The Road Less Traveled: Understanding Subutex Withdrawal
What You Need to Know About Subutex Withdrawal
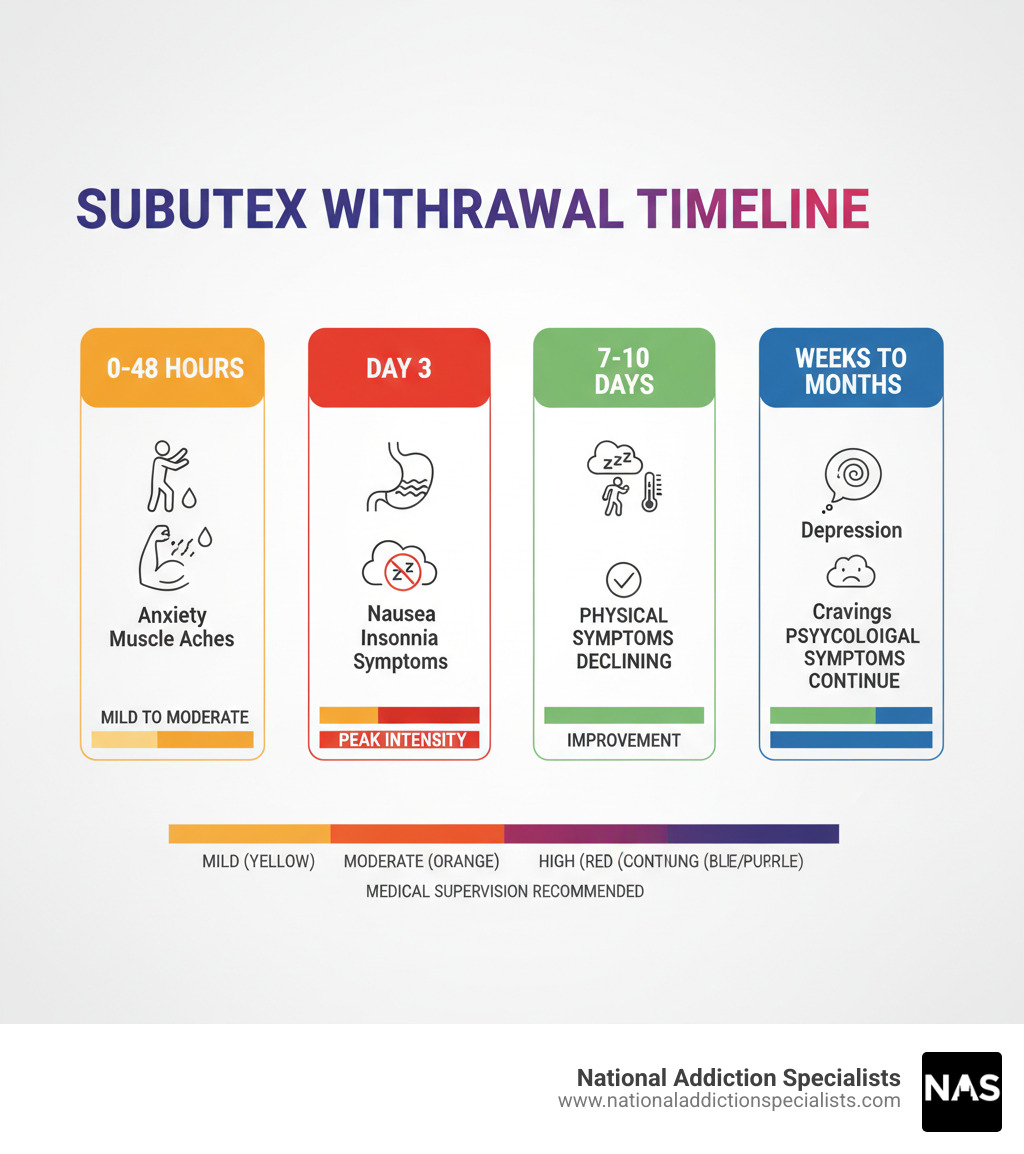
Subutex withdrawal occurs when you stop taking buprenorphine after your body has become physically dependent on it. Here’s what to expect:
| Timeline | What Happens |
|---|---|
| 24-48 hours | Symptoms begin (anxiety, muscle aches, sweating) |
| Day 3 | Peak intensity (flu-like symptoms, nausea, insomnia) |
| 7-10 days | Physical symptoms subside |
| Weeks to months | Psychological symptoms may continue (cravings, depression) |
Common symptoms include:
- Muscle aches and cramping
- Nausea, vomiting, diarrhea
- Anxiety and irritability
- Insomnia and fatigue
- Depression and intense cravings
Important: While Subutex withdrawal is generally milder than withdrawal from full opioid agonists like heroin, it lasts longer. Medical supervision is strongly recommended because the risk of relapse is high, and stopping “cold turkey” can lead to severe symptoms.
