Suboxone Withdrawal Duration: What to Expect and When It Ends
How Long Does Suboxone Withdrawal Last? Here’s What You Need to Know
How long does suboxone withdrawal last is one of the most important questions anyone considering stopping this medication will ask — and the honest answer is: it depends, but most people can expect symptoms to span roughly one month.
Here’s a quick breakdown:
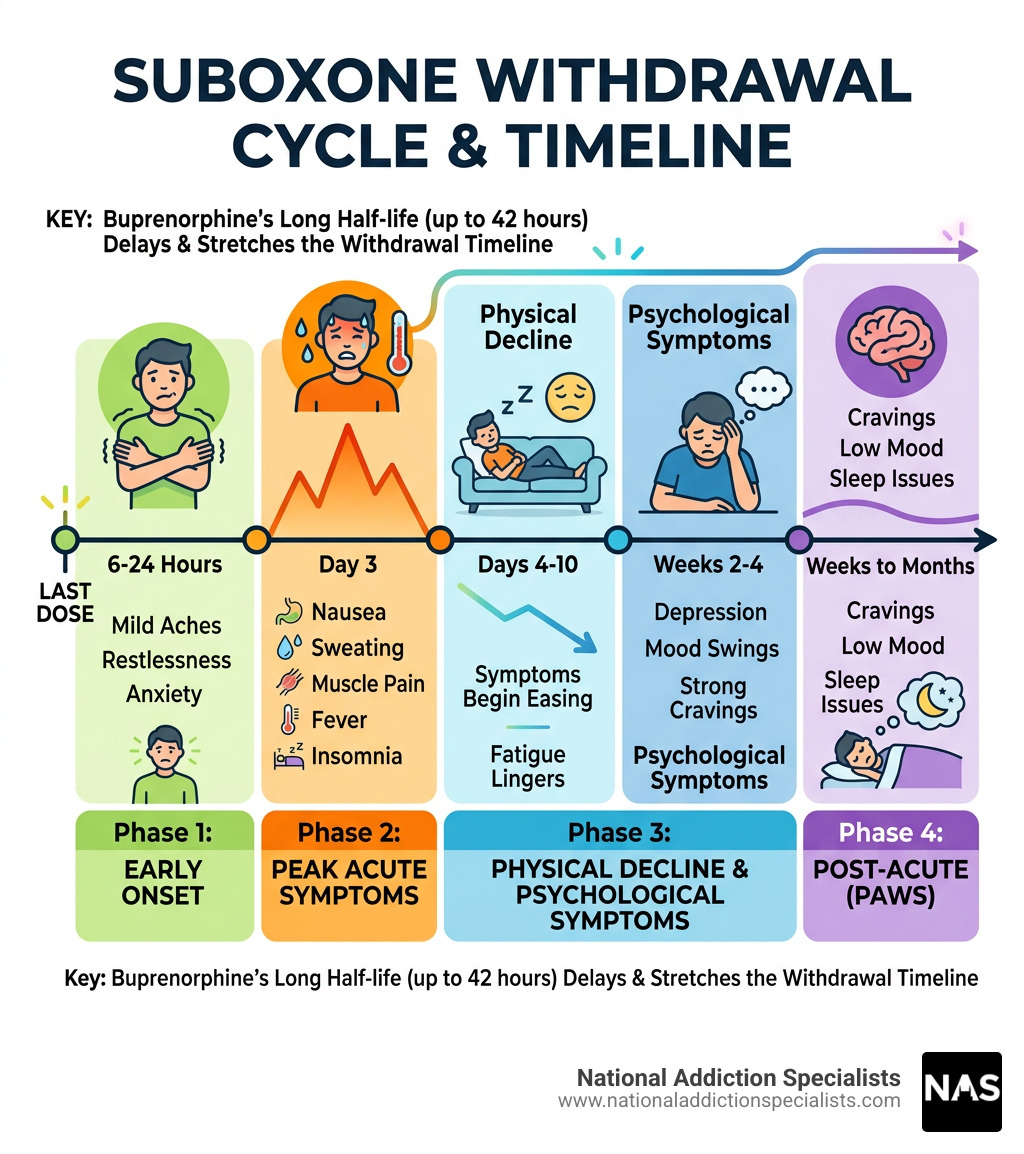
| Phase | Timeline | What to Expect |
|---|---|---|
| Early onset | 6–24 hours after last dose | Mild aches, restlessness, anxiety |
| Peak acute symptoms | 72 hours (days 1–3) | Nausea, sweating, muscle pain, fever, insomnia |
| Physical decline | Days 4–10 | Symptoms begin easing, fatigue lingers |
| Psychological symptoms | Weeks 2–4 | Depression, mood swings, strong cravings |
| Post-acute (PAWS) | Weeks to months | Cravings, low mood, sleep issues |
The physical symptoms are usually the worst in the first three days. Most physical discomfort fades within one to two weeks. But the emotional and psychological effects — depression, cravings, and sleep problems — can linger for weeks or even months after that.
