Why Help for Opioid Addiction Matters Now More Than Ever
Help for opioid addiction is available, evidence-based, and can save your life. With millions struggling with opioid use disorder, it’s crucial to know that effective help is within reach.
Quick Help Resources:
- Call SAMHSA’s National Helpline: 1-800-662-HELP (4357) – free, confidential, 24/7
- Find treatment near you: FindTreatment.gov
- Emergency overdose: Call 911 and administer naloxone if available
- Crisis support: Call or text 988 for the Suicide & Crisis Lifeline
Effective Treatment Options:
- Medication-Assisted Treatment (MAT) – FDA-approved medications like methadone, buprenorphine (Suboxone), or naltrexone
- Counseling and behavioral therapy – addressing root causes and building coping skills
- Telehealth services – convenient, private treatment from home
- Support groups – peer support and community connection
Recovery is not just possible – it’s happening every day for people just like you.
Opioid addiction is a chronic medical condition that changes the brain, making it hard to stop using alone. Treatment works. Research shows that medication-assisted treatment (MAT) combined with counseling reduces overdose deaths and helps people reclaim their lives.
The stigma around addiction prevents many from seeking help. Fewer than 1 in 5 people with opioid use disorder receive the medication that could save them. This needs to change.
You don’t have to face this alone. Whether you’re struggling yourself or worried about someone you love, understanding your options is the first step toward recovery.
I’m Dr. Chad Elkin, founder of National Addiction Specialists. I’ve dedicated my career to providing accessible help for opioid addiction through evidence-based telemedicine, focusing on eliminating barriers to care.
This guide will explain opioid use disorder, cover effective treatments, and show you how to find help that fits your life.
![[object Object] [object Object]](https://images.bannerbear.com/direct/4mGpW3zwpg0ZK0AxQw/requests/000/117/141/299/9BvRDJ724zWPgwmg6lAKNOd03/ab4ad3bccdd908982fea4329c6183f8e09bdb7d4.jpg)
Common Help for opioid addiction vocab:
Understanding Opioid Use Disorder (OUD)
If you or someone you care about is struggling with opioids, understanding what’s actually happening in the body and brain can be incredibly helpful. Opioid use disorder (OUD) isn’t about being weak or making bad choices – it’s a chronic medical condition that changes how your brain works. And here’s the important part: it’s treatable.