Subutex contains buprenorphine, a partial opioid agonist used for opioid use disorder. It binds to opioid receptors, partially activating them to reduce cravings and withdrawal symptoms without the intense high of full opioids.
Your body adapts to buprenorphine, and stopping suddenly causes withdrawal as your brain rebalances. Physical dependence on Subutex can develop over time, which is different from addiction. It means your body has adjusted to the drug, and its removal triggers withdrawal as your system readjusts.
While Subutex withdrawal is less intense than from heroin or fentanyl, it can last longer, with challenging psychological symptoms like depression and cravings. As an addiction medicine physician, I’ve seen that with proper medical support and a structured tapering plan, patients can successfully manage withdrawal and move forward in their recovery journey.
Glossary for subutex withdrawal:
Understanding Subutex: A Tool for Opioid Dependence
Subutex contains buprenorphine, an FDA-approved medication that is a lifeline for many with opioid use disorder. As part of Medication-Assisted Treatment (MAT), it helps reduce cravings and avoid painful Opioid Withdrawal Symptoms.
As a partial opioid agonist, buprenorphine attaches to the same brain receptors as full opioids (like heroin) but only partially activates them. This prevents withdrawal and cravings without causing the intense euphoria of full opioids. This mechanism also creates a “ceiling effect,” where taking more buprenorphine beyond a certain dose doesn’t increase its effects, making it safer regarding overdose risk compared to full agonists. Buprenorphine’s effectiveness and safety have earned it a place on the WHO list of essential medications.
Subutex vs. Suboxone: What’s the Difference?
When exploring treatment, you’ll encounter both Subutex and Suboxone. While both are effective, they have a key difference.
| Feature | Subutex (Buprenorphine only) | Suboxone (Buprenorphine/Naloxone) |
|---|---|---|
| Active Ingredients | Buprenorphine | Buprenorphine and Naloxone |
| Primary Purpose | Treat OUD, pain management | Treat OUD |
| Misuse Deterrent | Minimal | Naloxone (opioid antagonist) |
| Risk of Precipitated Withdrawal (if misused) | Lower (if injected/snorted) | Higher (if injected/snorted) |
| Common Prescribing Scenarios | Initial induction, pregnancy, naloxone sensitivity | Standard OUD treatment |
Suboxone contains naloxone, an opioid antagonist, to deter misuse. If injected, naloxone triggers immediate, unpleasant precipitated withdrawal. Doctors may prescribe Subutex over Suboxone for pregnant patients (due to limited data on naloxone’s effects on a fetus), during the initial treatment phase, or for patients with a naloxone sensitivity. For a more detailed comparison, see our article on Suboxone vs Subutex.
The Risk of Dependence and Precipitated Withdrawal
It’s critical to understand that physical dependence on Subutex, an opioid, can occur. Stopping suddenly triggers Subutex withdrawal. This is a physical adjustment, not addiction. With regular use, your body develops tolerance, meaning it adapts to the drug’s presence.
Misuse, such as taking more than prescribed, is also a concern. A particularly serious risk is precipitated withdrawal. This occurs if you take buprenorphine too soon after using full opioids like heroin or fentanyl. Buprenorphine’s strong bond to opioid receptors displaces other opioids, causing a rapid and intense onset of withdrawal.
Risk factors for precipitated withdrawal include switching from long-acting opioids like methadone or starting with too low a dose of buprenorphine. Proper timing when beginning treatment is crucial to avoid this. We explore these brain chemistry interactions in The Science Behind Opioid Addiction.
The Challenge of Subutex Withdrawal: Symptoms and Comparisons

When you stop using Subutex, your body begins to re-adjust, causing withdrawal. The intensity of your Subutex withdrawal experience varies based on factors like your dosage, duration of use, and individual metabolism. Higher doses and longer use often lead to more intense symptoms.
Common Physical Symptoms of Subutex Withdrawal
The physical side of Subutex withdrawal often feels like a severe flu, appearing 24-48 hours after your last dose. Symptoms can include:
- Muscle aches and cramps
- Nausea, vomiting, and diarrhea, which can lead to dehydration
- Sweating and chills
- Runny nose and watery eyes
- Crushing fatigue combined with insomnia
- Goosebumps (the origin of the term “cold turkey”)
These physical symptoms are your body’s response as it learns to function without the medication. For more information, see our guide on Drug Withdrawal Symptoms.
