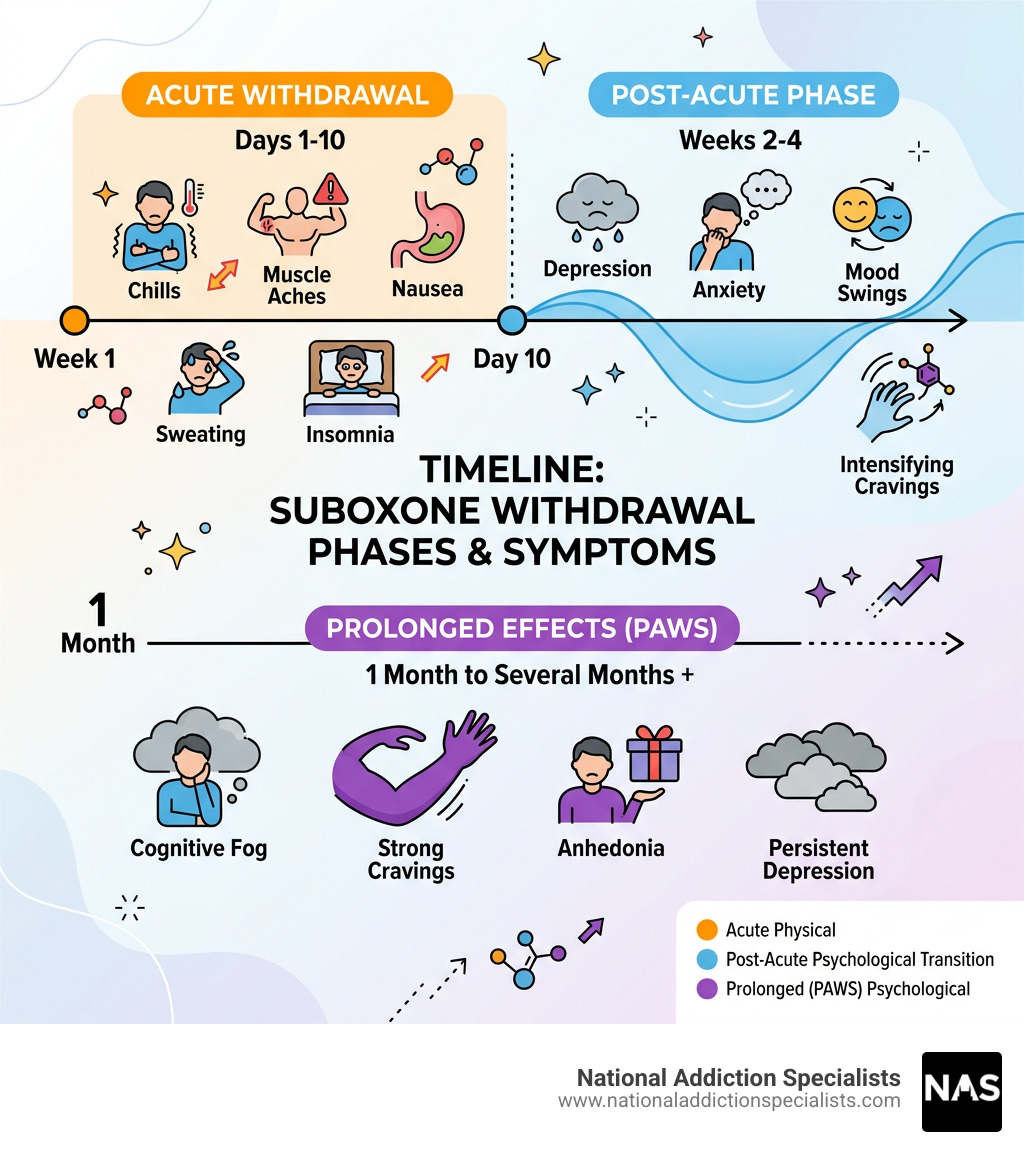
| Acute withdrawal | Days 1-10 | Muscle aches, nausea, sweating, chills, insomnia |
| Post-acute phase | Weeks 2-4 | Depression, anxiety, mood swings, intensifying cravings |
| Prolonged effects (PAWS) | 1 month to several months | Persistent depression, cognitive fog, strong cravings, anhedonia |
Most physical symptoms clear up within the first month. But psychological symptoms — especially depression and drug cravings — can linger for months, and in some cases, opioid cravings have been reported years after stopping the medication.
