Understanding Your Options for Opioid Use Disorder
When considering treatment for opioid addiction, the safety of Subutex vs Suboxone evidence-based comparison reveals key differences that matter for your recovery.
Quick Safety Comparison:
| Factor | Subutex | Suboxone |
|---|---|---|
| Active Ingredients | Buprenorphine only | Buprenorphine + Naloxone |
| Misuse Potential | Moderate (if diverted) | Lower (naloxone deters injection) |
| Overdose Risk | Low (ceiling effect) | Low (ceiling effect) |
| Pregnancy Use | Preferred | Generally avoided |
| Current Availability | Limited/special cases | Standard of care |
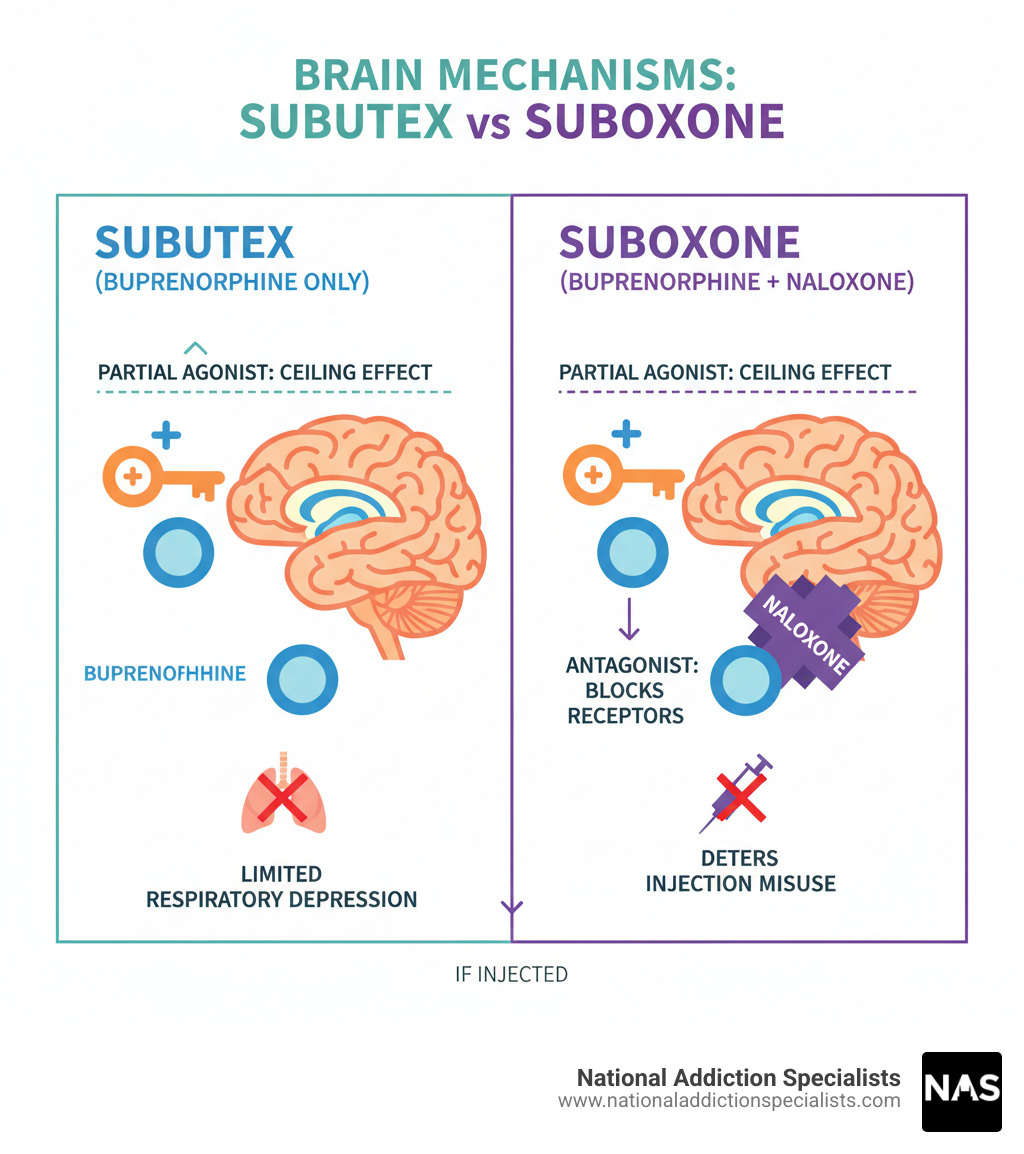
Both medications contain buprenorphine, a partial opioid agonist that reduces cravings and withdrawal symptoms with a built-in safety ceiling. The key difference is that Suboxone adds naloxone, which blocks opioid effects if the medication is crushed and injected. This makes Suboxone less likely to be misused.
