Why Understanding Opioid Recovery Statistics Matters
Opioid addiction recovery rates reveal both sobering realities and reasons for hope. While recovery is challenging, millions of Americans have successfully overcome opioid use disorder.
Quick Facts About Opioid Recovery Rates:
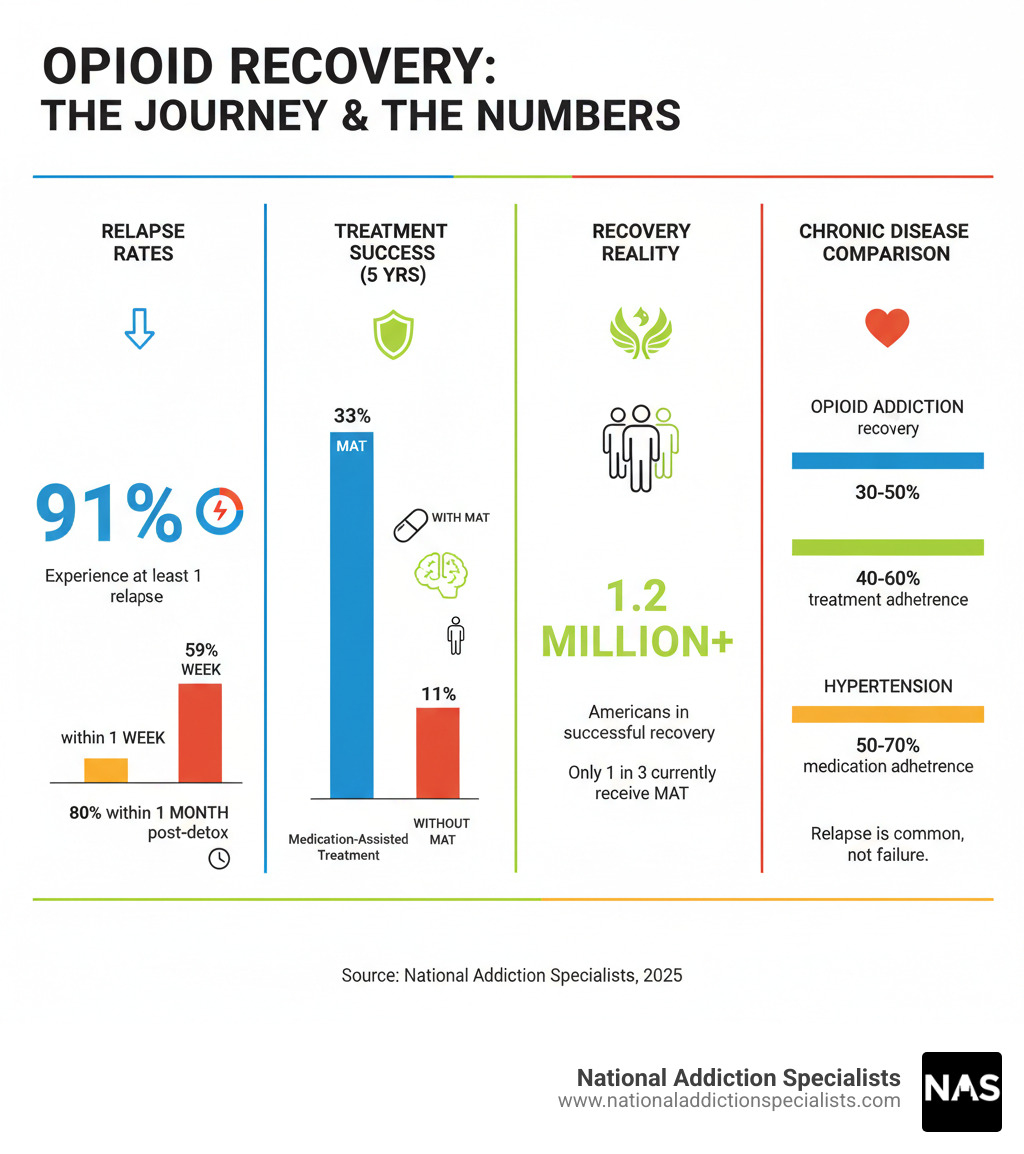
- 91% of people in opioid recovery experience at least one relapse.
