Suboxone Treatment Medicaid: Your Path to Affordable Recovery
Understanding Your Coverage: How Medicaid Supports Your Recovery
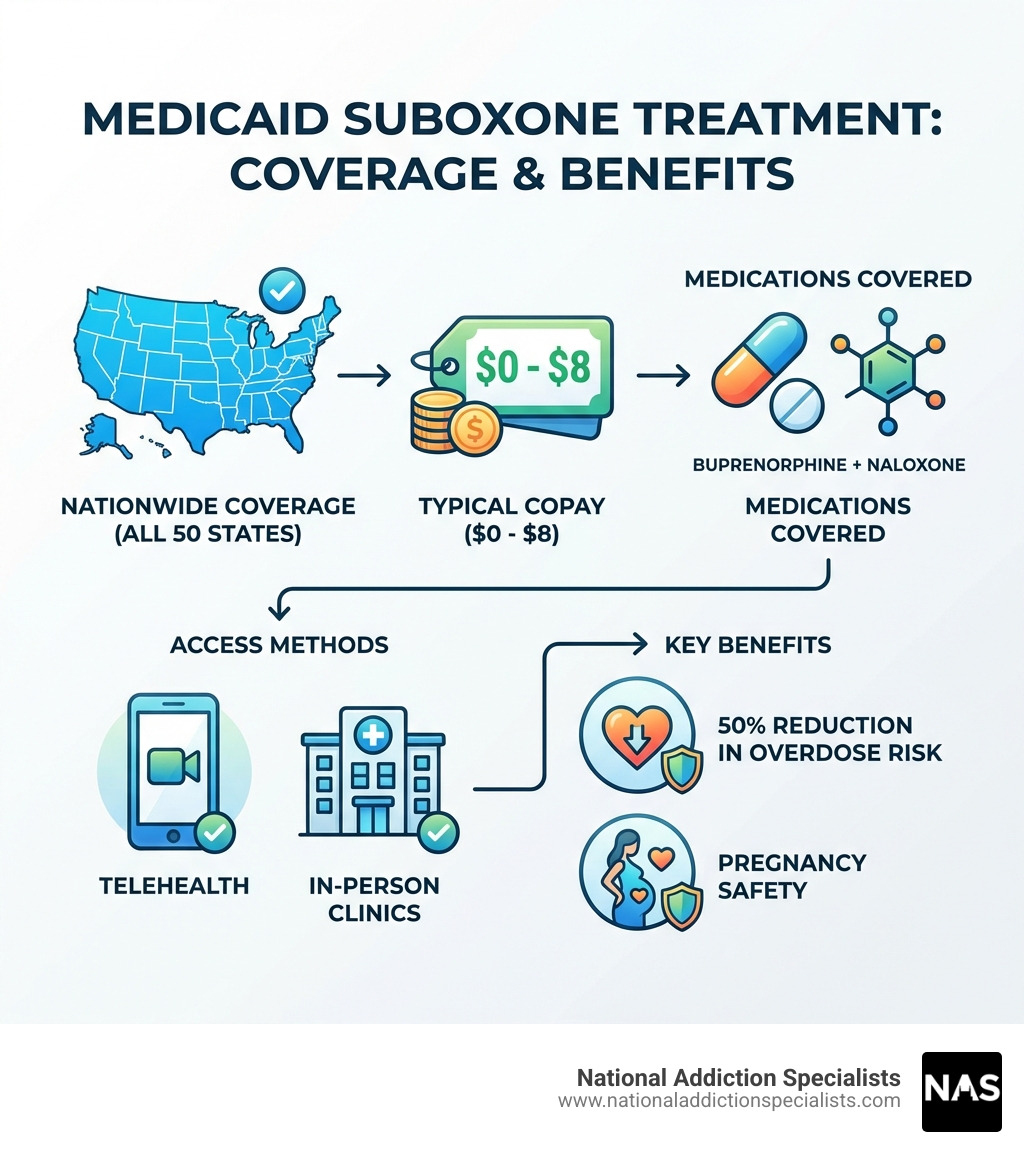
Suboxone treatment Medicaid coverage is available in all 50 states and the District of Columbia. If you’re struggling with opioid use disorder and have Medicaid, you have access to one of the most effective treatments available.
Here’s what you need to know right now:
- Universal Coverage: Medicaid covers Suboxone treatment nationwide as a mandatory benefit under the SUPPORT Act, made permanent by the Consolidated Appropriations Act (CAA) 2024
- Minimal Cost: Most Medicaid patients pay between $0-$8 per prescription, with many states charging no copay at all
- Flexible Access: Treatment is available through both in-person clinics and telehealth providers who accept Medicaid
- No Special Requirements: Any licensed prescriber with DEA registration can prescribe Suboxone since 2023, when the special waiver requirement was eliminated
- Comprehensive Care: Coverage includes both medication and counseling services in most states
The reality is simple: Medicaid wants to help you recover. With an estimated 12% of adult Medicaid beneficiaries struggling with substance use disorders, states have made medication-assisted treatment a priority. Research shows Suboxone can reduce overdose risk by up to 50%, making it a gold-standard treatment option.