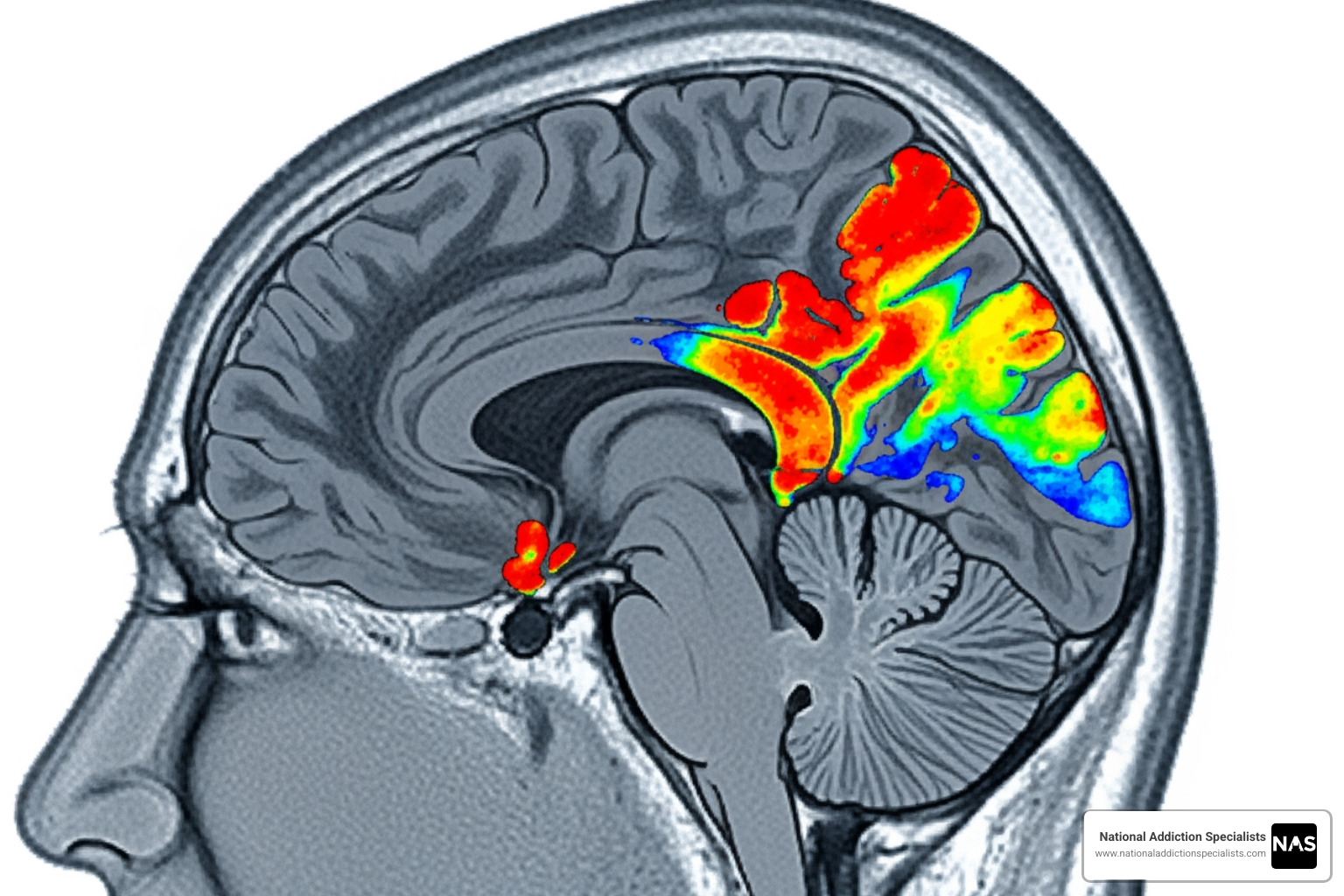
Millions of Americans experience OUD, characterized by compulsive opioid use despite harmful consequences. Your brain has been rewired in a way that makes stopping incredibly difficult without the right help for opioid addiction.
It’s important to distinguish physical dependence from addiction. Physical dependence can happen to anyone taking opioids regularly, even as prescribed. Your body adapts to the medication. Addiction, however, involves deeper brain changes affecting decision-making, impulse control, and pleasure. For more background, visit our page on Drug Addiction.
What is Opioid Use Disorder?
OUD is a medical condition defined by criteria in the DSM-5, such as using more opioids than intended, strong cravings, and failed attempts to quit. It’s not a label but a diagnosis for a treatable, chronic condition, similar to diabetes or heart disease. It’s caused by a mix of genetics, brain chemistry, and environment. The key takeaway is that OUD is a medical problem with medical solutions. Scientific research on DSM-5 criteria for substance use disorders offers more detail.
How Opioid Addiction Changes the Brain
Opioids attach to brain receptors, triggering a massive dopamine release that creates intense pleasure, far more powerful than natural rewards. Over time, your brain adapts in ways that make quitting on your own extremely difficult.
- The reward system gets hijacked. Your brain prioritizes opioids above all else, making normal activities less satisfying.
- Tolerance develops. You need more of the drug to feel the same effect—a biological adaptation.
- Physical dependence sets in. Your body can’t function normally without opioids, leading to miserable withdrawal symptoms when you stop. Learn more on our Opioid Withdrawal page.
- Decision-making becomes impaired. The brain’s prefrontal cortex is altered, making it harder to resist using despite knowing the consequences.
These are measurable brain changes, not character flaws. That’s why professional help for opioid addiction is medically necessary.
Common Signs and Symptoms of OUD
Recognizing OUD is the first step. Signs can be physical, behavioral, and emotional.