- 59% relapse within the first week of sobriety.
- 80% relapse within one month after leaving detox.
- 1.2 million American adults have successfully recovered from opioid problems.
- 33% of people in MAT programs remain abstinent from heroin after 5 years.
- Only 11% of people with opioid addiction currently receive medication-assisted treatment.
Behind these statistics lies an important truth: recovery is possible. Understanding these numbers can help guide your path to lasting sobriety. Opioid addiction is a chronic condition, similar to diabetes or hypertension, requiring ongoing management. Relapse doesn’t mean failure; it means your treatment plan may need adjustment.
As a board-certified addiction medicine physician, I’ve seen that while statistics can seem daunting, personalized care and medication-assisted treatment significantly improve your chances of long-term recovery.
Opioid addiction recovery rates terms to learn:
Understanding Opioid Addiction Recovery Rates: A Sobering Look at the Data
Recovery from opioid use disorder is a process of managing a chronic condition, not a one-time fix. Opioid addiction recovery rates tell a story of both challenge and hope, helping us understand addiction as a brain disease that changes how we think and feel.
Repeated opioid use rewires the brain’s reward system. This is a biological change, not a character flaw. The good news is that brains can heal with time and support. The science of addiction and recovery shows that this process is real and recovery is possible.
What Are the Overall Opioid Addiction Recovery Rates?
The numbers show the challenges, especially in early recovery.
- 91% of people recovering from opioid addiction experience at least one relapse.
- The risk is highest early on: 59% of relapses occur within the first week, and 80% within the first month.
These statistics highlight the need for a strong support plan from day one. But there is hope: an estimated 1.2 million American adults have successfully recovered from opioid problems.
The right treatment makes a huge difference. For example, about 33% of people in MAT programs remain abstinent from heroin after five years. Unfortunately, only 11% of people with opioid addiction currently receive this effective treatment.
How Do These Rates Compare to Other Chronic Illnesses?
It’s helpful to compare opioid addiction to other chronic conditions. Relapse rates for addiction (40-60%) are similar to those for high blood pressure (50-70%) and diabetes (30-50%).

This comparison shows that addiction is a medical condition that responds to medical treatment. Like other chronic diseases, it requires ongoing management and adjustments to the treatment plan. A relapse is not a personal failure, but a sign that the treatment approach needs to be strengthened.
Key Factors Influencing Relapse and Recovery
Recovery from opioid addiction is shaped by a complex web of factors. Understanding what influences opioid addiction recovery rates can help you and your loved ones steer the journey with more confidence. Recognizing these factors gives you the power to make positive changes.
Common Warning Signs and Triggers for Opioid Relapse
Relapse is often a gradual process with clear warning signs. Recognizing them is key to preventing a setback. Common triggers include:
- Stress: Job loss, relationship problems, or financial strain can trigger the urge to use.
- Social isolation: Pulling away from support systems like family, friends, and recovery groups.
- Old patterns: Falling back into negative self-talk or dishonest behaviors.
- Negative emotions: Unmanaged anger, sadness, anxiety, or boredom can feel overwhelming.
- Environmental cues: People, places, and things associated with past drug use can spark intense cravings.
- Untreated mental health issues: Co-occurring depression, anxiety, or trauma significantly increase relapse risk.
Learning to spot these signs early and having a plan is crucial. For practical strategies, see our Tips to Prevent Addiction Relapse.
The Role of Psychosocial Factors and Mental Health
Addiction rarely exists in a vacuum. Mental health, social support, and life circumstances all play a major role in recovery.
Co-occurring mental health disorders are very common; 55.8% of people with a substance use disorder also have a mental illness. These conditions often fuel each other, so treating both is essential for lasting recovery.
Social support from family, friends, and peers acts as a protective shield. In contrast, isolation makes recovery much harder.