You don’t need to navigate this alone. Finding a provider who accepts Medicaid is straightforward, and many offer same-day appointments through secure telehealth platforms. Whether you’re working full-time, managing family responsibilities, or simply value your privacy, there’s a treatment option that fits your life.
I’m Dr. Chad Elkin, board-certified in addiction medicine and founder of National Addiction Specialists. I’ve dedicated my career to helping patients access Suboxone treatment Medicaid covers, serving communities across Tennessee and Virginia through both in-person and telehealth services. My goal is to eliminate barriers to care and help you understand exactly what’s available to you.
Simple guide to Suboxone treatment Medicaid terms:
- Online addiction counselors
- mat clinics near me
- suboxone dr near me
Does Medicaid Cover Suboxone Treatment? The Quick Answer
The short answer is a resounding yes. Suboxone treatment Medicaid policies have evolved rapidly over the last few years to meet the growing need for accessible recovery options. Thanks to the SUPPORT Act of 2018, all state Medicaid programs were required to cover Medication-Assisted Treatment (MAT) for Opioid Use Disorder (OUD).
More recently, the Consolidated Appropriations Act (CAA) of 2024 made this mandatory coverage permanent. This means you no longer have to worry about the benefit expiring; it is now a foundational part of the Medicaid state plan. Whether you live in Tennessee or Virginia, your Medicaid plan is legally required to cover the medications, biological products, and counseling services necessary to treat OUD.
At National Addiction Specialists, we see how this Medicaid Suboxone Treatment changes lives. By removing the financial barrier, Medicaid allows individuals to focus on their health rather than how they will pay for their next dose.
| Feature | Medicaid Coverage Detail |
|---|---|
| Availability | All 50 States & DC |
| Medications Covered | Buprenorphine/Naloxone (Suboxone), Methadone, Naltrexone |
| Copay Range | $0 to $8 (State-dependent) |
| Counseling | Included (Mandatory in ~16 states) |
| Telehealth | Widely accepted and covered |
Why Suboxone is the Gold Standard for Opioid Use Disorder
If you’re researching Suboxone treatment Medicaid options, you might wonder why doctors call it the “gold standard.” Suboxone is a combination of two medications: buprenorphine and naloxone.
- Buprenorphine (The Partial Agonist): This is the primary workhorse. It attaches to the same receptors in the brain as opioids like oxycodone or heroin. However, it only partially activates them. This satisfies the brain’s “hunger” for opioids, effectively eliminating cravings and withdrawal symptoms without producing the intense “high” associated with misuse.
- Naloxone (The Deterrent): This is an opioid antagonist. It’s included to prevent misuse. If someone tries to inject the medication, the naloxone kicks in and causes immediate withdrawal symptoms. When taken properly under the tongue (sublingually), the naloxone isn’t absorbed well, allowing the buprenorphine to do its job safely.
The Substance Abuse and Mental Health Services Administration notes that MAT with Suboxone cuts overdose risk by up to 50%. It also features a “ceiling effect,” meaning that after a certain dose, taking more won’t increase the effects. This makes it significantly safer than traditional opioids or methadone. We specialize in Medicaid Opioid Treatment because we know that providing a safe, controlled environment for recovery is the most effective way to help our patients reclaim their lives.
Suboxone Treatment Medicaid and Pregnancy
One of the most compassionate aspects of Medicaid coverage is its support for pregnant individuals. For a long time, methadone was the only option, but today, Suboxone treatment Medicaid covers is considered a standard of care for pregnant women with OUD.
Research indicates that buprenorphine-based treatments lead to better neonatal outcomes. For example, babies born to mothers on buprenorphine typically have shorter hospital stays—averaging about 10 days compared to 17.5 days for those on methadone. This allows for earlier bonding and a healthier start for both mother and child. You can Learn more about buprenorphine and its safety profile through official SAMHSA resources.
Navigating State Variations and Costs for Suboxone Treatment Medicaid
While federal law mandates coverage, the “how” and “how much” can vary depending on where you live. Medicaid is a federal-state partnership, so each state has some leeway in how they manage their pharmacy benefits.

What You Will Pay
For most patients, the out-of-pocket cost is incredibly low. Typically, you will pay between $0 and $8 per prescription. Some states, like Texas, often have copays as low as $0 to $3. In Tennessee and Virginia, where we primarily operate, the goal is to keep these costs at a minimum so they never stand in the way of your sobriety.
Common Limitations
Even though coverage is universal, you might encounter some administrative “speed bumps”:
- Dosage Caps: Most states cap daily doses between 16mg and 32mg. If your doctor determines you need more, they may need to file a “prior authorization” to explain why a higher dose is medically necessary.
- Counseling Requirements: About one-third of states (roughly 16) require you to participate in counseling alongside your medication for Medicaid to continue paying for the prescription. We believe this “whole-patient” approach is best for long-term success anyway!
- Preferred Drug Lists: Medicaid programs often prefer generic buprenorphine/naloxone over the brand-name Suboxone film to save costs. The efficacy is identical, but your doctor might need to specify if there is a medical reason you need the brand name.
