Subutex 8mg: Understanding Your Prescription
Understanding Your Subutex Prescription: What You Need to Know
Subutex dosage information is essential for anyone starting treatment for opioid dependence. Subutex contains buprenorphine, a partial opioid agonist that reduces cravings and withdrawal symptoms without the “high” of full agonists.
Key Dosage Facts:
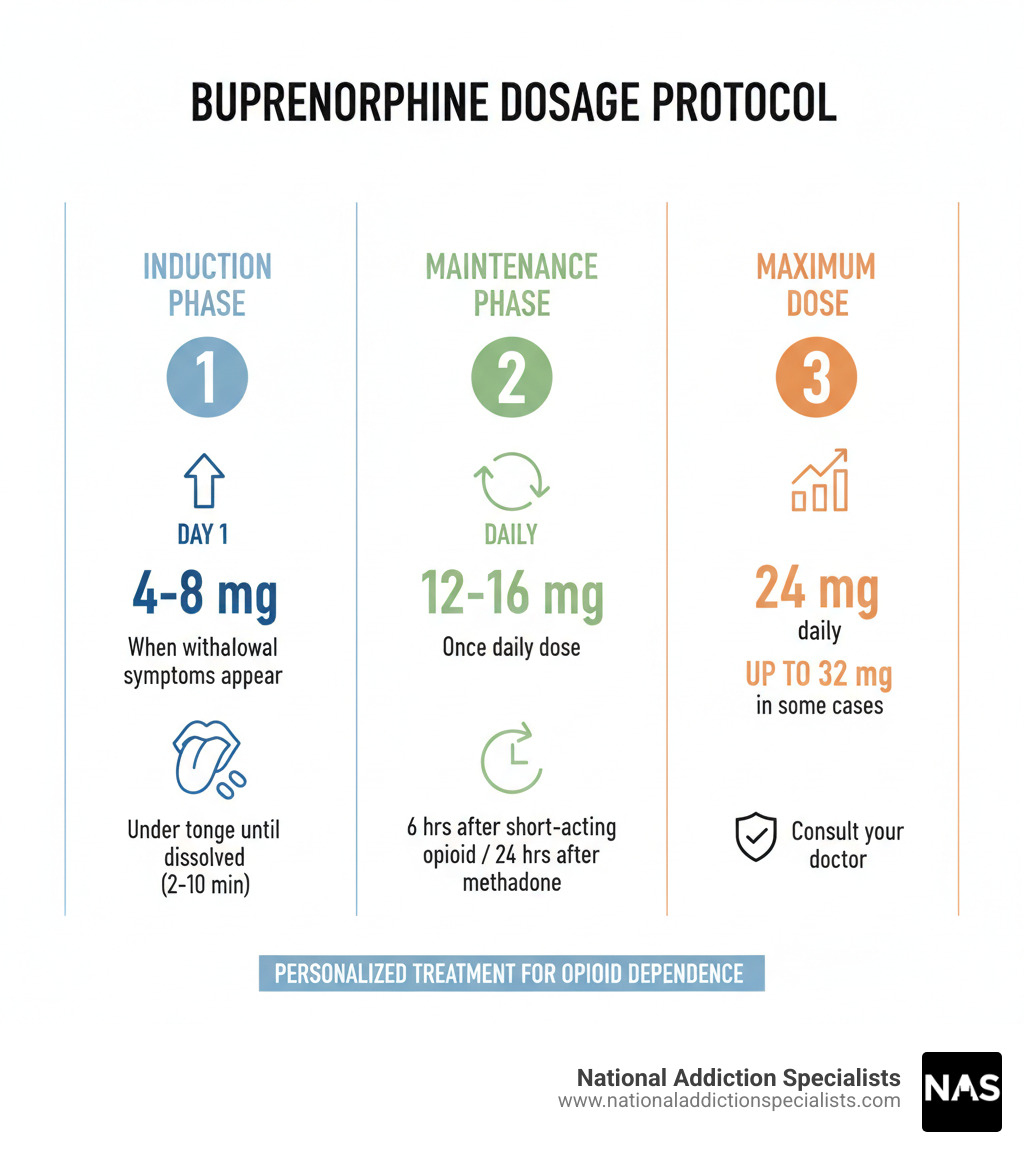
- Starting Dose (Day 1): 4-8 mg, taken when withdrawal symptoms appear
- Typical Maintenance Dose: 12-16 mg once daily
- Maximum Recommended Dose: 24 mg per day (up to 32 mg in some cases)
- Administration: Place tablet under your tongue until fully dissolved (2-10 minutes)
- Timing: Wait at least 6 hours after your last short-acting opioid use, or 24 hours after methadone
Your dosage is not one-size-fits-all; it’s personalized based on your opioid use history, health, and response to treatment. Your doctor will start you on a low dose and adjust it as needed.
