Restoring Your Zzz’s: Sleep Strategies for a Sober Life
Why Quality Sleep is Essential in Recovery
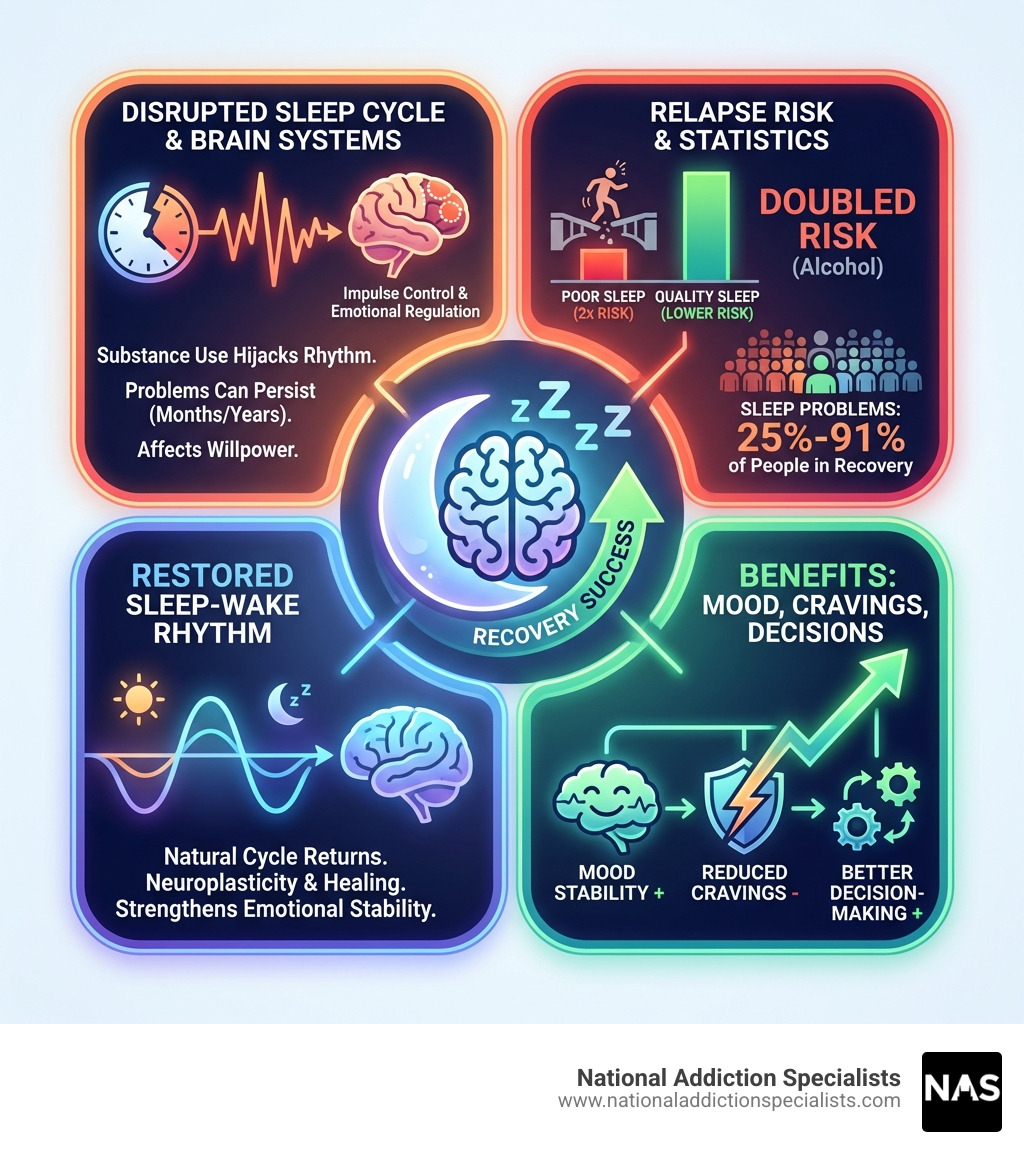
Addiction recovery sleep is one of the most overlooked yet critical components of successful sobriety. When you’re recovering from substance use, your body and brain desperately need restorative rest to heal, but sleep problems affect between 25% and 91% of people in recovery—making it one of the most common challenges you’ll face.
Quick Answer: Key Facts About Addiction Recovery Sleep
- Sleep disruption is universal: Every substance withdrawal—alcohol, opioids, stimulants, marijuana—includes sleep problems as a core symptom
- Relapse risk doubles: People recovering from alcohol addiction are twice as likely to relapse when not getting enough sleep
- Problems persist: Sleep issues can last months or even years after you stop using substances
- Recovery depends on it: Quality sleep improves decision-making, reduces cravings, and strengthens emotional stability
- Treatment helps: Cognitive behavioral therapy for insomnia (CBT-I), sleep hygiene, and proper screening can significantly improve outcomes
The connection between sleep and addiction works both ways. Substance use disrupts your natural sleep-wake cycle, leading to insomnia, fragmented sleep, or excessive daytime sleepiness. But poor sleep also increases your vulnerability to relapse by weakening willpower, intensifying cravings, and impairing the judgment you need to stay sober.