This is partly because Suboxone contains buprenorphine, a long-acting partial opioid agonist with a half-life of up to 42 hours. That long half-life delays the onset of withdrawal but also stretches out the timeline compared to shorter-acting opioids.
Knowing what to expect — and when — makes the process far less frightening.
I’m Dr. Chad Elkin, board-certified Addiction Medicine physician and founder of National Addiction Specialists, and I’ve worked with hundreds of patients navigating the question of how long does suboxone withdrawal last as they transition safely off Suboxone. In the sections below, I’ll walk you through the full timeline, the factors that shape your personal experience, and the safest ways to manage every stage.
How long does suboxone withdrawal last terms at a glance:
Understanding the Suboxone Withdrawal Timeline
To understand the Suboxone Withdrawal experience, we first have to look at how the medication works. Suboxone is a combination of two active ingredients: buprenorphine and naloxone. Buprenorphine is a “partial opioid agonist,” which means it sticks to the brain’s opioid receptors to stop cravings and withdrawal, but it doesn’t produce the intense “high” of full agonists like heroin or oxycodone. Naloxone is added as a safety mechanism; it is an antagonist that stays inactive unless someone tries to inject the medication, at which point it triggers immediate withdrawal.
Because buprenorphine has an exceptionally long half-life (ranging from 24 to 60 hours depending on the individual), it stays in your system much longer than most other opioids. This is a double-edged sword. On one hand, it means you only need to take it once a day. On the other hand, it means that when you stop taking it, the From Start to Finish: Understanding the Suboxone Withdrawal Timeline is more drawn out.
While a heroin withdrawal might be “over” in a week, Suboxone withdrawal is often described as a marathon rather than a sprint. We generally categorize this journey into two distinct stages: the acute phase and the post-acute phase.
How long does suboxone withdrawal last in the acute phase?
The acute phase is where the “heavy lifting” happens. This is the period when your body is physically reacting to the absence of the medication. Clinical research on buprenorphine withdrawal suggests that symptoms typically begin within 24 to 48 hours of the last dose.
During the first 72 hours, symptoms usually reach their peak. You might feel like you have a particularly nasty case of the flu. Common symptoms during this peak include:
- Intense muscle aches and joint pain
- Excessive sweating and “gooseflesh”
- Nausea, vomiting, or digestive upset
- Fever and chills
- Severe insomnia and restlessness
By the end of the first week (days 4–7), the most intense physical symptoms usually begin to subside, though you may still feel very fatigued and “foggy.” Most physical symptoms are largely gone by day 10, but that doesn’t mean the journey is over.
how long does suboxone withdrawal last during the PAWS stage?
Once the physical “flu” passes, many people enter what is known as Post-Acute Withdrawal Syndrome, or PAWS. This is where the psychological battle begins. Because opioids change how your brain processes dopamine and handles stress, it takes time for your internal chemistry to return to its natural baseline.
During PAWS, you might experience:
- Depression and Anxiety: Feeling “flat” or easily overwhelmed.
- Sleep Disturbances: Difficulty falling or staying asleep, even after the physical restlessness is gone.
- Cravings: Sudden, intense urges to use opioids again.
- Cognitive Issues: Difficulty concentrating or memory “blips.”
How long does PAWS last? It varies significantly. For some, it might be a few weeks of “the blues.” For others, these symptoms can linger for several months. Understanding Opioids and PAWS is vital because this is the stage where the risk of relapse is highest. Without the physical “barrier” of Suboxone, your brain may try to convince you that using again is the only way to feel “normal.”