Combined buprenorphine/naloxone medications are preferred over buprenorphine monotherapy because of their lower abuse potential, except for pregnant patients, those breastfeeding, or individuals allergic to naloxone.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists, where I’ve helped thousands of patients steer the safety of Subutex vs Suboxone evidence-based comparison to find their path to recovery. My work with state and national addiction medicine organizations has given me deep insight into how these medications work in real-world treatment settings.
Safety of subutex vs suboxone evidence-based comparison terms to know:
The Core Difference: Formulation and Ingredients
Subutex and Suboxone are key medications for Medication-Assisted Treatment (MAT) for Opioid Use Disorder (OUD). Both rely on buprenorphine, but their different formulations affect their safety and how they are prescribed.
Subutex, a former brand name, contains only buprenorphine. It provides the benefits of buprenorphine—easing cravings and withdrawal—without any misuse-deterrent ingredients. It was typically an under-the-tongue tablet.
Suboxone combines buprenorphine and naloxone, available as films or tablets that dissolve under the tongue. The addition of naloxone is the key difference and central to the safety of Subutex vs Suboxone evidence-based comparison.

The Role of Naloxone in Suboxone’s Safety Profile
Naloxone is an opioid antagonist that acts as a misuse deterrent in Suboxone. When taken as prescribed by dissolving it under the tongue, very little naloxone is absorbed, allowing buprenorphine to work effectively against cravings and withdrawal.
However, if someone misuses Suboxone by injecting it, the naloxone becomes fully active. As an opioid blocker, it immediately triggers unpleasant precipitated withdrawal symptoms. This mechanism is designed to discourage injection. The Substance Abuse and Mental Health Services Administration (SAMHSA) confirms naloxone is added to prevent misuse. You can learn more about naloxone’s role in MAT from SAMHSA here: SAMHSA information on Naloxone.
This built-in safety feature gives Suboxone a lower chance of being misused, making it a safer choice than buprenorphine-only options like Subutex.
How Buprenorphine’s “Ceiling Effect” Improves Safety
Buprenorphine itself has a key safety feature called the “ceiling effect.” As a partial opioid agonist, it activates opioid receptors less than full agonists like heroin. After a certain dose, its effects plateau and do not increase, which provides several safety benefits:
- Less Euphoria: It produces less of a “high,” making it less appealing for misuse.
- Lowered Overdose Risk: Crucially, it limits respiratory depression (slowed breathing), the main cause of opioid overdose deaths. This makes it much safer than full opioids when taken as prescribed.
- Fewer Severe Side Effects: It generally causes less physical dependence and fewer severe side effects compared to full opioids.
While buprenorphine is safer, an overdose is still possible if mixed with other central nervous system depressants like benzodiazepines or alcohol. The National Institute on Drug Abuse (NIDA) highlights buprenorphine’s safety when used correctly. This unique feature is why buprenorphine-based medications are effective and safe tools for treating OUD. You can find more information about how these medications work on the NIDA website: NIDA research on how MAT medications work.
The Safety of Subutex vs. Suboxone: An Evidence-Based Comparison
In the safety of Subutex vs Suboxone evidence-based comparison, medical evidence clearly favors Suboxone for most patients. This preference is backed by clinical guidelines, patient outcomes, and extensive research.
The key difference is naloxone. While both share buprenorphine’s therapeutic benefits, Suboxone’s naloxone provides a built-in safety feature that reduces misuse and diversion risk.
Here’s how they compare on key safety factors:
| Factor | Subutex (Buprenorphine Monotherapy) | Suboxone (Buprenorphine + Naloxone) |
|---|---|---|
| Active Ingredients | Buprenorphine only | Buprenorphine + Naloxone |
| Misuse Potential | Moderate (if diverted and injected, can produce opioid effects) | Lower (naloxone triggers precipitated withdrawal if injected) |
| Use in Pregnancy | Often preferred by some clinicians to avoid fetal naloxone exposure, though methadone is the standard | Generally avoided unless other options are not suitable or available |
| Primary Use Case | Special populations (pregnancy, naloxone allergy, supervised settings) | Standard of care for most OUD treatment |
The overdose potential for both medications is relatively low when used as prescribed, thanks to buprenorphine’s ceiling effect. However, Suboxone’s formulation provides an extra layer of protection against misuse that makes it the safer choice for most treatment scenarios.