You can explore comprehensive state indicator data from the Kaiser Family Foundation to see exactly how your state compares. If you’re still asking Does Medicaid Cover Suboxone Treatment?, we are here to help you verify your specific plan benefits.
Key State Examples: Texas, Tennessee, and Virginia
Let’s look at a few specific examples of how Suboxone treatment Medicaid works on the ground.
Texas In places like Dallas County, the opioid crisis is a significant concern. In 2021 alone, Dallas County reported over 500 opioid overdose deaths. Texas Medicaid covers buprenorphine/naloxone with very low copays. Approximately 6,000 individuals received MAT in Dallas County in 2022, showing that the system is working to get people into care.
Tennessee (TennCare) Tennessee has been at the forefront of the opioid epidemic response. TennCare (the state’s Medicaid program) provides robust coverage for Suboxone. Because we have locations in Brentwood and serve the entire state of Tennessee, we understand the nuances of TennCare’s requirements, including their office-based buprenorphine treatment guidelines.
Virginia With our presence in Virginia Beach and across Virginia, we see how the state’s Medicaid expansion has opened doors for thousands. Virginia Medicaid covers all FDA-approved OUD medications, and we work closely with the state’s guidelines to ensure our patients get their prescriptions filled without delay.
Finding Suboxone Doctors Near Me That Accept Medicaid is the first step toward utilizing these state benefits.
How to Access Treatment via Telemedicine
One of the biggest breakthroughs in addiction medicine has been the expansion of telehealth. Before the COVID-19 pandemic, the Ryan Haight Act required an in-person visit before a doctor could prescribe controlled substances like Suboxone. However, emergency flexibilities changed that, and many of these changes have been extended or made permanent.
Today, you can access Suboxone treatment Medicaid covers from the comfort of your own home. This is a game-changer for:
- Rural residents who might live hours away from the nearest clinic.
- Busy professionals who can’t take half a day off for an appointment.
- Parents who struggle with childcare.
- Individuals seeking privacy who prefer not to be seen walking into a local clinic.
The telehealth visits only(DEA068)%20DEA%20SAMHSA%20buprenorphine%20telemedicine%20%20(Final)%20+Esign.pdf) model allows us to provide the same high level of care virtually. At National Addiction Specialists, we specialize in this Medicaid Suboxone Treatment 2 model, ensuring our Tennessee and Virginia patients have a direct line to expert care.
Step-by-Step Guide to Starting Suboxone Treatment Medicaid Online
Getting started doesn’t have to be overwhelming. Follow these steps to begin your journey:
- Verify Your Coverage: Ensure your Medicaid plan is active. You can call the number on the back of your card or check your state’s online portal.
- Find a Qualified Provider: Use the SAMHSA Treatment Locator and filter for “Buprenorphine Practitioners” and “Medicaid.” Or, simply reach out to us—we specialize in accepting Medicaid for virtual visits.
- Schedule Your Intake: During your first virtual appointment, a doctor will review your medical history and current opioid use. This is a judgment-free zone; we are here to help, not criticize.
- The Induction Phase: You will need to be in mild withdrawal before taking your first dose to avoid “precipitated withdrawal.” Your doctor will guide you through this carefully.
- Pick Up Your Prescription: Once approved, your prescription is sent electronically to a pharmacy near you. Because of our streamlined process, we often see Medicaid Suboxone Treatment 3 patients get their first dose the very same day.
Conclusion
Recovery is a journey, but it doesn’t have to be a lonely or expensive one. Suboxone treatment Medicaid coverage is a powerful tool designed to help you succeed. By combining the “gold-standard” medication with the convenience of telemedicine, National Addiction Specialists provides a path to recovery that fits into your real life.
We are proud to serve the communities of Tennessee (including Brentwood) and Virginia (including Virginia Beach). Our team is dedicated to providing personalized, confidential care that respects your dignity and supports your goals.
If you’re ready to take the next step, we’re ready to walk with you. You can find More info about insurance and pricing on our website to see how we make recovery affordable and accessible.
Frequently Asked Questions
How much will I pay at the pharmacy for Suboxone with Medicaid?
Most patients pay a very small copay, typically between $0 and $8. In many cases, especially with generic versions of the medication, the cost is $0. Your specific state policy and whether you have a managed care plan (MCO) will determine the exact amount, but it is designed to be the most affordable way to access MAT.
Can I switch to Suboxone under Medicaid coverage?
Yes! Many patients switch from methadone to Suboxone because Suboxone allows for monthly prescriptions and doesn’t require daily visits to a clinic. This transition must be supervised by a doctor, as you typically need to taper your methadone dose and wait for a specific period of withdrawal before starting Suboxone to ensure safety and comfort.
Does Medicaid cover Suboxone treatment if I use telehealth?
Absolutely. Medicaid programs in Tennessee and Virginia recognize the value of telehealth. Online addiction medicine doctors are legitimate, highly trained professionals. As long as the provider is licensed in your state and accepts your Medicaid plan, your virtual visits and the resulting prescriptions should be covered just like an in-person visit.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