Factors That Influence how long does suboxone withdrawal last
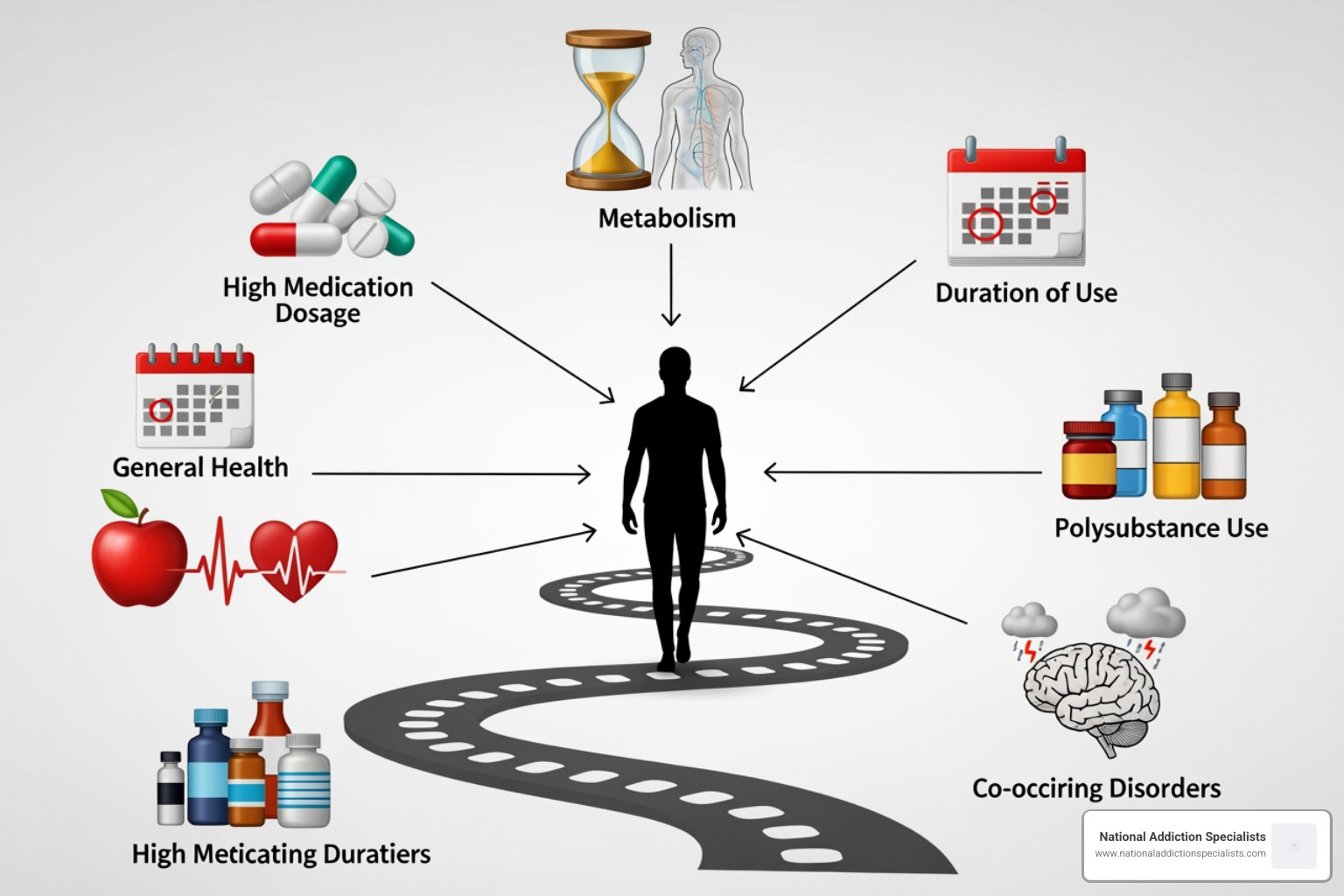
Not everyone experiences withdrawal the same way. We often see patients who breeze through the process, while others find it more challenging. Several key factors influence the severity and duration of your symptoms:
- Dosage Levels: If you have been taking a high dose of Suboxone (such as 16mg or 24mg daily), your brain has more receptors occupied. Coming down from a higher peak generally takes longer and feels more intense than starting from a lower dose.
- Duration of Use: The longer you have been on the medication, the more your brain has adapted to its presence. This is why the question of How Long Should I Stay on Suboxone? is so personal; staying on it longer provides more stability, but it also means a longer adjustment period later.
