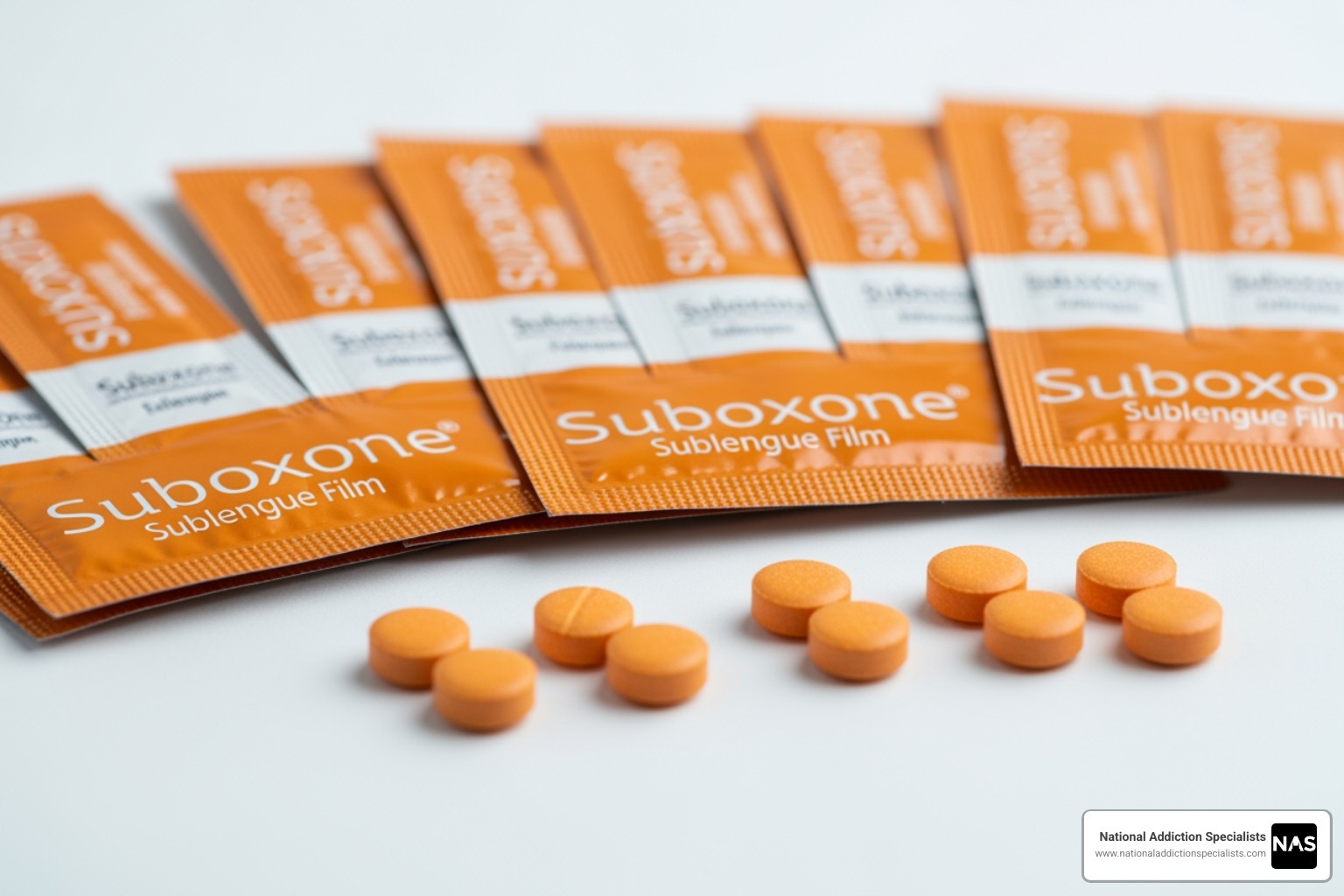
Why Opioid Dependence Treatment Can Change Your Life
Opioid dependence treatment offers proven pathways to recovery through FDA-approved medications, counseling, and support systems that help individuals regain control of their lives. With approximately 60 million people globally engaging in non-medical opioid use and roughly 450,000 deaths annually attributed to opioids, effective treatment has never been more critical.