Subutex is often used for the initial induction phase before many patients transition to a combination medication for long-term maintenance. The goal is to find the lowest effective dose that keeps you comfortable and supports your recovery.
As Chad Elkin, MD, founder and Chief Medical Officer of National Addiction Specialists, I’ve guided hundreds of patients through safe Subutex treatment. My focus is ensuring every patient receives personalized, evidence-based care.
Glossary for Subutex dosage information:
Comprehensive Subutex Dosage Information
Getting your Subutex dosage information right is about finding a personalized path. At National Addiction Specialists, we guide patients through each phase of treatment, from the first dose to a stable maintenance level. We work with you to ensure your safety and success.
The Induction Phase: Your Starting Dose
The induction phase begins your recovery journey with Subutex. The main concern is “precipitated withdrawal,” a sudden onset of intense symptoms if buprenorphine is taken too soon after other opioids. This is preventable with proper timing.
Timing is everything.
- Short-acting opioids (heroin, oxycodone): Wait at least 6 hours after your last use before your first dose. Your doctor may advise waiting until you feel the first signs of withdrawal.
- Long-acting opioids (methadone): Wait at least 24 hours after your last dose. Your doctor will likely reduce your methadone dose before the switch.
To ensure you’re ready, your doctor may use the Clinical Opiate Withdrawal Scale (COWS). A score of 12 or higher typically signals it’s safe to begin.
What is the recommended starting dose of Subutex for opioid dependence? On Day 1, you’ll typically receive 4-8 mg. An additional 4 mg dose may be given later that day, depending on your symptoms.
How is the dosage of Subutex adjusted during treatment? Over the next few days, your doctor will adjust your dose in small steps (2-4 mg at a time) in a process called titration. This helps find the lowest effective dose to control your symptoms and cravings. This personalized approach is exactly how Medication Assisted Treatment works.
Adjusting for Maintenance: Finding Your Stable Dose
Once initial withdrawal is controlled, the focus shifts to a long-term maintenance dose for lasting stability. The goal is to suppress cravings and block the effects of other opioids, providing a foundation for recovery.
What is the maximum recommended daily dose of Subutex? The target maintenance dose is typically 16 mg once daily. Some patients do well on 8-12 mg, while others may need up to 24 mg per day. Doses up to 32 mg may be prescribed, but research shows little benefit above 24 mg due to the ceiling effect. As a partial opioid agonist, buprenorphine’s effects plateau at higher doses, which is a key safety feature that reduces overdose risk compared to full agonists.
| Phase | Goal | Typical Daily Dosage | Duration |
|---|---|---|---|
| Induction | Safely suppress acute withdrawal and cravings | 4-8 mg on Day 1, increasing to 16 mg over 2-3 days | 1-3 days, up to a week |
| Maintenance | Prevent withdrawal/cravings, block opioid effects | 8-24 mg (target 16 mg); up to 32 mg in some cases | Ongoing, as determined by you and your doctor |
How to Take Subutex Correctly
How you take Subutex is as important as the dose. It must be taken sublingually (under the tongue) to be effective.
How should Subutex be administered, and does this affect dosage? Place the tablet under your tongue and let it dissolve completely, which takes 2-10 minutes. Do not chew, swallow, cut, or break it. Buprenorphine is not effective if swallowed because the digestive system breaks it down. Dissolving it under the tongue allows it to be absorbed directly into the bloodstream.
While the tablet dissolves, avoid talking or drinking. After it has dissolved, you can rinse your mouth with water. Some doctors recommend waiting an hour before brushing your teeth to protect your oral health.
Can Subutex be split or broken? No. Altering the tablet can change how the medication is absorbed, leading to an incorrect dose.