Common Side Effects and Potential Contraindications
Since buprenorphine is the main active ingredient in both, Subutex and Suboxone cause similar, generally mild side effects compared to full opioids. Common side effects include headache, nausea, and constipation. Some patients also experience drowsiness or insomnia, muscle aches, or irritability, especially early in treatment.
Serious drug interactions are a major concern. Combining buprenorphine with central nervous system depressants like benzodiazepines, alcohol, or other sedatives significantly increases the risk of respiratory depression, severe sedation, coma, and even death. This is a critical safety consideration for every patient.
We also pay close attention to liver function monitoring. While mild to moderate liver issues don’t always prevent treatment, we must be cautious and regularly check liver health. Buprenorphine can also affect heart rhythm, particularly at higher doses, so we carefully monitor patients with pre-existing heart conditions.
Before starting treatment, we conduct a thorough review of your medical history and current medications to identify any potential contraindications. This personalized approach ensures your treatment is as safe as possible.
Evidence-Based Comparison of Misuse and Diversion
Real-world misuse and diversion data clearly highlight Suboxone’s superior design in the safety of Subutex vs Suboxone evidence-based comparison.
Subutex diversion remains a concern. Because it contains only buprenorphine, it can be misused for euphoric effects, especially if crushed and injected. The risk is moderate with take-home doses due to the lack of a built-in deterrent.
Suboxone’s deterrent effect changes this equation. If someone tries to inject or snort Suboxone, the naloxone rapidly enters their bloodstream and triggers immediate, intense precipitated withdrawal. This makes Suboxone far less appealing for illicit use. The National Institute on Drug Abuse (NIDA) specifically highlights that buprenorphine/naloxone formulations like Suboxone are highly effective in reducing illicit opioid use and supporting long-term recovery.
The professional consensus is clear: Suboxone’s formulation makes it the preferred choice for most patients. Buprenorphine monotherapy is typically reserved for supervised settings—like hospitals or residential facilities—or for specific medical reasons like pregnancy.
While Subutex is safe when used appropriately, Suboxone provides an extra layer of protection against diversion and misuse in most outpatient settings, benefiting both patients and communities.
Clinical Applications: Who Gets Prescribed Which Medication?
Deciding between Subutex (or generic buprenorphine monotherapy) and Suboxone (buprenorphine/naloxone) is a careful process. It’s guided by medical best practices, what’s best for each patient, and your doctor’s expert judgment. Here at National Addiction Specialists, our main goal is always to create a personalized treatment plan. We want to ensure you have the safest and most effective path to lasting recovery.
Your journey with buprenorphine-based medications usually unfolds in three key steps. First, there’s the induction phase. This is when you start taking the medication. It’s really important that you’re in a mild to moderate state of opioid withdrawal before your first dose of buprenorphine. This helps prevent something called “precipitated withdrawal,” which we definitely want to avoid! Next, you’ll move into the stabilization phase. This happens once you’ve stopped or greatly reduced using illicit opioids, your cravings are under control, and you’re feeling good with minimal side effects. Finally, you’ll reach the maintenance phase. In this step, you’ll be on a steady dose, and the length of your treatment is completely custom. It can even continue indefinitely, helping you maintain your long-term recovery.

Safety of Subutex vs. Suboxone in Special Populations
While Suboxone is typically the first choice for most patients, there are special situations where buprenorphine monotherapy, like generic Subutex, might be a better fit. These are specific cases where the safety of Subutex vs Suboxone evidence-based comparison leans towards the monotherapy.
The most common reason for choosing buprenorphine monotherapy is during pregnancy and lactation. The main concern here is to avoid any potential exposure of naloxone to the developing baby or nursing infant. While methadone is still considered the standard for pregnant women with opioid dependency in the U.S. (as per SAMHSA guidelines), some doctors might prefer buprenorphine monotherapy. This is to avoid even a theoretical risk of naloxone exposure for the baby. It’s a very important decision, made with careful consideration and often in partnership with specialists, to ensure the best health for both mom and child.
Another rare but important instance is for a patient with a documented naloxone allergy. If someone has a confirmed allergy or a very bad reaction to naloxone, buprenorphine monotherapy would be the clear choice. In these unique situations, the benefits of avoiding naloxone are greater than the deterrent effect it offers against misuse. This is why we consider monotherapy.