Quick Answer: What Are My Treatment Options?
-
Medication-Assisted Treatment (MAT)
- Methadone (full opioid agonist)
- Buprenorphine/Suboxone (partial agonist)
- Naltrexone (opioid antagonist)
-
Counseling & Therapy
- Cognitive-Behavioral Therapy (CBT)
- Individual and group sessions
- Family counseling
-
Support Systems
- Peer support groups
- Recovery community resources
- Telemedicine options for convenient, private care
The opioid crisis has devastated families, with over 800,000 Americans lost to drug overdoses from 1999 to 2020. But here’s the crucial truth: recovery is possible.
Opioid Use Disorder (OUD) is a treatable medical condition, not a moral failing. It causes brain chemistry changes that make quitting incredibly difficult, even when you want to stop. The good news is that treatment works. Research shows medication-assisted treatment reduces overdose deaths by nearly 50% and supports long-term recovery. Help is available whether you’re struggling with prescription painkillers or illicit opioids like heroin or fentanyl.
Understanding the difference between physical dependence and addiction matters. Physical dependence means your body has adapted to regular opioid use and you’ll experience withdrawal symptoms if you stop suddenly. Addiction (OUD) goes further—it involves cravings, compulsive use, and continued use despite serious negative effects on your life, relationships, and health.
As a board-certified addiction medicine physician and founder of National Addiction Specialists, I’ve dedicated my career to providing evidence-based opioid dependence treatment. Through innovative telemedicine services, my work focuses on eliminating barriers to care, prioritizing privacy and accessibility to help people find lasting recovery.
This guide will walk you through everything you need to know about opioid dependence treatment—from understanding how different medications work to finding the right combination of therapy and support for your unique situation.
Terms related to Opioid dependence treatment:
Understanding Opioid Use Disorder (OUD)
Opioid Use Disorder (OUD) is a medical condition defined by a problematic pattern of opioid use that causes significant impairment or distress. It’s a complex brain disorder that changes how you think, feel, and behave.
It’s critical to understand that physical dependence and OUD are not the same. Physical dependence can happen to anyone taking opioids regularly, even as prescribed. It means your body has adapted and will experience withdrawal if you stop suddenly. OUD is more serious, characterized by compulsive drug-seeking and continued use despite harmful consequences. The drug hijacks your brain, controlling your decisions, relationships, and life.
What Causes OUD?
It’s not about being weak or making bad choices. Multiple factors work together to increase someone’s risk:
- Genetics: A family history of addiction can influence how your brain responds to opioids.
- Environment: Growing up around drug use, facing peer pressure, or having easy access to opioids all contribute.
- Trauma: People who’ve experienced physical or emotional trauma are more vulnerable, sometimes using opioids to numb emotional pain.
- Mental Health: Conditions like anxiety, depression, or PTSD increase the likelihood of self-medicating with opioids.
- Prescription Opioids: Many journeys with OUD begin with a prescription. Extended use can lead to tolerance, dependence, and eventually OUD.
The Brain Science Behind Opioid Dependence
Opioids attach to mu-opioid receptors in your brain, triggering a flood of dopamine that creates intense pleasure. Your brain remembers this powerful reward and wants more.
With repeated use, your brain adapts. Tolerance develops, meaning you need higher doses just to feel normal. When opioids leave your system, your brain goes into crisis mode, causing miserable withdrawal symptoms like muscle aches, nausea, anxiety, and overwhelming cravings. Many people continue using just to avoid this, creating a vicious cycle. These biological changes are why willpower alone isn’t enough; medical support is needed to restore balance.
Recognizing the Signs of OUD
Knowing the warning signs can save a life. If opioids are causing problems, opioid dependence treatment can help you reclaim control. Look for these red flags:
- Behavioral Signs: Using more opioids than intended, failed attempts to quit, spending excessive time getting or using opioids, and giving up important activities.
- Social Signs: Neglecting responsibilities at work or home, continuing use despite relationship problems, and withdrawing from family and friends.
