Suboxone Withdrawal Symptoms and How to Handle the Heat
What Are Withdrawal Symptoms from Suboxone? Here’s What to Expect
What are withdrawal symptoms from Suboxone is one of the most important questions anyone stopping this medication needs answered — and the honest answer is: they’re real, they’re manageable, and knowing what’s coming makes all the difference.
Here’s a quick overview of the most common symptoms:
| Type | Common Symptoms |
|---|---|
| Physical | Muscle aches, nausea, vomiting, diarrhea, sweating, chills, headaches, insomnia |
| Psychological | Anxiety, depression, irritability, mood swings, drug cravings, restlessness |
| Timeline | Symptoms begin 12-48 hours after last dose; physical symptoms peak at 72 hours and mostly resolve within a month; psychological symptoms can linger for weeks or months |
Suboxone is a medication that has helped countless people break free from opioid addiction. But when it’s time to stop taking it, the body doesn’t simply return to normal overnight. Because Suboxone contains buprenorphine — a partial opioid agonist — your brain has adapted to its presence. Removing it triggers a withdrawal process that is both physical and emotional.
The good news? Suboxone withdrawal is generally less intense than withdrawal from full opioids like heroin or oxycodone. But it tends to last longer, and the emotional side can catch people off guard.
I’m Chad Elkin, MD — board-certified in Addiction Medicine and founder of National Addiction Specialists — and understanding what are withdrawal symptoms from Suboxone is something I work with patients on every day in my clinical practice. In this guide, I’ll walk you through exactly what to expect, when to expect it, and how to get through it as safely as possible.
Simple what are withdrawal symptoms from suboxone glossary:
Understanding Suboxone and Its Role in Opioid Treatment
To understand why withdrawal happens, we first need to look at what Suboxone actually is. It is a combination of two active ingredients: buprenorphine and naloxone.
Buprenorphine is a “partial opioid agonist.” Think of your brain’s opioid receptors like a lock. A full agonist (like heroin or oxycodone) turns the key all the way, creating a massive “high” and slowing down your breathing. Buprenorphine only turns the key halfway. It provides enough stimulation to stop cravings and prevent withdrawal symptoms, but it has a “ceiling effect.” This means that after a certain dose, taking more doesn’t increase the effect, making it much safer than traditional opioids.
The second ingredient, naloxone, is an antagonist. It’s added to prevent misuse. If someone tries to inject the film, the naloxone kicks in and causes immediate, “precipitated” withdrawal. When taken correctly under the tongue (sublingually), the naloxone isn’t absorbed well, allowing the buprenorphine to do its job.
According to Suboxone: Uses, Dosage and Side Effects, the medication is highly effective for maintenance because it stays in your system for a long time. However, this long “half-life” (roughly 24 to 42 hours) is exactly why withdrawal symptoms take longer to show up and longer to leave than other drugs.
What are withdrawal symptoms from Suboxone?
When we talk about what are withdrawal symptoms from Suboxone, we are describing the body’s “rebound” effect. After being on the medication for a while, your brain stops producing its own feel-good chemicals in normal amounts because it relies on the buprenorphine. When you stop, your nervous system goes into overdrive—a state known as autonomic hyperactivity.
The severity of these symptoms isn’t the same for everyone. Several factors influence how “hot” the withdrawal heat gets:
- Duration of use: How many months or years you have been on the medication.
- Dosage: Higher daily doses usually lead to more significant physical dependence.
- Metabolism: Everyone processes medicine differently based on genetics and liver health.
- Concurrent health conditions: Other mental health or physical issues can amplify the discomfort.
Research on opioid receptor imaging shows that buprenorphine binds very tightly to the receptors in the brain. Even a tiny dose—as low as 0.25mg—can still be occupying a significant number of receptors. This is why many people feel “stuck” at the end of their taper.
Common Physical Withdrawal Symptoms from Suboxone
Physical symptoms are usually what people fear the most. They typically begin within 24 to 48 hours after the last dose and are often most intense during the first 72 hours.

The most common physical withdrawal symptoms include:
- Muscle Aches and “Heebie Jeebies”: Patients often describe an excruciating, restless feeling in their legs or back.
- Digestive Distress: Nausea, vomiting, and diarrhea are common as the gut (which is full of opioid receptors) tries to recalibrate.
- Sweating and Chills: You might feel like you’re burning up one minute and freezing the next.
- Insomnia: Sleep can be incredibly elusive during the first week.
- Headaches: Tension headaches are a frequent complaint reported in Patient Information for SUBOXONE®.
