Understanding What Happens When You Stop Suboxone
The suboxone withdrawal symptoms timeline is a critical piece of information for anyone considering stopping this medication. Here’s what you need to know:
Quick Timeline Overview:
| Timeframe | Key Symptoms |
|---|---|
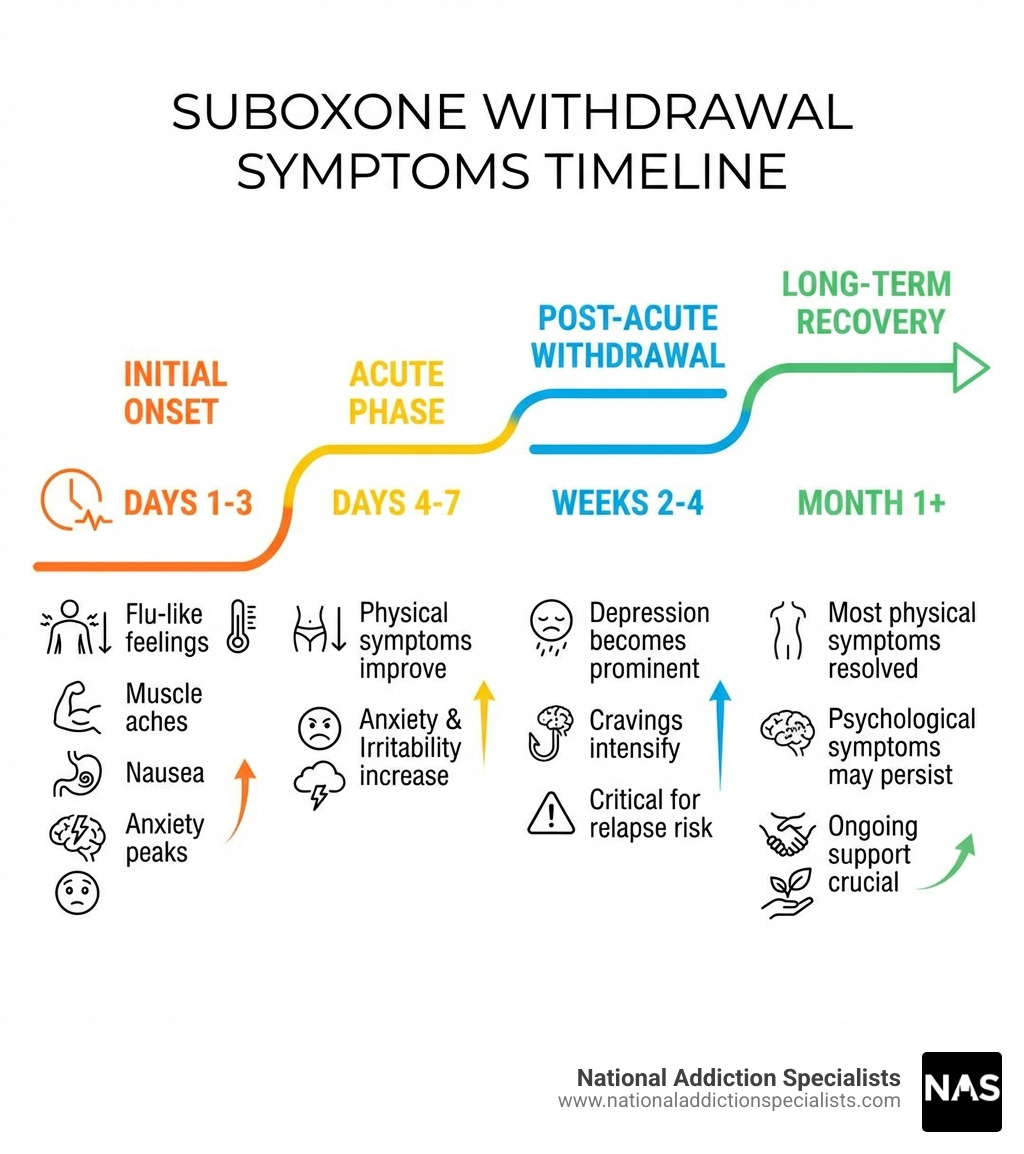
| Days 1-3 | Symptoms begin within 24-72 hours; flu-like feelings, muscle aches, nausea, anxiety peak |
| Days 4-7 | Physical symptoms start improving; psychological symptoms like anxiety and irritability increase |
| Weeks 2-4 | Depression becomes prominent; cravings intensify; critical period for relapse risk |
| Month 1+ | Most physical symptoms resolved; psychological symptoms may persist for months |
Suboxone, a combination of buprenorphine and naloxone, has helped countless people manage opioid use disorder through medication-assisted treatment (MAT). But because your body adapts to its regular presence, stopping the medication—especially abruptly—triggers withdrawal symptoms. These symptoms occur as your brain’s chemistry readjusts to functioning without the medication.