How should a missed dose of Subutex be handled? Take it as soon as you remember. If it’s almost time for your next dose, skip the missed one. Do not double up. Consistent dosing is key to stability, so talk to your provider if you frequently miss doses.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Safety, Side Effects, and Special Dosage Considerations
Safe Subutex use requires understanding its risks, side effects, and necessary dosage adjustments for your health profile. This knowledge empowers you to stay safe during recovery. At National Addiction Specialists, we ensure you have all the information you need.
Potential Side Effects Related to Dosage
When starting or adjusting Subutex, you may experience side effects, which are often mild and temporary.
What are the potential side effects related to Subutex dosage? Common side effects include:
- Headache
- Nausea and vomiting
- Constipation
- Drowsiness or sedation
- Increased sweating
- Insomnia
- Body aches and flu-like symptoms
These usually improve within a few days or weeks. However, some serious side effects require immediate medical attention:
- Respiratory Depression: This is the most serious risk, involving slow or shallow breathing. While buprenorphine’s “ceiling effect” makes it less likely than with full opioids, the risk increases when combined with substances like benzodiazepines or alcohol. Watch for confusion, extreme sleepiness, and slowed breathing.
- Severe Liver Problems: Though rare, watch for signs like jaundice (yellowing skin/eyes), dark urine, light-colored stools, or persistent fatigue.
- Severe Allergic Reactions: Seek emergency help for difficulty breathing or swelling of the face, lips, or throat.
- Dental Problems: Cases of tooth decay and loss have been reported. Maintain good oral hygiene and see your dentist regularly.
For more details, see our resource on Subutex Side Effects. Contact your doctor if you experience any concerning symptoms.
Risks of Overdose and Interactions
While safer than full agonists, Subutex is still an opioid, and overdose is possible, especially when misused or combined with other substances.
What are the risks associated with taking too much Subutex (overdose)? An overdose is a medical emergency. Signs include:
- Pinpoint pupils
- Slowed or shallow breathing
- Extreme drowsiness or unconsciousness
- Confusion, dizziness, blurred vision
- Pale or blue-tinged skin, lips, or fingernails
Call 911 immediately if you suspect an overdose. We recommend that patients and their families have naloxone (Narcan) available and know how to use it.
The Critical Danger of Drug Interactions
The greatest risk of overdose and death comes from mixing Subutex with other central nervous system (CNS) depressants.
- Benzodiazepines and Alcohol: Combining Subutex with benzodiazepines (Xanax, Ativan) or alcohol is extremely dangerous. This combination can lead to profound sedation, respiratory depression, coma, and death. Avoid alcohol completely during treatment.
- Other CNS Depressants: Sedatives, tranquilizers, certain antihistamines, and some antidepressants can increase the risk of respiratory depression.
- Serotonergic Drugs: Combining Subutex with certain antidepressants (SSRIs) or migraine medications (triptans) can lead to a rare but serious condition called Serotonin Syndrome.

Always discuss all medications and substances with your doctor. Scientific research highlights these risks, which you can explore here: Scientific research on buprenorphine overdose.
Special Subutex Dosage Information and Adjustments
Your Subutex dosage information must be customized to your health profile. Certain conditions require special attention:
- Switching from Methadone: Requires a cautious approach. Your doctor will likely taper your methadone and require at least a 24-hour waiting period after your last dose to prevent precipitated withdrawal.
- Age over 65: Your doctor may start with a lower dose and increase it more slowly due to increased sensitivity to medications.
- Liver Impairment: If you have severe liver problems, your doctor will likely reduce your dose and monitor you closely, as buprenorphine can accumulate in your system.
- Kidney Impairment: Dose adjustments are generally not required for kidney problems.
- Pregnancy: Subutex (buprenorphine-only) is often preferred for pregnant patients to reduce fetal exposure to naloxone. Your dose will be carefully managed to balance the health of both mother and baby.
- Other Conditions: Tell your doctor if you have a history of seizures or respiratory conditions like asthma or COPD, as buprenorphine requires careful monitoring in these cases.
Make an Appointment to Treat Addiction
If you’re ready to take the next step, we’re here to help. Make an appointment today.