Recovery capital refers to the total resources—personal, social, and community—that support your recovery. This includes coping skills, supportive relationships, safe housing, and employment. While people with OUD often start with lower recovery capital, it can be rebuilt over time.
Improving quality of life is a key goal. Stable housing, meaningful work, and healthy relationships make recovery more sustainable. Statistics show that 88.4% of people in recovery rate their quality of life as good or better.

Positive psychosocial factors that support recovery:
- Stable housing and safe living environment
- Meaningful employment or educational pursuits
- Strong family relationships and friendships
- Active participation in recovery communities
- Access to healthcare and mental health services
- Engaging hobbies and interests
- Spiritual or religious connections
- Financial stability and management skills
Our approach at National Addiction Specialists combines MAT with mental health support to address these interconnected factors, helping you build a foundation for recovery from home.
Evidence-Based Strategies for Preventing Relapse
Powerful, scientifically-proven tools can dramatically improve opioid addiction recovery rates. A comprehensive approach that addresses the issue from multiple angles is key to building lasting sobriety.
How Medication-Assisted Treatment (MAT) Improves Success
Medication-Assisted Treatment (MAT) is the gold standard for opioid use disorder. It combines FDA-approved medications like buprenorphine (in Suboxone) with counseling and therapy. These medications work by:
- Reducing intense cravings
- Managing withdrawal symptoms
- Blocking the euphoric effects of opioids
The impact is remarkable: studies show about 33% of people in MAT programs remained abstinent from heroin after five years. Yet, only about 11% of people with opioid addiction currently receive MAT, often due to barriers like stigma and lack of access.
Our telemedicine approach makes Medication-Assisted Treatment for Opioid Addiction accessible from home. We accept Medicaid and Medicare in Tennessee and Virginia to ensure everyone can access this life-saving treatment.
The Impact of Treatment Duration and Aftercare
Lasting recovery takes time. Research shows that longer treatment durations lead to better outcomes, with the National Institute on Drug Abuse recommending at least 90 days of treatment for meaningful results.

Formal treatment is just the beginning. Aftercare is the crucial bridge to independent sober living. Key components include:
- Continuing Care: Regular therapy sessions to process challenges.
- Support Groups: Peer-led groups like Narcotics Anonymous or SMART Recovery offer connection and understanding.
- Sober Living Environments: These provide structure, with 68% of residents remaining abstinent for at least 12 months.
- Ongoing Therapy: Approaches like CBT help you manage stress and triggers.
- Physical Health: Proper nutrition is a powerful, often overlooked, part of aftercare. Learn more about The Importance of Nutrition in Addiction Recovery.
Our telemedicine platform makes ongoing support convenient, offering personalized Addiction Recovery Strategies for your journey.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
What to Do After an Opioid Relapse
Relapse can be a part of recovery, but it is not a failure. It doesn’t erase your progress or mean recovery is out of reach. A relapse is a sign that your recovery plan needs adjustment.
Crucially, your overdose risk is much higher after a period of abstinence because your tolerance has dropped. Taking immediate, safety-focused action is vital.
Immediate Steps to Take for Safety and Support
If a relapse occurs, your safety is the top priority. Take these steps immediately:
- Stop using. Your tolerance is lower, and continued use is extremely dangerous.
- Tell someone you trust. Reach out to a family member, friend, sponsor, or treatment provider. Isolation is the enemy of recovery. Our guide on How to Support Someone in Recovery can help loved ones.
- Get rid of any substances. Remove the temptation to use more.
- Do not isolate. Fight the urge to hide in shame. Connect with your support network.
- Seek emergency medical help if you have signs of overdose or severe withdrawal.
- Analyze what happened. Without self-blame, try to understand the triggers that led to the relapse to build a stronger defense.
Re-engaging with Treatment and Strengthening Your Plan
A relapse is a signal that your safety system needs attention. It’s time to re-engage with your treatment and strengthen your plan.