Availability and Modern Prescribing Practices
You might recall the brand name Subutex, which was the original buprenorphine monotherapy. It was actually discontinued in the U.S. back in 2011. However, generic versions of buprenorphine monotherapy are still very much available and prescribed when needed, especially for the special populations we just talked about. For the vast majority of people seeking help with OUD, Suboxone (buprenorphine/naloxone) has become the go-to treatment.
The way we treat opioid addiction changed significantly with the Drug Addiction Treatment Act of 2000 (DATA 2000). This important law allowed qualified doctors to prescribe buprenorphine for OUD right in their offices. This was a huge step, making treatment much more accessible than just traditional clinics like methadone programs. This shift has opened doors for us to offer convenient, private care, including telemedicine-based Suboxone treatment, to patients across Tennessee and Virginia. It means you can get the help you need, often from the comfort of your own home.
Make an Appointment to Treat Addiction
If you’re ready to take the first step towards recovery, we’re here to help. Our compassionate providers in Tennessee and Virginia specialize in medication-assisted treatment that fits your life. Please don’t hesitate. Make an appointment today.
More info about starting treatment
Efficacy, Outcomes, and the Professional Consensus
When we look at the safety of Subutex vs Suboxone evidence-based comparison, we need to think beyond just the immediate effects. What really matters is how well these medications work over time and how they help people build lasting recovery. The good news? Both medications, when used as part of a comprehensive treatment plan, have strong track records for helping people stay in treatment, stop using illicit opioids, and reclaim their lives.
Here’s something I’ve seen time and again in my practice: medication alone isn’t the full answer. The research backs this up completely. Buprenorphine-based treatment works best when it’s paired with counseling and social support. Think of the medication as stabilizing the foundation—it quiets the cravings and withdrawal symptoms—while counseling helps you build the life skills and emotional tools you need for long-term success. At National Addiction Specialists, this comprehensive approach isn’t just something we recommend; it’s how we structure every treatment plan.
Are Subutex and Suboxone Equally Effective?
Let’s get to the heart of it: when taken as prescribed, the buprenorphine in both Subutex and Suboxone does the same job. It reduces cravings, eases withdrawal symptoms, and helps stabilize your brain chemistry. From a pure efficacy standpoint, clinical trials show no significant difference between buprenorphine monotherapy and the combination product when we’re measuring their ability to manage opioid dependence.
The buprenorphine component is doing the heavy lifting in both medications. The real differences in patient outcomes often come down to patient adherence—how consistently people take their medication—and whether they’re also getting counseling and behavioral support.
One important study published in JAMA made a crucial point about treatment duration. Researchers found that maintenance therapy (staying on medication long-term) led to much better outcomes than trying to taper off quickly. This held true regardless of which specific buprenorphine formulation patients were using. The message was clear: sustained treatment matters. You can read more about this research here: JAMA study on maintenance vs. taper therapy.
This aligns with what we see every day in practice. Buprenorphine treatment isn’t meant to be a short-term fix. Long-term recovery success is strongly connected to staying in treatment for as long as you need it—which might mean months, years, or even indefinitely. There’s no shame in that. We’re treating a chronic condition, and ongoing management is often the path to lasting wellness.
The Current Medical Recommendation
So with all this information, what do the experts recommend? The professional consensus is clear: Suboxone (buprenorphine/naloxone) is the preferred choice for most patients seeking treatment for opioid use disorder. The reason comes back to safety—specifically, its lower abuse potential.
That naloxone component we’ve talked about throughout this article? It’s a game-changer for reducing diversion and misuse in the community. When someone tries to inject Suboxone, the naloxone triggers immediate withdrawal, making it far less appealing on the illicit market. This built-in safety feature gives Suboxone an edge in real-world settings where medication might be diverted or misused.
Both SAMHSA (the Substance Abuse and Mental Health Services Administration) and ASAM (the American Society of Addiction Medicine) recommend buprenorphine/naloxone formulations as the standard of care. These aren’t just arbitrary guidelines—they’re based on years of research and clinical experience showing that combination products offer better safety profiles without sacrificing effectiveness.
These organizations also emphasize something we believe deeply: medication is just one part of comprehensive treatment plans. The role of counseling, behavioral therapy, peer support, and addressing the whole person—not just the addiction—is essential. We can prescribe the safest, most effective medication available, but recovery happens when you’re also getting the emotional and psychological support you need.