This is what makes Suboxone withdrawal different from many other opioid withdrawals. Because Suboxone is long-acting, with a half-life of up to 60 hours, the withdrawal process is slower and more drawn out than with short-acting opioids like heroin. The one-month mark is often described as one of the most vulnerable periods — physical symptoms have faded, but intense cravings and depression make relapse risk especially high.
I’m Chad Elkin, MD, board-certified in Addiction Medicine and founder of National Addiction Specialists — I’ve helped hundreds of patients navigate the long term effects of Suboxone withdrawal safely through medically supervised tapering and individualized treatment plans. In the sections below, I’ll walk you through exactly what to expect and how to protect your recovery.
Understanding the Long Term Effects of Suboxone Withdrawal
When we talk about the long term effects of Suboxone withdrawal, we are often referring to a phenomenon known as Post-Acute Withdrawal Syndrome (PAWS). While the first few days of quitting any opioid involve a “flu-like” physical battle, PAWS is a marathon, not a sprint. It represents the brain’s struggle to return to a baseline state of health after being accustomed to the presence of buprenorphine.
Suboxone works by binding to the same receptors in the brain as other opioids, but it does so as a partial agonist. This means it provides stability without the intense “high” of heroin or fentanyl. However, over time, the brain adjusts its chemistry to account for the medication. When the medication is removed, especially if it is done too quickly, the brain experiences a period of neurochemical chaos.
This process involves neuroplasticity — the brain’s ability to reorganize itself. Healing takes time. During this period, the brain’s “reward system” is essentially offline. This is why many people feel “flat” or unable to experience joy during the months following their last dose. Understanding how Suboxone treatment works is the first step in realizing why the transition away from it requires such care.
Scientific research, such as studies on buprenorphine tapering and illicit opioid use, highlights that a structured approach is vital. Without a medically managed plan, the brain doesn’t get the “slow landing” it needs to stabilize its chemistry, leading to more severe opioid withdrawal symptoms that can last much longer than expected.
Why Long Term Effects of Suboxone Withdrawal Last Longer Than Other Opioids
You might wonder why someone can detox from heroin in about ten days, yet Suboxone users often report feeling “off” for a month or more. The answer lies in the drug’s half-life.
The “half-life” is the amount of time it takes for half of the substance to leave your bloodstream. While heroin has a very short half-life (leaving the body quickly and causing intense, immediate withdrawal), buprenorphine has a half-life of 24 to 60 hours. This means it stays in your system for a long time, creating a “steady-state” in your plasma.
Because it leaves the body so slowly, the onset of withdrawal is delayed — sometimes not even starting until 2 to 4 days after the last dose. Consequently, the entire withdrawal timeline is stretched out.
| Opioid Type | Typical Half-Life | Acute Withdrawal Duration |
|---|---|---|
| Heroin (Short-acting) | Minutes to 2-3 hours | 5-10 days |
| Oxycodone (Short-acting) | 3-5 hours | 7-10 days |
| Suboxone (Long-acting) | 24-60 hours | 20-30+ days |
This extended duration is why we often see the long term effects of Suboxone withdrawal persist. The body is processing the drug for weeks, not days. If you are in Tennessee or Virginia and feeling overwhelmed by this timeline, you don’t have to face it alone.
Common Psychological Symptoms of Long Term Effects of Suboxone Withdrawal
While the physical symptoms like muscle aches and nausea usually subside within the first week or two, the psychological symptoms can be much more persistent. These are the hallmarks of the long term effects of Suboxone withdrawal:
- Anhedonia: This is the inability to feel pleasure. Things that used to make you happy — like a good meal, a hobby, or spending time with family — may feel meaningless. This happens because the brain’s dopamine receptors are still recalibrating.
- Prolonged Depression: After the second week, depression often becomes the most significant symptom. It can feel heavy and all-consuming, often peaking around the one-month mark.
- Generalized Anxiety: Many people experience a baseline level of “jitters” or a constant sense of unease that can last for several weeks.
- Intense Cravings: These are often strongest when the depression is at its worst. The brain “remembers” that opioids provided a quick fix for these low feelings, leading to a high risk of relapse.
- Cognitive Fog: You might find it hard to concentrate, remember simple tasks, or feel “sharp” at work. This mental cloudiness is a common part of the brain’s healing process.
- Sleep Disturbances: Insomnia or poor-quality sleep can persist for months, which in turn makes the anxiety and depression harder to manage.
For more detailed information on what to watch out for, you can read about Suboxone side effects.

Factors Influencing the Severity of Prolonged Withdrawal
Not everyone experiences the long term effects of Suboxone withdrawal in the same way. Several factors determine how long and how intense your journey will be:
- Dosage Levels: Individuals on higher daily doses (such as 16mg or 32mg) generally face a more challenging withdrawal than those on lower maintenance doses.