Subutex in Medication-Assisted Treatment
Subutex is a unique Medication-Assisted Treatment (MAT) because it’s a buprenorphine-only product (no naloxone). This makes it an ideal starting point for many patients beginning their recovery. Understanding its role can help you feel more confident in your treatment plan.
Why Subutex is Used for Induction
Subutex is ideal for the induction phase because it contains only buprenorphine. This “monotherapy” provides a gentler transition and avoids the risk of precipitated withdrawal from naloxone, making it safer to start treatment while we ease your withdrawal symptoms and cravings.
During induction with Subutex, the focus is on getting you stable as quickly and safely as possible. The dose typically starts at 4-8 mg and is adjusted until you are comfortable, usually around 12-16 mg within a few days. You can Learn more about Subutex and its role in your treatment on our site.
Transitioning to Maintenance Medication
After a successful induction with Subutex (usually 1-2 days), your doctor will likely discuss transitioning to a different medication for long-term maintenance.
For most patients, this means switching to a buprenorphine-naloxone combination product like Suboxone. This switch is for safety during unsupervised, at-home use. The naloxone in combination products is a misuse deterrent; it is not absorbed when taken as directed but will trigger immediate withdrawal if the medication is injected or snorted.
This makes combination products much safer for take-home use. However, some patients may continue Subutex for maintenance due to a naloxone allergy or other clinical reasons. Other maintenance options include long-acting injections like Sublocade or Brixadi, which offer the convenience of weekly or monthly dosing. Your doctor will work with you to find the best long-term plan for your recovery.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Discontinuing Subutex: The Tapering Process
Discontinuing Subutex is a major step that requires medical supervision. Your doctor will guide you through a gradual dosage reduction, known as tapering, to minimize discomfort and prevent relapse.
Risks of Abrupt Discontinuation
Stopping Subutex suddenly (“cold turkey”) can trigger a painful opioid withdrawal syndrome because your body has become physically dependent on it.
What are the risks of abrupt discontinuation of Subutex, and how does this relate to dosage tapering?
Abruptly stopping can cause uncomfortable and protracted withdrawal symptoms, including:
- Physical symptoms: Nausea, vomiting, diarrhea, muscle aches, cramps, sweating, and chills.
- Psychological symptoms: Intense cravings, anxiety, depression, irritability, and insomnia.
Severe withdrawal symptoms significantly increase the risk of relapse. Returning to opioid use after stopping Subutex is especially dangerous because your tolerance is lower, raising the risk of a fatal overdose. A controlled, gradual taper is crucial for your safety. For more information, see our page on Understanding Subutex Withdrawal.
How to Taper Off Subutex Safely
The key to safely discontinuing Subutex is a gradual dosage tapering plan supervised by your doctor. There is no one-size-fits-all schedule; it is personalized based on your dose, treatment duration, health, and response to reductions.
- Medical Supervision: Your doctor will create and manage your tapering schedule.
- Gradual Dose Reduction: The dose is typically reduced in small increments (e.g., 2-4 mg) every one to two weeks or even more slowly to minimize withdrawal symptoms.
- Monitoring and Adjustment: Your doctor will monitor you for withdrawal or cravings and can slow or pause the taper if you experience significant discomfort.
- Support Systems: Continued counseling and psychosocial support are vital for managing any emotional challenges that arise during the process.
The decision to taper should be a shared one between you and your provider. For more detailed guidance, visit our page on How to Taper Off Subutex.
Conclusion: The Importance of Professional Guidance
We’ve covered key Subutex dosage information, from starting treatment to tapering off. This complex medical information is meant to empower you for discussions with your doctor.
This article is for informational purposes only and is not a substitute for professional medical advice.
Your Subutex dosage must be personalized and managed by a certified addiction medicine physician. It depends on your opioid use history, health, and other factors. Never attempt to determine your own dose or adjust it without medical supervision. A qualified doctor is the only person who can safely create and monitor your treatment plan.
At National Addiction Specialists, we remove barriers to recovery. We offer expert, confidential telemedicine care from your home in Tennessee and Virginia. Our team of compassionate professionals provides personalized, evidence-based treatment that fits your life. We accept Medicaid and Medicare to make treatment accessible.
Recovery is possible, and you don’t have to do it alone. If you or someone you love is struggling, we encourage you to reach out. Your path to a healthier life starts with a single conversation.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.