Research shows that sleep deprivation affects the same brain systems involved in addiction—including impulse control, emotional regulation, and stress response. When you don’t sleep well, your brain’s ability to resist cravings drops significantly. This creates a dangerous cycle where addiction disrupts sleep, and sleep problems fuel continued substance use or relapse.
The good news? Prioritizing sleep can be a powerful tool in your recovery toolkit. From simple sleep hygiene strategies to evidence-based therapies, there are proven ways to restore healthy rest patterns and strengthen your sobriety.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists, where I’ve spent over a decade helping people overcome substance use disorders. Through my clinical work and leadership in addiction medicine, I’ve seen how addressing addiction recovery sleep issues can transform recovery outcomes and reduce relapse risk.
The Science of Addiction Recovery Sleep
To understand why we struggle so much with sleep in early sobriety, we have to look at what substances do to the brain’s “wiring.” Addiction is essentially a brain disease that hijacks the reward system and the arousal system. When we stop using, the brain doesn’t just “reset” overnight. It takes time for neuroplasticity—the brain’s ability to reorganize itself—to kick in and heal the damage.
One of the biggest problems is the increased risk of relapse tied to exhaustion. When you are sleep-deprived, your prefrontal cortex (the part of the brain responsible for executive function and self-control) begins to underperform. It’s like trying to drive a car with a dying battery; eventually, the systems you rely on to make good decisions just won’t start. Scientific research on polysomnographic predictors of relapse confirms that specific sleep patterns, such as increased REM pressure and long delays in falling asleep, can actually predict who is more likely to return to use.
Furthermore, Scientific research on insomnia and alcoholism highlights that for those with Alcohol Use Disorder (AUD), sleep complaints are not just a nuisance; they are a clinical marker for the severity of the dependence and a major trigger for “self-medicating” with a drink just to get some rest.
Why Quality Sleep is Crucial for Addiction Recovery Sleep
Why are we so focused on addiction recovery sleep? Because sleep is the foundation of every other recovery tool you use.
- Emotional Regulation: Ever notice how a bad night’s sleep makes you irritable? In recovery, that irritability can turn into a full-blown emotional crisis.
- Impulse Control: Sleep restores the brain’s ability to say “no.” Without it, the “go” system of addiction runs wild.
- Cravings: Lack of sleep increases the hormone ghrelin and disrupts dopamine, making cravings feel more physical and harder to ignore.
- Physical and Spiritual Healing: Sleep is when the body repairs tissues and the mind processes the trauma often associated with active addiction.
Neurobiological Mechanisms of Addiction Recovery Sleep
The link between sleep and addiction is deeply rooted in our biology.
- Dopamine D2 Receptors: Chronic drug use downregulates dopamine receptors. Sleep deprivation does the same thing, making it harder to feel pleasure from normal activities and increasing the urge to seek a “hit.”
- The HPA Axis: This is your body’s stress response system. Both addiction and sleep loss keep the HPA axis in overdrive, flooding your body with cortisol (the stress hormone).
- GABRA2: Variations in this gene can predict drinking behavior and are linked to how the brain processes relaxation and sleep.
- Circadian Rhythms: Our “body clock” is often completely shattered by active addiction. Restoring this rhythm is essential for the brain to know when to be alert and when to rest.
How Different Substances Disrupt Rest
Different substances leave different “scars” on your sleep architecture. Understanding what your specific “drug of choice” did to your brain can help us tailor your addiction recovery sleep plan.

Alcohol and Sleep Fragmentation
While many people use alcohol as a “nightcap,” it is actually one of the worst things for sleep.
- REM Suppression: Alcohol prevents you from entering deep REM sleep in the first half of the night. When it wears off, you experience “REM rebound,” leading to vivid nightmares and frequent wakefulness.
- Sleep Apnea: Alcohol relaxes the throat muscles, significantly increasing the risk of obstructive sleep apnea.
- Statistics: Between 36% and 91% of people with AUD suffer from insomnia. Even after a year of sobriety, many still report fragmented sleep.
Opioids and Breathing Disruptions
Opioids, including prescription pain relievers and heroin, have a profound impact on the brain’s respiratory center.
- Central Sleep Apnea: Unlike obstructive apnea, the brain simply “forgets” to signal the body to breathe during sleep when opioids are present.