- Physical Signs: Frequent drowsiness or “nodding off,” pinpoint pupils, changes in sleep or weight, poor hygiene, and experiencing flu-like withdrawal symptoms when not using.
- Other Consequences: Developing intense cravings, using in risky situations like driving, and facing mounting financial or legal problems.
If you see these signs in yourself or a loved one, reaching out for professional support is the most important next step. At National Addiction Specialists, we provide confidential telemedicine-based treatment that meets you where you are.
A Comprehensive Guide to Opioid Dependence Treatment Medications
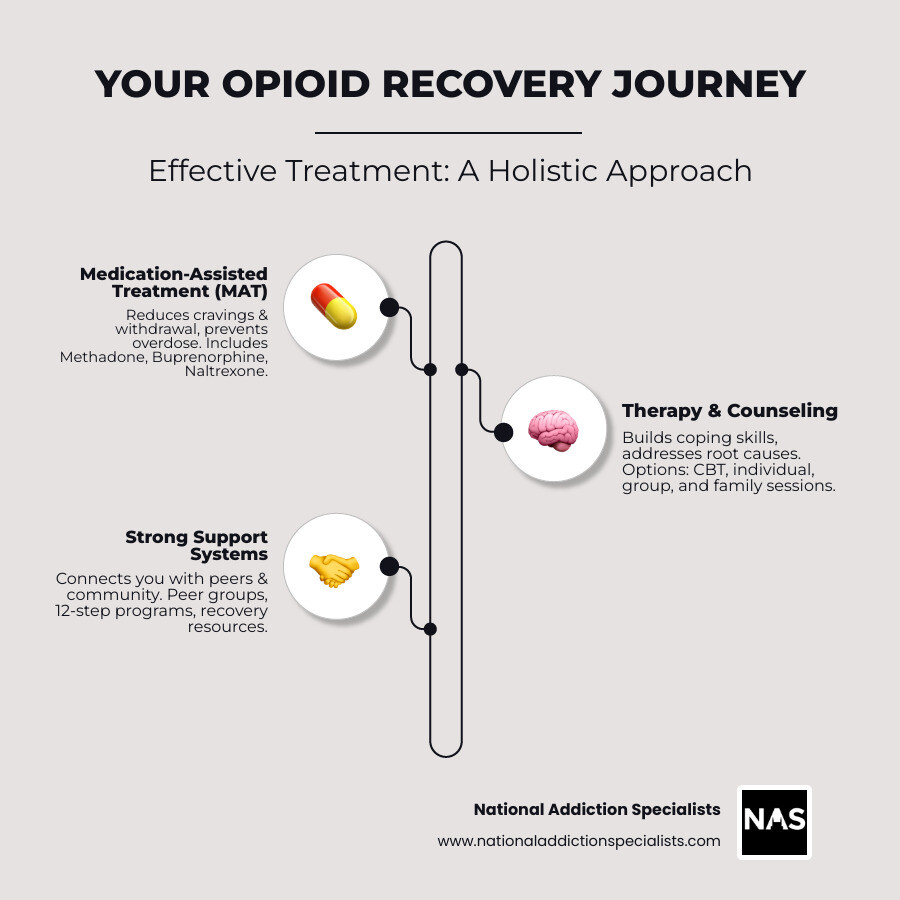
When it comes to opioid dependence treatment, medications are often essential. They help quiet the storm in your brain so you can focus on healing. This approach, called Medication-Assisted Treatment (MAT), combines FDA-approved medications with behavioral therapies to address the physical changes OUD has caused.
MAT medications work by reducing cravings, easing withdrawal symptoms, and preventing overdose. Some even block the euphoric effects of other opioids, removing the incentive for use. The FDA has approved three main medications for OUD: methadone, buprenorphine, and naltrexone.
Full Agonists: How Methadone Works
Methadone is a full opioid agonist that activates opioid receptors slowly and steadily. When taken as prescribed, it prevents withdrawal and reduces cravings without causing a high. Methadone maintenance treatment (MMT) is highly effective at reducing illicit drug use and keeping people in treatment. However, it has drawbacks. As a Schedule II drug, it typically requires daily visits to a certified clinic, which can be a major barrier. It also carries a risk of overdose if misused and can cause cardiac issues, requiring careful monitoring.