The Psychological Toll of Subutex Withdrawal
The psychological symptoms of Subutex withdrawal can be even more challenging than the physical ones as your brain readjusts. These can feel overwhelming and include:
- Anxiety, irritability, and agitation
- Depression that can sap your interest in daily activities
- Mood swings and difficulty concentrating (“brain fog”)
- Intense cravings for the drug, which are often the hardest part of recovery
Understanding the connection between medication and mental health is crucial. Learn more in our article on Suboxone and Mental Health.
How Subutex Withdrawal Compares to Other Opioids
There’s good and bad news when comparing Subutex withdrawal to other opioids. The good news is that because buprenorphine is a partial agonist, withdrawal is typically less intense than from full agonists like heroin or fentanyl.
The challenge is that Subutex withdrawal lasts longer. Acute symptoms may not appear for 24-48 hours and can last beyond 10 days, whereas heroin withdrawal often resolves in 5-7 days. This extended timeline, especially for psychological symptoms, makes medical support essential. For more context, visit our page on Opioid Withdrawal.
Navigating the Subutex Withdrawal Timeline
The Subutex withdrawal timeline varies but generally includes an acute phase and Post-Acute Withdrawal Syndrome (PAWS). Your experience depends on your dosage, duration of use, and individual body chemistry.
The First 72 Hours: The Peak of Discomfort
Symptoms typically begin 24-48 hours after the last dose due to buprenorphine’s long half-life. They often peak around day 3, with intense flu-like symptoms: muscle aches, nausea, vomiting, diarrhea, sweating, chills, severe anxiety, and insomnia. This 72-hour window is often the most physically demanding part of withdrawal.
Week 1-2: Physical Symptoms Subside, Psychological Symptoms Linger
After the first few days, physical symptoms gradually subside. By days 7-10, most acute physical discomfort becomes more manageable, though some may linger. However, as physical symptoms fade, psychological ones like depression, mood swings, and sleep disturbances can intensify as your brain chemistry rebalances.
Month 1 and Beyond: Post-Acute Withdrawal Syndrome (PAWS)
For many, Subutex withdrawal continues with Post-Acute Withdrawal Syndrome (PAWS), which is primarily psychological and can last for weeks or months. PAWS is characterized by symptoms that come and go, including:
- Persistent cravings
- Ongoing depression or anxiety
- Irritability and low energy
- Difficulty concentrating (“brain fog”)
- Continued sleep problems
PAWS is challenging because you may look fine but are struggling internally, making the relapse risk high. The temptation to use again for relief is strong during this phase, which is why ongoing support is crucial. Learning effective Tips to Prevent Addiction Relapse is essential for navigating this extended recovery phase.
Detoxing from Subutex: Why Medical Supervision is Crucial

Attempting to detox from Subutex on your own is risky. While not as immediately life-threatening as alcohol withdrawal, it has dangers that are often underestimated. Physical risks include severe dehydration from vomiting and diarrhea, which can become a medical emergency. The intense psychological distress can also escalate into a mental health crisis.
However, the greatest concern is the high risk of relapse. After abstinence, your tolerance is lower, and relapsing on a previous dose could cause a fatal overdose. For this reason, professional support isn’t just helpful—it’s potentially life-saving.
Recommended Detox Methods: Tapering vs. ‘Cold Turkey’
Tapering is the recommended method for stopping Subutex. It involves gradually reducing your dose under medical supervision, which allows your body to adjust and minimizes withdrawal symptoms. A personalized schedule is created and adjusted based on your needs. Slower tapers often lead to better outcomes.
Quitting ‘cold turkey’ is strongly advised against. The abrupt stop shocks your system, causing severe, often unbearable withdrawal symptoms that make relapse highly likely. It is an unnecessarily difficult and risky approach. For more guidance, our article on How to Taper Off Suboxone shares similar principles.
The Role of Medical Detox and Professional Support
Medical detox offers a safe, supportive environment for Subutex withdrawal. It includes 24/7 monitoring by professionals who manage symptoms and complications, ensuring your safety. A key benefit is symptom management medications, such as clonidine for anxiety and anti-nausea drugs. These medical interventions make withdrawal more tolerable and prevent complications.
A detox facility prioritizes your safety and comfort, reducing distress and increasing success rates for long-term recovery. It provides the foundation for a healthier future, often as the first step in a comprehensive plan. Explore how detox fits into the bigger picture in our Beginners Guide to Medication-Assisted Treatment.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today.
Can Home Remedies and Self-Care Help?