While these symptoms feel like a severe flu, they are rarely life-threatening on their own. However, they can be exhausting and are the primary reason people might consider returning to opioid use just to find relief.
Psychological and Emotional Withdrawal Symptoms from Suboxone
While the physical stuff is rough, many of our patients tell us the emotional “heat” is actually harder to handle. Because Suboxone has been stabilizing your mood for so long, stopping it can feel like a sudden emotional crash.
Common psychological opioid withdrawal symptoms include:
- Anxiety and Restlessness: A constant feeling of being “on edge.”
- Depression: A deep sense of sadness or lack of motivation.
- Irritability: Small things that didn’t bother you before might suddenly feel infuriating.
- Drug Cravings: The brain starts demanding the substance it’s missing.
- Cognitive Fog: Difficulty concentrating or remembering simple tasks.
Research on mood during detoxification highlights that these emotional symptoms often peak a bit later than the physical ones—usually around the second week—and can persist much longer.
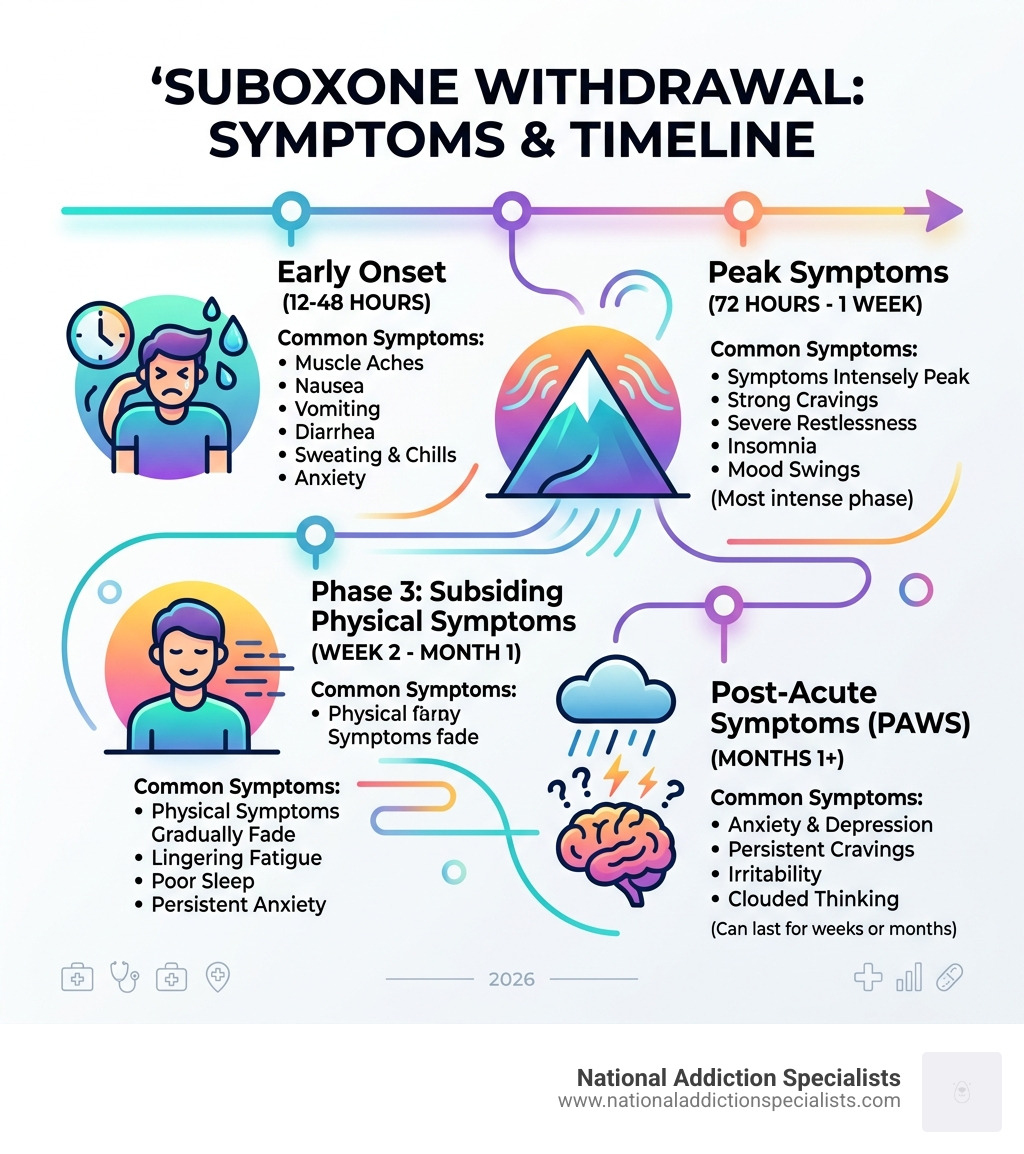
The Suboxone Withdrawal Timeline: Acute and Post-Acute Phases
Knowing the timeline helps you “brace for the waves.” Instead of feeling like the symptoms will last forever, you can check them off a calendar.