Partial Agonists: The Role of Buprenorphine
Buprenorphine is a partial opioid agonist, meaning it activates the same receptors but less intensely. This creates a “ceiling effect”—after a certain point, taking more doesn’t increase the opioid effects, making the risk of fatal overdose much lower. This safety profile is a major advantage.
One of buprenorphine’s biggest benefits is accessibility. The elimination of a special prescriber waiver in 2023 means it can be prescribed in primary care offices and through telemedicine—which is what we offer at National Addiction Specialists to patients in Tennessee and Virginia.
Buprenorphine is often combined with naloxone in a product called Suboxone. The naloxone is a safety feature: it’s not absorbed when taken as directed but will cause immediate, severe withdrawal if the medication is injected, deterring misuse. Subutex contains only buprenorphine.
Here’s a quick comparison of methadone and buprenorphine:
- Safety: Buprenorphine is safer due to its ceiling effect; methadone has a higher overdose risk.
- Accessibility: Buprenorphine is available from many doctors and via telemedicine; methadone requires daily clinic visits.
- Efficacy: Both are highly effective, though methadone may be preferred for severe OUD.
- Induction: Methadone can be started immediately; buprenorphine requires you to be in mild withdrawal first.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Antagonists: Naltrexone for Relapse Prevention
Naltrexone is an opioid antagonist that blocks opioid receptors, preventing any opioid from producing a high. It has no abuse potential and you cannot overdose on it, making it an excellent choice for relapse prevention in highly motivated individuals.
However, naltrexone presents challenges. You must be completely opioid-free for 7-10 days before starting, a difficult period to endure. Adherence to the daily oral pill can be low, though long-acting injections (Vivitrol) help. Most importantly, if you stop naltrexone and relapse, your tolerance is lower, creating a significantly increased risk of fatal overdose.
Managing Withdrawal: The Role of Alpha-2-Adrenergic Agonists
For those focused on getting through detoxification, non-opioid medications like clonidine and lofexidine can help. These alpha-2-adrenergic agonists calm the overactive nervous system response that causes the miserable physical symptoms of withdrawal (sweating, chills, anxiety). They are not a treatment for OUD itself but are valuable tools for making the initial phase of recovery more manageable.
The Holistic Approach: Integrating Therapy and Support Systems
Medication alone isn’t enough. True opioid dependence treatment addresses the whole person—the emotional wounds, broken relationships, and lost sense of purpose that often accompany addiction.
Medication stabilizes your brain, but recovery means rebuilding your life. Therapy and support systems provide the tools to do so. This whole-person approach focuses on building coping skills, addressing root causes like trauma, restoring relationships, and developing a meaningful life in recovery.
The Role of Counseling in Opioid Dependence Treatment
Counseling provides practical tools to change the patterns that fuel addiction.
- Cognitive-Behavioral Therapy (CBT) helps you identify and challenge the negative thoughts that drive drug use.
- Contingency Management uses positive reinforcement, like small rewards, to encourage recovery behaviors.
- Motivational Interviewing helps you explore your own reasons for change without judgment.
Therapy can be done in individual sessions for personalized attention, group therapy to connect with peers, or family counseling to heal relationships and build a supportive home environment.
Different Settings for Opioid Dependence Treatment
The right setting depends on your needs. Outpatient programs allow you to live at home while attending treatment, which works well for those with a stable environment. Inpatient or residential treatment offers 24/7 structured support for those needing a higher level of care.
Telemedicine options have revolutionized access to care. At National Addiction Specialists, we provide complete Suboxone treatment through secure video appointments. The benefits are substantial:
- Privacy: Receive care in the comfort of your own home, reducing stigma.
- Convenience: Save time and money by eliminating travel.
- Accessibility: Overcome barriers like distance from a clinic or difficult work schedules.
Studies show telehealth for buprenorphine treatment is as effective, or even more so, than in-person care.
The Power of Psychosocial Support
Community makes a huge difference in long-term recovery.