- Metabolism and General Health: Your body’s ability to clear the medication depends on your liver function, age, and activity level. People with faster metabolisms may move through the acute phase more quickly.
- Polysubstance Use: If you are also using alcohol, benzodiazepines, or other substances, the withdrawal process becomes significantly more complex and potentially more dangerous.
- Presence of Co-occurring Disorders: If you struggled with depression or anxiety before starting Suboxone, those symptoms may flare up during the withdrawal process, making the PAWS stage feel more permanent.
Managing Symptoms and Tapering Safely
The most important thing we tell our patients is: Do not quit cold turkey. While Suboxone withdrawal is rarely life-threatening on its own, the discomfort of stopping abruptly is the leading cause of relapse. The safest, most effective way to stop is through a medically supervised taper.
Learning How to Taper off Suboxone involves gradually reducing your dose over weeks or even months. This gives your brain time to slowly adjust to lower levels of buprenorphine, significantly minimizing the “crash” associated with quitting. At National Addiction Specialists, we provide Suboxone Withdrawal Treatment that is tailored to your specific needs, ensuring you never have to “white-knuckle” through the process alone.
Following FDA-approved buprenorphine information and clinical guidelines, a slow taper allows you to maintain your daily responsibilities — like work and family — while your body heals.
Medications and lifestyle strategies to ease withdrawal
Even with a perfect taper, you might still feel some discomfort. Fortunately, there are several tools we can use to help:
- Prescription Medications: Drugs like Clonidine can help manage anxiety, sweating, and high blood pressure. Newer, non-opioid medications like Lucemyra are specifically FDA-approved to reduce the severity of Opioid Withdrawal Symptoms by blocking the release of excess norepinephrine (the “stress” chemical) in the brain.
- Hydration and Nutrition: Withdrawal often causes dehydration due to sweating and digestive issues. Drinking plenty of water and eating small, bland, nutrient-dense meals can keep your energy levels up.
- Gentle Exercise: While you won’t feel like running a marathon, a short walk or some light yoga can help release natural endorphins, which are the body’s built-in pain relievers.
- Sleep Hygiene: Establishing a calm nighttime routine can help combat the insomnia that often plagues the first few weeks.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
Frequently Asked Questions About Suboxone Withdrawal
Is suboxone withdrawal worse than other opioids?
This is a common concern. The answer is that it is different. If you compare it to heroin or fentanyl, Suboxone withdrawal is generally considered “moderate” in intensity but much longer in duration. Heroid withdrawal hits like a freight train but is mostly over in a week. Suboxone withdrawal is more like a persistent, heavy fog. Because it is long-acting, the Withdrawal Symptoms take longer to start and longer to finish, which can be mentally exhausting. However, the physical “peak” is usually less violent than that of full agonists.
Can I quit suboxone cold turkey?
Technically, you can, but we strongly advise against it. Quitting cold turkey carries a high risk of severe Opioid Withdrawal that can lead to extreme dehydration, heart palpitations, and intense psychological distress. Most importantly, the relapse rate for people who quit cold turkey is upwards of 90%. When you are in that much pain, your brain will do anything to make it stop, often leading you back to the very substances you worked so hard to quit.
When should I seek professional help for withdrawal?
You should always be under a doctor’s care when stopping Suboxone, but you should seek immediate help if you experience:
- Severe, persistent vomiting or diarrhea (which leads to dangerous dehydration)
- Thoughts of self-harm or severe suicidal ideation
- Extreme confusion or hallucinations
- Chest pain or difficulty breathing
If you are struggling with Drug Withdrawal Symptoms, professional medical detox or a supervised outpatient taper can provide the safety net you need to succeed.
Conclusion
At National Addiction Specialists, we believe that recovery shouldn’t be a punishment. Our goal is to make the transition off Suboxone as smooth and comfortable as possible. Through our telemedicine platform, we provide personalized care to patients in Tennessee and Virginia, allowing you to access expert medical support from the comfort and privacy of your own home.
Whether you are just starting your journey or are ready to discuss a tapering plan, we are here to guide you through every step of the process. Recovery is a marathon, but you don’t have to run it alone.
For more information on how we can help you navigate this transition, check out The Complete Guide to Suboxone Treatment Options.
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








