Suboxone Treatment at Home Made Simple
Getting Suboxone Treatment at Home Is Now Possible — Here’s What You Need to Know
Suboxone treatment at home is a legitimate, medically supervised option for people dealing with opioid use disorder (OUD). You don’t need to visit a clinic every day. A licensed provider can assess you, prescribe Suboxone, and monitor your progress — all through a secure video call.
Here’s how it works in a nutshell:
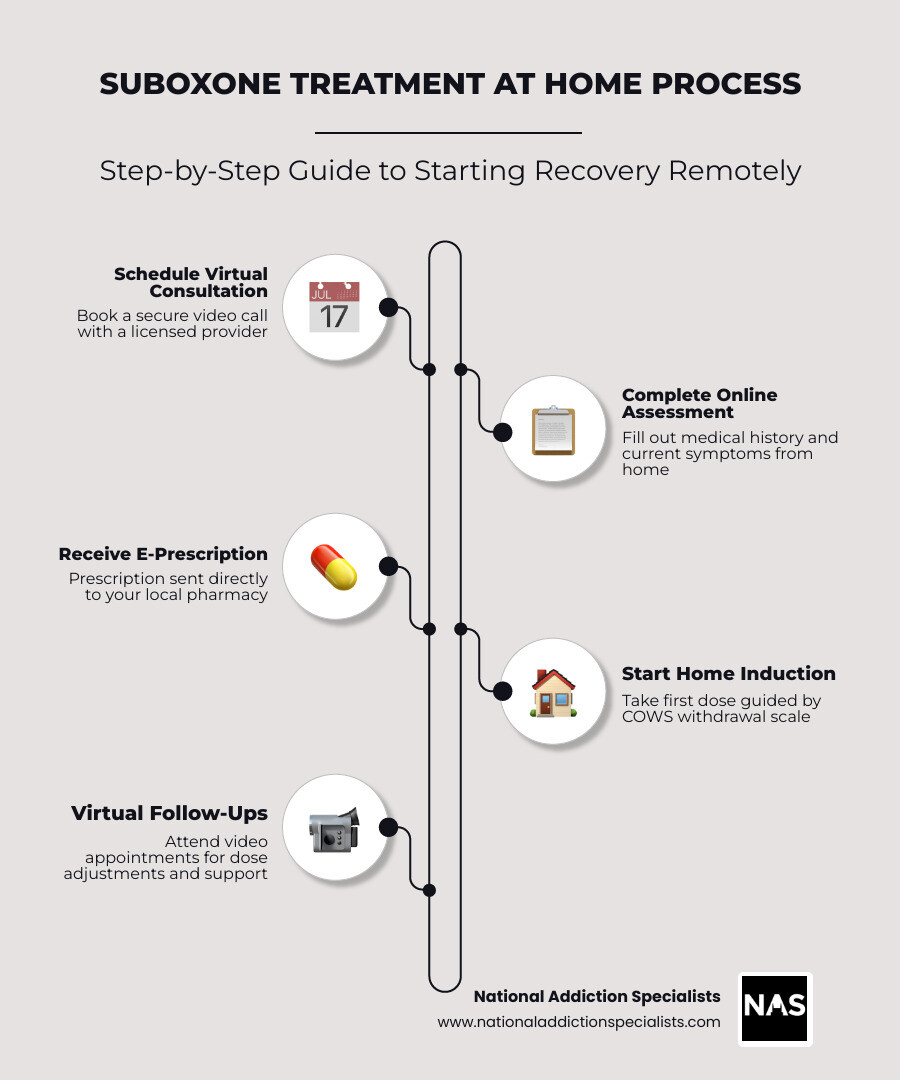
- Schedule a virtual consultation with a licensed addiction medicine provider
- Complete your initial assessment online, from home
- Receive your Suboxone prescription sent electronically to your local pharmacy
- Begin the induction phase at home under medical guidance
- Attend follow-up appointments virtually for dose adjustments and ongoing support
This approach is backed by real evidence. Medication-Assisted Treatment (MAT) reduces opioid overdoses by 76%, and without medication, opioid addiction treatment fails about 90% of the time. Telehealth makes it possible to access this gold-standard care privately, on your schedule.
I’m Chad Elkin, MD, Founder and Medical Director of National Addiction Specialists, board-certified in both Addiction Medicine and Internal Medicine, with years of hands-on experience helping patients access suboxone treatment at home through telehealth. In the sections below, I’ll walk you through everything you need to know — from how Suboxone works to how to start your first appointment today.
What is Suboxone and How Does It Work?
To understand why suboxone treatment at home is so effective, we first need to look at what the medication actually is. What is Suboxone? It is a combination of two specific ingredients: Buprenorphine and Naloxone. This combination is specifically designed to treat opioid use disorder (OUD) by addressing both the physical and behavioral aspects of addiction.
Buprenorphine: The Partial Agonist
Buprenorphine is the primary active ingredient. It is a “partial opioid agonist.” In simple terms, it sticks to the same receptors in the brain that opioids like heroin or oxycodone do. However, because it is only a partial agonist, it doesn’t produce the intense “high” or the dangerous respiratory depression associated with full opioids. Instead, it “quiets” the brain’s receptors, effectively eliminating cravings and preventing withdrawal symptoms.
Naloxone: The Safety Guard
Naloxone is added as an abuse deterrent. If Suboxone is taken as directed (dissolved under the tongue), the Naloxone is not absorbed into the bloodstream in significant amounts. However, if someone tries to inject the medication, the Naloxone activates, blocking the opioid receptors and triggering immediate withdrawal. This makes Suboxone much safer than older treatments.