What makes Suboxone withdrawal unique is its timeline. Unlike short-acting opioids where withdrawal hits within hours, Suboxone’s long-acting nature means symptoms typically begin 2-4 days after your last dose and can last significantly longer—sometimes up to a month or more for psychological symptoms. The first 72 hours are usually the most physically intense, but the emotional and mental challenges that follow can be just as difficult.
Understanding this timeline helps you prepare, plan, and succeed. Many people describe withdrawal as feeling like a severe flu combined with intense mood changes and cravings. But with the right support and a medically supervised approach, you can steer this journey safely and comfortably.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists. Over my years of treating patients, I’ve helped countless individuals successfully steer the suboxone withdrawal symptoms timeline through personalized, evidence-based care. My goal is to help you understand what to expect and how to manage each phase of this process.
Suboxone withdrawal symptoms timeline terms at a glance:
Common Suboxone Withdrawal Symptoms
Starting on the journey of Suboxone withdrawal means preparing for a range of physical and psychological challenges. Understanding these symptoms is the first step in managing them effectively and ensuring a smoother path to recovery. While the experience can be intense, it is temporary and manageable with proper support.
Physical Symptoms
When your body begins to adjust to the absence of Suboxone, you may experience a variety of physical symptoms, often likened to a severe flu. These are your body’s way of recalibrating its systems.
Common physical symptoms include:
- Flu-like symptoms: This is a broad category encompassing several uncomfortable sensations. You might experience a fever, chills, and excessive sweating, sometimes accompanied by a runny nose or teary eyes.
- Muscle aches and body pains: Many individuals report widespread muscle aches and joint pain, which can range from mild discomfort to significant agony. Restlessness in the limbs is also common.
- Nausea and vomiting: Gastrointestinal distress is a hallmark of opioid withdrawal. Nausea can be persistent, often leading to vomiting.
- Diarrhea and stomach cramps: Your digestive system may become overactive, leading to diarrhea and painful abdominal cramps or indigestion.
- Insomnia: Despite feeling utterly exhausted, falling and staying asleep can become a significant challenge, further exacerbating other symptoms.
- Lethargy and fatigue: A profound sense of tiredness and lack of energy often accompanies withdrawal, making even simple tasks feel monumental.
- Headaches: Persistent or throbbing headaches are also frequently reported.
- Overactive reflexes and dilated pupils: Your nervous system can become hypersensitive, leading to exaggerated reflexes and pupils that appear larger than usual. Goosebumps (piloerection) are also a classic sign, often referred to as “cold turkey.”
Psychological Symptoms
Beyond the physical discomfort, the psychological aspects of Suboxone withdrawal can be equally, if not more, challenging. These symptoms affect your mood, thoughts, and emotional well-being.
Common psychological symptoms include:
- Anxiety: A pervasive feeling of unease, worry, or nervousness is very common. This anxiety can range from mild to severe, sometimes leading to panic attacks.
- Depression: Feelings of sadness, hopelessness, and a loss of interest in activities you once enjoyed are frequently reported. This can be particularly challenging and may persist for some time after acute withdrawal.
- Irritability and mood swings: You might find yourself easily agitated, quick to anger, or experiencing rapid shifts in mood.
- Difficulty concentrating: Mental fog, an inability to focus, and trouble with memory or decision-making can make daily tasks difficult.
- Intense cravings: The brain’s powerful desire for the drug can lead to strong urges to use Suboxone or other opioids, posing a significant risk for relapse.