- Opiate Detox: During withdrawal, the Locus Coeruleus (the brain’s alarm system) becomes hyperactive, making it nearly impossible to fall asleep.
- MAT Impact: While life-saving, medications like methadone or buprenorphine can sometimes contribute to sleepiness or disrupted sleep. At National Addiction Specialists, we work with patients in Tennessee and Virginia to optimize their Suboxone treatment timing to minimize these disruptions.
Stimulants and Cocaine Withdrawal
Stimulants like cocaine and methamphetamines keep the brain in a state of hyper-arousal.
- The “Crash”: Initial withdrawal often involves hypersomnia (sleeping too much), but this is not restorative sleep.
- Protracted Insomnia: After the crash, many experience months of inability to stay asleep.
- Cocaine Dreams: Three-quarters of people withdrawing from cocaine report poor sleep quality and distressing “using” dreams that can trigger cravings.
Overcoming Insomnia: Effective Strategies
If you’re struggling with addiction recovery sleep, don’t lose hope. Sleep is a skill that can be relearned.
Establishing a Consistent Sleep Schedule
Your brain loves routine. To fix your circadian rhythm:
- The 15-Minute Rule: Go to bed and wake up at the same time every day, even on weekends. Don’t vary this by more than 15 minutes.
- Limit Naps: If you must nap, keep it under 20 minutes and before 3:00 PM.
- Light Exposure: Get bright sunlight in your eyes within 30 minutes of waking up. This “sets” your internal clock for the day.
Creating a Restful Sleep Environment
Your bedroom should be a sanctuary for sleep and intimacy only.
- Temperature: Keep it cool (around 65°F or 18°C).
- Darkness: Use blackout curtains or an eye mask. Humans are incredibly sensitive to light; even a small LED from a charger can disrupt melatonin production.
- Blue Light: Electronic screens emit blue light that tells your brain it’s daytime. Turn off phones and TVs at least two hours before bed.
Holistic and Clinical Approaches to Better Sleep
Sometimes, sleep hygiene isn’t enough. We may need to dig deeper into holistic and clinical tools.
Relaxation Techniques for Recovery
- Deep Breathing: The 4-7-8 technique (breathe in for 4, hold for 7, exhale for 8) can physically calm your nervous system.
- Progressive Muscle Relaxation: Tensing and releasing each muscle group helps the body let go of the day’s stress.
- Warm Baths: Taking a warm bath or shower 1 to 1.5 hours before bed causes your core temperature to drop afterward, which is a natural signal for the body to sleep.
- Mindfulness: Meditation helps you observe “using” dreams or racing thoughts without reacting to them, reducing the anxiety that keeps you awake.
Clinical Treatment Options
At National Addiction Specialists, we believe in a comprehensive approach to addiction recovery sleep.
- Screening: We look for underlying issues like depression, anxiety, or sleep apnea that might be masquerading as “just” recovery insomnia.
- Non-Pharmacological: We prioritize Cognitive Behavioral Therapy for Insomnia (CBT-I), which is the gold standard for long-term results.
- Medication Management: If medication is needed, we focus on non-addictive options like melatonin, magnesium, or specific antidepressants that aid sleep without the risk of a new dependency. We avoid benzodiazepines, which carry high abuse potential and can lead to respiratory depression, especially in those on MOUD.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
https://www.nationaladdictionspecialists.com/new-patient-packet/
Frequently Asked Questions about Addiction Recovery Sleep
What are common triggers for sleep disturbances in recovery?
Stress is the primary trigger, but others include excessive caffeine (especially after noon), irregular schedules, and emotional instability. Environmental factors like a noisy neighborhood or an uncomfortable mattress also play a role. For those on MOUD, the timing of your medication can sometimes be a trigger; some find buprenorphine energizing, while others find it sedating.
How can healthcare providers screen for sleep problems?
We use tools like the Insomnia Severity Index (ISI) and sleep diaries to track your patterns over several weeks. In some cases, we may refer you for a formal sleep study (polysomnography) to rule out conditions like sleep apnea or restless leg syndrome.
How can loved ones support a recovering individual’s sleep?
The best thing you can do is help maintain a low-stress environment in the evening. Avoid bringing up heavy topics or “house meetings” right before bed. Encourage their routine without being “the sleep police”—pressure to sleep often makes insomnia worse!
Conclusion
Prioritizing addiction recovery sleep isn’t just about feeling less tired; it’s about giving your brain the best possible chance to stay sober. By establishing a routine, optimizing your environment, and seeking professional help when needed, you can turn sleep into your greatest “secret weapon” for long-term well-being.
If you are in Tennessee or Virginia and struggling with the intersection of addiction and sleep, National Addiction Specialists is here to help. Our telemedicine-based care is convenient, confidential, and led by experts who understand the unique challenges of the recovery journey.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.