- Duration of Treatment: The longer you have been on Suboxone, the more “set” your brain chemistry has become. Long-term use (over six months) is associated with more persistent PAWS.
- Tapering Speed: This is perhaps the most critical factor. Quitting “cold turkey” or tapering too fast (e.g., over just a few days) almost guarantees more severe long-term effects.
- Biological Factors: Your metabolism, age, and overall physical health play a role in how quickly your body clears the medication and repairs itself.
- Co-occurring Mental Health Disorders: If you struggled with depression or anxiety before starting Suboxone, these symptoms are likely to return with greater intensity during withdrawal.
At National Addiction Specialists, we take all these factors into account when creating your personalized plan. If you have questions about your specific situation, our Suboxone treatment FAQ is a great resource.
Risks of Quitting Cold Turkey vs. Medical Tapering
We cannot stress this enough: quitting Suboxone “cold turkey” is not recommended. While it might seem tempting to “just get it over with,” the risks are significant.
First, there is the relapse risk. When withdrawal symptoms become unbearable — especially the intense psychological depression — many people return to illicit opioids just to make the pain stop.
Second, there is the danger of a fatal overdose. After a period of abstinence, your body’s tolerance for opioids drops significantly. If a relapse occurs and you take the same dose of heroin or fentanyl you used to take, your body may not be able to handle it, leading to a life-threatening respiratory failure.
Third, there is the risk of precipitated withdrawal if you try to cycle back and forth between medications without professional guidance.
Expert-recommended tapering guidelines suggest a gradual reduction. This allows the brain to slowly adjust to lower levels of the drug, minimizing the “shock” to the system. There are many benefits of Suboxone treatment for opioid addiction, but the greatest benefit comes from finishing the journey safely under a doctor’s care.
Managing the Long Term Effects of Suboxone Withdrawal Safely
If you’re ready to move toward a life without Suboxone, the best way to do it is through a direct taper. This involves slowly reducing your dose — often by only 5% to 10% every few weeks — until you reach the lowest possible amount before stopping.
Here is how we help manage the process:
- Clinical Supervision: We monitor your symptoms in real-time. If the withdrawal becomes too intense, we can pause the taper or adjust the dose to keep you stable.
- Behavioral Therapy: Counseling is essential for managing the depression and anxiety that come with PAWS. It helps you build the coping skills needed to stay sober when cravings hit.
- Support Groups: Connecting with others who understand the long term effects of Suboxone withdrawal can reduce the isolation that often leads to relapse.
- Nutritional Support: A healthy diet and hydration can actually help your brain repair its neurochemistry faster.
- Alternative Medications: In some cases, non-opioid medications like clonidine or Lucemyra can be used to manage specific symptoms like high blood pressure or anxiety during the taper.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
Frequently Asked Questions about Suboxone Withdrawal
Are there permanent or irreversible effects from Suboxone withdrawal?
The good news is that the brain is remarkably resilient. While the long term effects of Suboxone withdrawal can feel permanent while you are in the thick of them, research shows that neurobiological recovery is possible. Over time, your brain will begin to produce its own endorphins again, and your receptors will return to a more natural state. Cognitive restoration — the clearing of the “fog” — generally happens as your sleep and mood stabilize.
How long does the depression from Suboxone withdrawal typically last?
This varies, but most patients see a significant improvement after the first 30 to 60 days. While the first month is the “delicate time” where depression is most intense, the following months usually involve a gradual lifting of the cloud. Complete dopamine and serotonin regulation can take several months to a year, depending on the length of your prior opioid use.
When should I seek professional medical help for persistent symptoms?
You should seek help immediately if you experience:
- Thoughts of self-harm or severe suicidal ideation.
- Cravings that feel impossible to manage on your own.
- A “relapse trigger” that you don’t feel equipped to handle.
- Physical symptoms that prevent you from eating, drinking, or sleeping for extended periods.
Professional intervention is not a sign of failure; it is a tool for success.
Conclusion
Navigating the long term effects of Suboxone withdrawal is a challenging journey, but it is one that leads to true freedom. At National Addiction Specialists, we provide telemedicine-based care across Tennessee and Virginia, including Brentwood and Virginia Beach. We offer personalized, confidential recovery plans that you can access from the comfort and privacy of your own home.
We accept Medicaid and Medicare, ensuring that expert care is accessible to those who need it most. Whether you are just starting your journey or are looking for a safe way to taper off your current medication, we are here to support you every step of the way.
Start your recovery journey today and let us help you move toward a brighter, healthier future.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.