Home remedies and self-care can support your detox, but they are not a substitute for medical care. They can make Subutex withdrawal more manageable when combined with professional guidance.
- Hydration: Drink plenty of water, electrolyte drinks, and clear broths to prevent dehydration, which is a serious risk.
- Nutrition: Eat small, bland, nutritious meals to stabilize your energy. Focus on easily digestible foods. The Importance of Nutrition in Addiction Recovery is a cornerstone of healing.
- Light exercise and relaxation: Gentle walks can improve mood and sleep. Techniques like deep breathing and meditation can calm anxiety.
Life After Detox: Preventing Relapse and Building a New Future

Completing Subutex withdrawal is a major accomplishment, but it’s the beginning of recovery, not the end. Detox clears your system, but the real work is addressing the root causes of opioid use and learning to live without them. After detox, you begin building a new life by developing tools for long-term sobriety.
The Importance of Continued Treatment
After the physical challenges of Subutex withdrawal, your brain and emotions need to heal. Ongoing treatment is essential for better long-term outcomes.
- Therapy and counseling are the backbone of recovery. Individual therapy helps you work through personal issues, while group therapy provides a sense of community and shared understanding.
- Cognitive-Behavioral Therapy (CBT) is highly effective. It teaches you to identify and change negative thought patterns and behaviors, helping you manage triggers and stress.
- It’s also crucial to address co-occurring disorders like depression or anxiety through integrated treatment, as they are often linked to addiction. Our Addiction Counseling Services provide this comprehensive approach.
Support Systems for Lasting Sobriety
Recovery requires a strong support system. Connecting with people who support your sobriety is a powerful tool for relapse prevention.
- Peer support groups like Narcotics Anonymous (NA) offer understanding from others with similar experiences. Sharing your story in a non-judgmental setting provides hope and a sense of community.
- Family therapy helps repair relationships damaged by addiction. It improves communication and teaches family members how to provide healthy support, allowing the entire family to heal. Understanding How to Support Someone Recovery is vital for your loved ones.
- Building a sober network is vital. Surround yourself with supportive friends and family, and create distance from people and situations that trigger substance use. Your environment heavily influences your choices.
The journey after Subutex withdrawal requires commitment and support. With the right treatment plan, lasting recovery is possible. Learn more with our Tips to Prevent Addiction Relapse.
Frequently Asked Questions about Subutex Withdrawal
We understand you have questions about Subutex withdrawal. Here are answers to some common concerns.
How long does Subutex withdrawal last?
The timeline for Subutex withdrawal varies. Acute physical symptoms usually start 24-48 hours after the last dose, peak around day 3, and subside over 7-10 days. However, psychological symptoms and Post-Acute Withdrawal Syndrome (PAWS), including cravings, depression, and anxiety, can last for weeks or months. The duration depends on factors like dosage and length of use, highlighting the need for ongoing support.
Can Subutex withdrawal be dangerous?
While Subutex withdrawal is not typically life-threatening like alcohol withdrawal, it can have dangerous complications. Severe dehydration from vomiting and diarrhea is a primary concern. The biggest danger, however, is the high risk of relapse. After withdrawal, your opioid tolerance is lower, which dramatically increases the risk of an accidental overdose if you use again. Medical supervision is crucial for safety.
Is it better to taper off Subutex or stop ‘cold turkey’?
Tapering under medical supervision is strongly recommended over stopping “cold turkey.” Tapering involves a gradual dose reduction, allowing your body to adjust slowly. This minimizes Subutex withdrawal symptoms and increases your chances of success. A personalized tapering schedule is created and adjusted based on your needs.
Stopping “cold turkey” causes a sudden shock to your system, triggering severe symptoms that are often overwhelming and lead to relapse. It is an unnecessarily difficult and risky approach.
Your Path to Recovery Starts Here
Understanding Subutex withdrawal is a vital first step. While detox is a critical foundation, true recovery involves building a new life by addressing the root causes of your substance use. Recovery is a journey that takes time, patience, and professional guidance. You don’t have to do it alone.
At National Addiction Specialists, we offer confidential, telemedicine-based Medication-Assisted Treatment (MAT) that meets you where you are. From the privacy of your home, you can connect with our expert providers who create personalized recovery plans combining medication management with counseling and support.
We proudly serve individuals in Tennessee and Virginia, and we accept both Medicaid and Medicare. Your insurance shouldn’t be a barrier to getting the help you deserve.
Taking control of your life starts with a single decision. If you’re ready to begin your journey away from Subutex withdrawal and toward lasting recovery, we’re here to help.
Schedule an appointment today to learn how we can support your path to a healthier, more fulfilling future.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