- Agitation and restlessness: A feeling of inner turmoil and an inability to sit still can be incredibly distressing.
Some psychological symptoms, particularly anxiety and depression, can persist even after the acute physical withdrawal phase has resolved. This is sometimes referred to as protracted withdrawal, and it requires continued support and treatment to manage effectively. For more information on this, we can look to resources like the Substance Abuse and Mental Health Services Administration (SAMHSA) on Protracted Withdrawal.
The Suboxone Withdrawal Symptoms Timeline: A Day-by-Day Guide
Understanding the suboxone withdrawal symptoms timeline is crucial for anyone preparing to discontinue the medication. Because Suboxone is a long-acting opioid, its withdrawal timeline differs significantly from that of short-acting opioids like heroin or oxycodone. Symptoms appear more slowly and can last longer, often for weeks or even months in some cases. This extended duration is primarily due to buprenorphine’s long half-life, which means it stays in your system longer.

Let’s break down the typical progression of symptoms:
Days 1-3: The Acute Phase Begins
This initial period marks the onset and peak of many physical withdrawal symptoms.
- Onset of symptoms: Due to Suboxone’s long half-life, physical symptoms of Suboxone withdrawal typically appear within 6–12 hours for some, but more commonly begin within 24 to 72 hours after your last dose. This delayed onset can sometimes catch individuals off guard if they expect immediate withdrawal like with short-acting opioids.
- Peak intensity: Suboxone withdrawal symptoms tend to peak around day two or within the first 72 hours. This is often the most challenging period, where physical discomfort is at its worst.
- Symptoms: You can expect intense flu-like feelings including chills, fever, profuse sweating, and muscle aches. Gastrointestinal problems such as nausea, vomiting, and diarrhea are very common. Insomnia, headaches, and a general feeling of lethargy will also likely be present. Increased heart rate, blood pressure, and significant anxiety or restlessness are also prominent during this acute phase.
Days 4-7: Physical Symptoms Subside, Psychological Symptoms Emerge
As you move past the initial peak, you’ll likely notice a shift in the nature of your symptoms.
- Transition phase: Physical symptoms often begin to resolve and decrease in intensity during days three to five. While some lingering body aches and general discomfort might persist, the worst of the flu-like symptoms typically start to diminish.
- Decreased physical intensity: By the end of the first week, most of the severe physical symptoms should have subsided, leaving behind more general aches and pains.
- Increased psychological symptoms: As the physical discomfort lessens, psychological symptoms often become more pronounced. You might experience increased anxiety, heightened irritability, and significant mood swings. Difficulty concentrating and persistent cravings for Suboxone or other opioids are also common during this time. This period is crucial for maintaining a stable and supportive environment, as emotional distress can be high.
Weeks 2-4: Navigating Lingering Symptoms
This period is often characterized by the persistence of psychological symptoms, even as most physical discomfort fades.
- Post-acute withdrawal (PAWS): While not everyone experiences PAWS, this phase can feel like a marathon. Most physical withdrawal symptoms will generally subside after one month, but psychological dependence can still remain.
- Depression as a key challenge: After the second week, depression often becomes the biggest symptom. Feelings of sadness, hopelessness, loss of interest in activities, fatigue, low energy, changes in appetite or weight, and trouble with memory or decision-making can be prevalent.
- Persistent insomnia: Sleep disturbances can continue to be a major issue, contributing to fatigue and irritability.
- Cravings can intensify: Even as the acute phase passes, intense drug cravings can persist, especially after one month. This period is critical for relapse prevention, as the desire to alleviate psychological discomfort can be strong.
Month 1 and Beyond: The Path to Stabilization
Even after the first month, the journey isn’t always over.
- Most physical symptoms resolved: By this point, nearly all physical symptoms of suboxone withdrawal symptoms timeline should have resolved.
- Psychological symptoms may persist: However, psychological symptoms like anxiety, depression, and insomnia can linger for weeks to months. After one month, individuals may still experience persistent depression and intensified drug cravings, which can be particularly challenging. This is where understanding and managing post-acute withdrawal syndrome (PAWS) becomes essential.
- Learning coping mechanisms: Successfully navigating this extended period requires developing robust coping strategies and engaging in ongoing therapeutic support.