| Phase | Timeline | What to Expect |
|---|---|---|
| Onset | 12–48 Hours | Mild anxiety, yawning, watery eyes, and the start of cravings. |
| Peak (Acute) | 72 Hours – 1 Week | Physical symptoms are at their worst: muscle aches, GI issues, and sweating. |
| Subsiding | Weeks 2 – 4 | Physical symptoms fade, but depression and fatigue may set in. |
| Post-Acute (PAWS) | 1 Month – 6+ Months | Lingering psychological symptoms like anxiety and sleep disturbances. |
The From Start to Finish: Understanding the Suboxone Withdrawal Timeline guide explains that most physical symptoms disappear within a month. However, the first 10 days are generally the “acute” phase where you’ll need the most support.
Post-Acute Withdrawal Syndrome (PAWS)
Some people experience what we call PAWS. This is the “long tail” of withdrawal. Even after the nausea and aches are gone, your brain is still rewiring itself. This can lead to persistent opioid withdrawal effects like:
- Intermittent sleep problems.
- Low energy or “anhedonia” (not finding joy in things you used to love).
- Occasional spikes in anxiety.
This happens because the brain’s reward system has been “down-regulated.” Research on reward deficiency syndrome suggests that it takes time for natural dopamine production to return to normal levels. This is why long-term counseling and support are so vital—even after the “detox” is technically over.
Managing Symptoms Safely: Tapering vs. Cold Turkey
We are often asked: “Can I just quit cold turkey?” Our professional advice is almost always no.
Quitting Suboxone cold turkey is like slamming on the brakes of a car going 80 mph. It’s a shock to the system that often leads to severe symptoms and a very high risk of relapse. Instead, we recommend a Suboxone withdrawal treatment plan based on a gradual taper.
A slow taper involves reducing your dose by a small amount (often 5-10%) every few weeks. This gives your brain time to adjust to slightly lower levels of buprenorphine without sending you into a tailspin.
Medical supervision is key for several reasons:
- Safety: A doctor can monitor your vitals and ensure you’re staying hydrated.
- Comfort: We can prescribe non-addictive “comfort meds” (like clonidine for blood pressure/anxiety or certain medications for sleep and nausea) to take the edge off.
- Relapse Prevention: Having a professional to talk to when cravings hit makes a world of difference.
At National Addiction Specialists, we provide this care through telemedicine, meaning you can manage your taper from the comfort of your home in Tennessee or Virginia. We believe that recovery shouldn’t be a “white-knuckle” experience.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
Frequently Asked Questions about Suboxone Withdrawal
How long do physical symptoms last?
While the peak intensity is usually in the first 72 hours, most physical symptoms will gradually subside over about 10 to 14 days. By the one-month milestone, the majority of physical discomfort is usually gone, though some fatigue may remain.
Is it safe to quit Suboxone cold turkey?
It is generally not recommended. While not typically fatal, the intensity of cold-turkey withdrawal often leads to “failed” detoxes and relapse. Tapering under medical monitoring is the gold standard for safety and long-term success.
Does Suboxone help with withdrawal symptoms from other opioids?
Yes, that is its primary job! Does Suboxone Help with Withdrawal Symptoms? explains that buprenorphine satisfies the brain’s need for opioids without the dangerous “high.” It provides cross-tolerance, meaning it can stabilize someone coming off heroin, fentanyl, or oxycodone, allowing them to focus on therapy instead of just “surviving” the day.
Conclusion
Understanding what are withdrawal symptoms from Suboxone is the first step toward a successful transition. Yes, there is some “heat” involved, but with a personalized tapering plan and professional support, it is a fire you can walk through.
At National Addiction Specialists, we’re here to help you every step of the way. Our telemedicine-based care in Tennessee and Virginia is designed to be convenient, confidential, and compassionate. Whether you are looking to start MAT or are ready to begin your journey toward being medication-free, our expert providers are ready to create a plan that works for you.
Don’t let the fear of withdrawal keep you from the life you deserve. Reach out to us today to learn more about our Suboxone withdrawal guide and how we can support your long-term sobriety.
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.