At National Addiction Specialists, we align completely with these SAMHSA recommendations and ASAM guidelines. We’re here to provide accessible, evidence-based care through telemedicine, making it easier for people in Tennessee and Virginia to get the treatment they deserve. Our approach combines the safety of Suboxone with personalized counseling and ongoing support, all from the comfort and privacy of your own home.
Frequently Asked Questions
We understand that choosing the right medication for opioid use disorder involves careful consideration, and you likely have questions about the safety of Subutex vs Suboxone evidence-based comparison. Let’s address some of the most common concerns we hear from patients.
Can you overdose on Subutex or Suboxone?
This is one of the most important questions we’re asked, and the answer requires some nuance. Yes, overdose is possible, but the risk is significantly lower than with full opioid agonists like heroin or prescription painkillers—thanks to buprenorphine’s unique “ceiling effect.”
When buprenorphine is used alone and as prescribed, the ceiling effect limits respiratory depression once a certain dose is reached. This means taking more buprenorphine beyond that point doesn’t significantly increase the risk of slowed breathing, which is what typically causes death in opioid overdoses. This built-in safety feature makes both Subutex and Suboxone much safer than many other opioids.
However—and this is crucial—the risk changes dramatically when buprenorphine is combined with other central nervous system depressants. Benzodiazepines like Xanax, Klonopin, or Valium are particularly dangerous when mixed with buprenorphine. Alcohol, even in small amounts, can dangerously amplify the sedative effects. Other sedatives, tranquilizers, or any substance that slows brain activity also poses serious risks.
Polysubstance use—combining buprenorphine with these other substances—can dramatically increase the risk of overdose, severe sedation, coma, and death. This is why we always conduct a thorough review of all medications and substances you’re taking. Your safety depends on honest communication with your healthcare provider about everything you’re using.
Is Subutex still commonly prescribed today?
The short answer is no, not commonly. The brand name Subutex was actually discontinued in the United States back in 2011. While generic buprenorphine monotherapy remains available, it’s now reserved for very specific, limited circumstances rather than routine treatment.
Today, you’ll typically see buprenorphine monotherapy prescribed in a few situations: during pregnancy and lactation, where some clinicians prefer to avoid any potential naloxone exposure to the fetus or nursing infant; for patients with a documented naloxone allergy, which is rare but does occur; or in highly supervised settings like hospitals or specialized treatment facilities where the risk of diversion and misuse can be more tightly controlled.
For the vast majority of patients seeking treatment for opioid use disorder, buprenorphine/naloxone combination products like Suboxone have become the standard of care. The shift happened because of Suboxone’s improved safety profile—specifically, the naloxone component that deters misuse. This represents the evolution of best practices in addiction medicine, and it’s why we at National Addiction Specialists primarily prescribe combination products for most of our patients in Tennessee and Virginia.
The availability of generic formulations means that when monotherapy is clinically appropriate, it’s still accessible. But the medical community’s consensus is clear: combination products offer better protection against misuse while providing the same therapeutic benefits for managing opioid use disorder.
Conclusion: Making the Safest Choice for Your Recovery
Navigating the path to recovery from opioid use disorder can feel like a big journey. But understanding your treatment options, especially the safety of Subutex vs Suboxone evidence-based comparison, is a powerful step. We hope this guide has helped clarify the differences and why one option is often preferred.
Both Subutex (generic buprenorphine monotherapy) and Suboxone (buprenorphine/naloxone) are truly valuable tools. They both use buprenorphine to help ease cravings and withdrawal, giving you a chance to rebuild your life.
For most people, Suboxone is the recommended choice. That’s because the added naloxone acts like a helpful guardian. It makes the medication less likely to be misused, especially if someone tries to inject it. This built-in safety feature helps protect both the individual and the community.
While generic buprenorphine monotherapy (like Subutex) has a specific role, it’s usually for special situations. Think about pregnant individuals, those with a rare naloxone allergy, or patients in very closely watched settings. For everyone else, Suboxone is generally the standard of care.
Your recovery journey is unique, and the best choice for you will always be a personal one. It needs careful guidance from a medical expert who understands your specific needs and situation.
At National Addiction Specialists, we believe in making this expert care accessible and easy. We offer convenient, confidential, and evidence-based treatment through telemedicine, right here in Tennessee and Virginia. Our caring providers are ready to work with you. We’ll help create a personalized treatment plan that gives you the right medication and support for lasting recovery.
Ready to take control of your future?
Start your recovery journey with us today.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.