- Importance of ongoing support: The one-month period is particularly challenging for individuals in recovery. Having strong support systems, access to counseling or therapy, and effective coping strategies are vital to steer these ongoing challenges. For additional insight into this extended phase, you can explore resources on Post-Acute Withdrawal Syndrome (PAWS).
Safely Managing Withdrawal: Tapering and Professional Support
Attempting to quit Suboxone “cold turkey” is not recommended due to severe discomfort, potential health risks, and a significantly high risk of relapse. A medically supervised taper is the safest and most effective method for navigating the suboxone withdrawal symptoms timeline. This approach allows your body to gradually adjust, minimizing the intensity of withdrawal and increasing your chances of long-term success.
Factors Influencing Your Suboxone Withdrawal Symptoms Timeline
The suboxone withdrawal symptoms timeline is not a one-size-fits-all experience. Several individual factors can significantly influence the duration and intensity of your withdrawal:
- Dosage amount: Higher daily doses of Suboxone typically lead to more severe and prolonged withdrawal symptoms.
- Duration of Suboxone use: The longer you have been taking Suboxone, the more physically dependent your body may have become, potentially extending the withdrawal period.
- Individual metabolism: Each person’s body processes medication differently, affecting how quickly Suboxone is cleared from their system.
- Co-occurring mental health conditions: Pre-existing conditions like anxiety, depression, or other mental health disorders can exacerbate psychological withdrawal symptoms and make the process more challenging. It can also be difficult to distinguish between withdrawal symptoms and underlying conditions after the first month.
- Polysubstance use: If you have been using other substances alongside Suboxone (e.g., alcohol, benzodiazepines), withdrawal can be more complex and potentially dangerous.
- Overall physical health: Your general health, including any chronic illnesses, nutritional status, and hydration levels, can impact your body’s ability to cope with withdrawal.
The Role of Medically Supervised Detox
Given the complexities and potential severity of Suboxone withdrawal, medically supervised detox is highly recommended. Our telemedicine-based Suboxone treatment, available in Tennessee and Virginia, offers convenient and confidential care.
Here’s why professional guidance is so crucial:
- Safety and comfort: Our expert medical team can monitor your vital signs, assess your symptoms, and intervene if complications arise, ensuring your safety throughout the process. We can also provide medications to alleviate discomfort, making withdrawal much more tolerable.
- Tapering schedules: We work with you to develop a personalized, gradual tapering schedule that slowly reduces your Suboxone dose over weeks or months. This precision minimizes withdrawal symptoms, allowing your body to adjust incrementally. Studies suggest that a slow, flexible tapering schedule is often the most effective.
- Symptom management: Our providers can prescribe medications to target specific withdrawal symptoms, such as anti-nausea drugs, sleep aids, or non-opioid medications for pain and anxiety. This comprehensive approach helps manage both physical and psychological distress.
- Reduced relapse risk: Attempting to detox at home without supervision carries a high risk of relapse due to uncontrolled cravings and unmanageable symptoms. Medically supervised detox provides the support and structure needed to successfully steer this vulnerable period and significantly lowers the likelihood of returning to opioid use. Experts recommend detoxing under medical supervision to ensure safety and increase the likelihood of success.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Medications and Coping Strategies
While medical supervision and tapering are foundational, several medications and coping strategies can further ease your journey through the suboxone withdrawal symptoms timeline.
Here’s a list of helpful strategies:
- Medications for symptoms: Your doctor may prescribe non-opioid medications to alleviate specific withdrawal symptoms. These can include clonidine, which helps regulate functions of the central nervous system and can reduce anxiety, sweating, and muscle aches. Lucemyra (lofexidine hydrochloride) is another FDA-approved non-opioid medication specifically designed to treat opioid withdrawal symptoms, and it can be started immediately after your last Suboxone dose.
- Over-the-counter relief: For milder symptoms, over-the-counter options like ibuprofen or acetaminophen for pain, ginger ale or anti-nausea medications for stomach upset, and anti-diarrheals can provide some relief. Multivitamins are also recommended to support overall health.
- Hydration and nutrition: Your body is working hard during withdrawal, and proper hydration is key, especially if you’re experiencing vomiting or diarrhea. Eating healthfully, even small, bland meals, provides essential nutrients and energy.