- Peer support groups like Narcotics Anonymous (NA) and other 12-step programs provide a safe space with people who truly understand your journey.
- Community resources like recovery housing or vocational training can help you rebuild the practical foundations of your life.
- A sober support network of friends, family, and peers provides accountability and encouragement, reducing the isolation that can threaten recovery. You don’t have to do this alone.
Key Considerations and the Future of OUD Treatment
Effective opioid dependence treatment has a profound impact that extends beyond the individual to benefit entire communities.
- Reducing Overdose Deaths: Medication-Assisted Treatment (MAT) is proven to reduce overdose mortality by nearly 50%, saving thousands of lives.
- Decreasing Disease Transmission: By reducing injection drug use, treatment helps curb the spread of bloodborne diseases like HIV and Hepatitis C.
- Reducing Stigma: Treating OUD as a chronic medical condition, like diabetes or hypertension, helps reduce the harmful stigma that prevents people from seeking help.
Choosing the Right Opioid Dependence Treatment Plan
Selecting the right plan is a highly personal process based on shared decision-making between you and your provider. Key factors include:
- Individual Needs: Treatment must be custom to your unique circumstances, history, and goals.
- Co-occurring Disorders: Many people with OUD also have mental health conditions that must be treated simultaneously.
- Lifestyle Factors: Work, family, housing, and transportation all influence which treatment approach is most sustainable.
- Patient Preference: You should be informed about all options (buprenorphine, methadone, naltrexone) and have a voice in your care.
Treating Special Populations
Certain groups require custom approaches in opioid dependence treatment:
- Pregnant Women: Opioid agonist therapy (buprenorphine or methadone) is the standard of care, improving health outcomes for both mother and baby.
- Adolescents: Treatment must account for developmental stages and family involvement. Extended MAT has shown promising results in this growing population.
- Individuals in the Criminal Justice System: Ensuring continuity of care from incarceration to release is critical for reducing overdose risk and supporting long-term recovery.
Latest Developments in OUD Pharmacotherapy
The field of opioid dependence treatment is continuously evolving, with exciting developments on the horizon:
- New Formulations: Long-acting injectables of buprenorphine (e.g., Sublocade, Brixadi) improve convenience and adherence by replacing daily dosing with monthly injections.
- Novel Medications: Researchers are exploring new compounds that target different brain systems to manage cravings and withdrawal.
- Immunotherapy: An emerging area of research involves therapeutic vaccines that could prevent opioids from reaching the brain, offering a new way to block their effects.
Conclusion
If you’ve made it this far, you’ve already taken an important step—seeking information, understanding your options, and considering a path forward. That takes courage.
Opioid dependence treatment works. We’ve walked through the science, the medications, the therapies, and the support systems that form the foundation of effective recovery. The evidence is clear: when medication, counseling, and psychosocial support work together, people heal. Lives are rebuilt. Families reconnect. Hope returns.
Recovery isn’t a straight line. Some days will feel easier than others. But here’s what matters most: you don’t have to face this alone. Whether you’re struggling with prescription painkillers, heroin, or fentanyl, effective, compassionate care is available right now.
At National Addiction Specialists, we understand that walking into a clinic can feel overwhelming or even impossible. That’s why we’ve built our practice around telemedicine-based Suboxone treatment for patients in Tennessee and Virginia. You can receive expert, personalized care from the privacy and comfort of your own home. No judgment. No unnecessary barriers. Just effective treatment delivered with respect and understanding.
We know that every person’s journey is different. Your treatment plan should reflect your unique needs, your life circumstances, and your goals. Whether you’re a parent trying to be there for your kids, a young adult just starting out, or someone who’s tried to quit before and faced setbacks—we’re here to help you find the right combination of medication, therapy, and support that works for you.
The opioid crisis has taken too many lives. But it doesn’t have to take yours. The path to recovery starts with a single decision: to reach out for help. We’ve seen it happen countless times—people who felt hopeless, who thought they’d never break free, who are now living full, meaningful lives in recovery.
Don’t wait another day. Your future self will thank you for taking this step.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.