How Does Suboxone Treatment Work? Essentially, it acts as a “reset button” for your brain chemistry. By stabilizing these receptors, it allows you to feel “normal” again, so you can focus on rebuilding your life rather than chasing the next dose. The FDA information on Medication-Assisted Treatment confirms that MAT is the gold standard for OUD, helping patients maintain long-term recovery.
The Benefits of Suboxone Treatment at Home
Choosing suboxone treatment at home over traditional clinic-based models (like methadone clinics) offers several life-changing advantages. For many of our patients in Tennessee and Virginia, the transition to home-based care is what finally makes recovery stick.
- Privacy and Stigma Reduction: One of the biggest hurdles to seeking help is the fear of being seen at a “rehab clinic.” Benefits of Suboxone Treatment at home include complete confidentiality. Your neighbors and coworkers don’t need to know you are in treatment.
- Convenience and Flexibility: Traditional methadone treatment often requires daily visits to a clinic, which can be impossible if you have a job or children to care for. With Telehealth Suboxone Treatment, your “clinic” is your living room.
- Increased Access: In rural parts of Tennessee or Virginia, the nearest specialist might be hours away. Telehealth removes the transportation barrier, ensuring that high-quality medical care is available regardless of your zip code.
- Safety and Comfort: Withdrawing from opioids is incredibly uncomfortable. Being able to manage this process in your own bed, with your own comforts around you, significantly reduces the stress of early recovery.
How to Start Your Recovery Journey Remotely
Starting suboxone treatment at home is designed to be a streamlined, stress-free process. We know that when you’re ready to quit, you need help now, not in three weeks.
The process begins with an initial assessment. You’ll meet with Online Suboxone Doctors who will review your medical history, your history of substance use, and your current physical state. This is a judgment-free zone; our goal is simply to create a plan that keeps you safe and comfortable.
At National Addiction Specialists, we often provide Same-Day Suboxone Treatment Online. Once the doctor determines you are a good candidate, they will send an electronic prescription to a pharmacy near you in Brentwood, Virginia Beach, or wherever you are located in TN or VA.
The Induction Phase of Suboxone Treatment at Home
The most critical part of starting suboxone treatment at home is the “induction” phase. This is the period when you transition from your previous opioid to Suboxone.
To avoid “precipitated withdrawal”—which is a sudden, intense onset of withdrawal symptoms caused by taking Suboxone too early—you must be in a state of moderate withdrawal before your first dose. We use a tool called the COWS (Clinical Opiate Withdrawal Scale) to help you determine the right time. You will look for symptoms like:
- Restlessness and anxiety
- Muscle aches and “gooseflesh”
- Nausea or stomach cramps
- Yawning and watery eyes
Once you reach a specific score on the scale, you’ll take your first small dose. Your At Home Suboxone Treatment plan will include clear instructions on how to titrate (slowly increase) your dose over the first 48 hours until your symptoms disappear.
Dosing and Stabilization for Suboxone Treatment at Home
After the first few days, you enter the stabilization phase. Your doctor will work with you to find the “sweet spot”—the dose that stops all cravings and withdrawal symptoms without making you feel sedated.
Suboxone for Opioid Addiction is not about replacing one addiction with another; it’s about using a long-acting medication to stabilize your brain so you can function. Once stabilized, most patients move into a maintenance phase, where they take the same dose daily and check in with us via telehealth once or twice a month.
Safety, Side Effects, and Success Rates
Safety is our top priority. While suboxone treatment at home is very safe, it is still a powerful medication.
Side Effects
Common side effects are usually mild and often go away as your body adjusts. According to Suboxone safety and side effect information, these can include:
- Headaches
- Nausea or constipation
- Insomnia
- Sweating
Statistics and Success
The data on telehealth-based Suboxone is incredibly encouraging. Research shows that approximately 83% of patients receiving tele-buprenorphine treatment had a follow-up visit within 30 days, which is an exceptionally high rate of engagement. Furthermore, tele-buprenorphine follow-up statistics indicate that patients using telehealth are just as likely—if not more likely—to stay in treatment compared to those using traditional in-person clinics.
One study found that after a 90-day program, opioid use among participants decreased by over 32%. More importantly, MAT is proven to reduce the risk of a fatal overdose by 76%. These aren’t just numbers; they represent lives saved and families kept together.
Frequently Asked Questions about At-Home Care
We understand you probably have many questions before starting Suboxone Treatment FAQ. Here are the most common concerns we hear:
Who is eligible for home-based treatment?
Most people with a history of opioid use are eligible for suboxone treatment at home. During your intake, we look at your medical history and psychiatric stability. While telehealth is a great fit for most, some individuals with severe, unstable medical conditions or acute suicidal ideation may be referred to a higher level of in-person care for their own safety.
Does insurance cover the cost of treatment?
Yes! At National Addiction Specialists, we believe cost should never be a barrier to recovery. We accept Medicaid and Medicare, as well as many private insurance plans. For those without insurance, we offer affordable self-pay options. In many cases, patients find that the cost of treatment is significantly less than what they were spending on illicit substances.
How long does Suboxone treatment typically last?
There is no “one size fits all” timeline. Some people use Suboxone for a few months to get through the initial hurdles of recovery, while others remain on a maintenance dose for years. Research suggests that longer-term treatment (6 months or more) leads to better outcomes and lower relapse rates. We will work with you to decide when—or if—it is the right time to begin a slow, medically supervised taper.
Conclusion
Recovery doesn’t have to be a battle you fight in a crowded waiting room. At National Addiction Specialists, we provide At-Home Addiction Recovery that is personalized, confidential, and convenient. Whether you are in Brentwood, TN, or Virginia Beach, VA, our expert team is here to help you regain control of your life.
Suboxone treatment at home is more than just a convenience—it’s a gold-standard medical intervention that meets you exactly where you are.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. Make an Appointment
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.