Contact your treatment provider immediately. We are here to help you get back on track without judgment. Your treatment plan may need adjustments, such as re-evaluating your Suboxone dose or increasing counseling frequency. Our Suboxone Treatment Programs are flexible for this reason.
Use this as an opportunity to strengthen your coping skills and refresh your relapse prevention plan. Identify missed warning signs and areas where your support system can be improved. A relapse is a learning experience that can make your recovery stronger in the long run.
Long-Term Recovery: What Does Success Look Like?
Success in recovery is about more than just abstinence; it’s about rebuilding a fulfilling, healthy, and meaningful life. This holistic journey toward well-being is often called an Addiction Recovery Journey.
Long-Term Opioid Addiction Recovery Rates and Outcomes
The long-term outlook for opioid addiction recovery rates offers genuine hope. Studies following individuals for 10+ years show that approximately 30% achieve abstinence from opioids. After five years of continuous remission, the risk of relapse drops to less than 15%.
However, the stakes are high. The mortality risk for people with OUD is at least 6 times greater than the general population, making effective treatment life-saving. You can read more in this Long-term course of opioid addiction research.
Long-term recovery brings dramatic improvements in quality of life, including better psychological well-being, stable employment, financial security, and flourishing relationships.
Overcoming Barriers to Effective Treatment
Despite proven treatments, significant barriers still impact opioid addiction recovery rates and prevent people from getting care. Key challenges include:
- Access to Treatment: Geographic limitations, especially in rural areas, make it hard to find qualified providers.
- Stigma Against MAT: Misconceptions prevent many from seeking this gold-standard treatment. Only about 11% of people with OUD receive MAT.
- Provider Shortages & Cost: A lack of trained professionals and issues with insurance coverage create further obstacles.
At National Addiction Specialists, we work to tear down these barriers. Our telemedicine Suboxone treatment brings expert care to your home in Tennessee and Virginia. By accepting Medicaid and Medicare, we make treatment more accessible. For other options, use SAMHSA’s Behavioral Services Locator.
Frequently Asked Questions about Opioid Recovery
Navigating opioid recovery can be confusing. Here are answers to some of the most common questions.
Is recovery from opioid addiction really possible?
Yes, absolutely. While opioid addiction recovery rates show the challenges, an estimated 1.2 million U.S. adults have resolved an opioid problem. These are real people who have rebuilt their lives. With proper treatment, strong support, and time, recovery is not just possible—it’s probable.
Why are opioid relapse rates so high?
Opioids fundamentally change brain chemistry, rewiring the areas responsible for pleasure, memory, and decision-making. This biological change leads to intense cravings and deep psychological dependence, where opioids become the primary coping mechanism. Everyday triggers—people, places, or emotions—can activate these altered brain pathways. Furthermore, tolerance drops during sobriety, making overdose a significant risk if a relapse occurs.
Does a relapse mean treatment failed?
No. Relapse does not equal failure. Addiction is a chronic condition, and relapse is a sign that the treatment plan needs adjustment, much like with diabetes or asthma. A relapse provides valuable information about triggers and coping strategies that need strengthening. The key is to respond by re-engaging with treatment quickly, being honest about what happened, and using the experience to build a more resilient recovery plan.
Conclusion: Your Path to Lasting Recovery Starts Here
The statistics on opioid addiction recovery rates tell a story of both challenge and profound hope. While early relapse rates are high, the most important statistic is that 1.2 million American adults are living proof that recovery is possible.
Evidence clearly shows that medication-assisted treatment (MAT) significantly improves outcomes, with 33% of people in MAT programs remaining abstinent from heroin after five years. This is the power of evidence-based care.
At National Addiction Specialists, we witness these changes daily. Our telemedicine platform breaks down barriers, providing convenient, confidential Suboxone treatment and counseling to help individuals reclaim their lives. We serve patients in Tennessee and Virginia, accepting Medicaid and Medicare to ensure financial constraints don’t stand in the way of recovery.
Seeking help is a sign of strength. Your story doesn’t end with addiction—it begins with recovery.
Take the first step with our convenient telemedicine treatment.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