- Light exercise: Engaging in mild to moderate physical activity, such as walking or gentle stretching, can be incredibly beneficial. Studies have shown that exercise boosts endorphins, the brain’s “feel-good” chemicals, which can improve mood and reduce restlessness.
- Mindfulness and relaxation techniques: Practices like deep breathing, meditation, yoga, or progressive muscle relaxation can help manage anxiety, agitation, and insomnia.
- Building a support system: Connecting with trusted friends, family, or support groups provides emotional encouragement and helps you feel less alone. Social interaction and making time for enjoyable activities can also be powerful distractions and mood boosters.
Special Considerations for Pregnancy
Suboxone treatment during pregnancy is a complex issue that requires careful medical consideration. It is generally not recommended for pregnant individuals to undergo opioid withdrawal, including from Suboxone, as it can pose risks to both the parent and the developing fetus.
- Risks of withdrawal during pregnancy: Abruptly stopping Suboxone or experiencing severe withdrawal symptoms can lead to complications such as preterm labor, fetal distress, or miscarriage.
- Importance of medical consultation: If you are pregnant or breastfeeding and taking Suboxone, it is imperative to consult with your doctor. They can assess your individual situation and determine the safest course of action.
- Alternatives: Often, buprenorphine without naloxone or methadone are considered safer alternatives for medication-assisted treatment during pregnancy, as they can stabilize the parent and minimize withdrawal risks for the newborn. The goal is to maintain stability and prevent illicit opioid use, which carries higher risks. For comprehensive guidance, refer to NIDA’s information on treating OUD during pregnancy.
Frequently Asked Questions about Suboxone Withdrawal
We understand you likely have many questions about the suboxone withdrawal symptoms timeline and what to expect. Here, we address some of the most common concerns.
How long do acute Suboxone withdrawal symptoms last?
Acute physical symptoms are typically most intense for the first 72 hours (days 1-3) after your last dose. While some physical discomfort may linger, the most severe physical symptoms generally subside significantly within 7-10 days. However, it’s crucial to remember that psychological symptoms like anxiety, depression, and cravings can persist for weeks or even months beyond this initial acute phase.
How does Suboxone withdrawal compare to withdrawal from other opioids?
Suboxone withdrawal differs from withdrawal from other opioids primarily due to its long-acting nature. With short-acting opioids like heroin or certain prescription painkillers, withdrawal symptoms can begin within 6-12 hours after the last dose and typically resolve within about a week.
In contrast, Suboxone withdrawal has a delayed onset, usually starting 2-4 days after your last dose, because the buprenorphine stays in your system longer. Furthermore, symptoms associated with Suboxone withdrawal generally last longer than other opioids—often for several weeks to a month or more—due to buprenorphine’s long half-life. While the physical symptoms may be less acutely severe than abrupt cessation of a full opioid agonist, their prolonged duration can be challenging.
Can I stop Suboxone “cold turkey”?
We strongly advise against attempting to stop Suboxone “cold turkey.” Quitting abruptly dramatically increases the risk of experiencing severe, often unmanageable, withdrawal symptoms. This intense discomfort not only makes the process incredibly difficult but also significantly raises the likelihood of relapse, which can be particularly dangerous due due to decreased opioid tolerance.
While some data suggests Suboxone withdrawal might last less than a week when stopped cold turkey, the uncontrolled cravings and severe symptoms often lead to relapse. A gradual, medically supervised taper is the safest and most effective method, allowing your body to adjust slowly and minimizing the intensity and duration of withdrawal symptoms. This approach also provides the necessary medical and psychological support to steer the process successfully.
Your Path Forward: Life After Withdrawal
Completing Suboxone withdrawal is a monumental achievement, but the journey to long-term recovery continues. The focus now shifts to preventing relapse and building a fulfilling, substance-free life. This involves ongoing therapy, support groups, and healthy lifestyle choices. With a telemedicine-based approach, National Addiction Specialists offers convenient, confidential, and expert care from the comfort of your home in Tennessee and Virginia, helping you maintain your recovery with a personalized plan.
Find out if our program is right for you.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.