- Physical signs: Drowsiness, pinpoint pupils, nausea, constipation, slurred speech, weight loss, poor hygiene.
- Behavioral signs: Social isolation, secretiveness, neglecting responsibilities, financial issues, risky behavior, failed attempts to quit.
- Psychological signs: Intense cravings, mood swings, irritability, anxiety, depression, loss of interest in hobbies.
Withdrawal symptoms appear when use stops and can include severe flu-like symptoms, muscle cramps, nausea, and intense anxiety. These symptoms often drive a person back to using for relief.
If you see these signs, seeking help is a sign of strength. If you’re concerned about a loved one, approach them with compassion. For more details, visit our resource on Signs of Drug Addiction in Adults.
The good news? Effective help for opioid addiction exists, and you don’t have to face this alone.
Effective Treatment: Your Path to Recovery
Here’s the truth: opioid use disorder is treatable, and people recover every single day. The most effective help for opioid addiction combines medication with counseling and therapy—a comprehensive approach that addresses both your brain chemistry and the life circumstances that contribute to addiction.
Research from the National Institute of Drug Abuse consistently shows that this integrated approach dramatically lowers overdose deaths. Unfortunately, fewer than 1 in 5 people with OUD receive this gold-standard treatment due to stigma and access barriers, which we are working to change.
The Gold Standard: Medication-Assisted Treatment (MAT)
Medication-Assisted Treatment (MAT) combines FDA-approved medications with counseling. It’s not “trading one drug for another”; it’s a medical treatment that:
- Normalizes brain chemistry: Restores normal function so you can think clearly.
- Relieves cravings: Reduces the intense psychological drive to use opioids.
- Prevents withdrawal: Eliminates the severe physical discomfort of quitting.
At National Addiction Specialists, I’ve seen MAT help people rebuild their lives, careers, and relationships through our telemedicine services. You can learn more about our approach on our Medication Assisted Treatment Program page.
FDA-Approved Medications for OUD
Three FDA-approved medications form the backbone of MAT: methadone, buprenorphine, and naltrexone. The right one depends on your individual needs.
- Methadone: A full opioid agonist available only at certified clinics, often requiring daily visits. It blocks the effects of other opioids and normalizes body functions.
- Buprenorphine: A partial opioid agonist with a “ceiling effect,” making it safer. Often combined with naloxone (as Suboxone), it can be prescribed by qualified providers via telemedicine. At National Addiction Specialists, we make buprenorphine accessible across Tennessee and Virginia, eliminating daily clinic visits.
- Naltrexone: An opioid antagonist that blocks opioid receptors entirely. It comes as a pill or monthly injection (Vivitrol). You must be opioid-free for 7-10 days before starting to avoid severe withdrawal.
For more detailed information about buprenorphine treatment, visit our page on Suboxone for Opioid Addiction.
The Crucial Role of Counseling and Therapy
Medication stabilizes your brain, but counseling helps you rebuild your life. It’s just as important as medication for addressing the root causes of addiction, like trauma, anxiety, or chronic pain.

Effective therapies include:
- Cognitive Behavioral Therapy (CBT): Helps you identify and change negative thought patterns that lead to drug use.
- Motivational Interviewing: Strengthens your personal motivation and commitment to recovery.
Therapy provides practical coping skills for managing stress and cravings, helps repair relationships, and allows you to build a meaningful life beyond addiction. At National Addiction Specialists, we integrate counseling into our telemedicine MAT programs for the best outcomes. Learn more in our article on the Importance of Counseling and Therapy in Suboxone Treatment.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
How to Find Help for Opioid Addiction
Taking the step to find help for opioid addiction is a brave decision. It can feel overwhelming, but the good news is that effective, compassionate care is more accessible than you might think, especially with the rise of telemedicine.
For practical guidance on taking this crucial first step, our resource on the Best Ways to Ask for Help with Addiction offers valuable advice.
Finding Quality Treatment Programs and Providers
Finding a quality program that offers evidence-based care is key. Use these confidential resources:
- SAMHSA’s National Helpline: Call 1-800-662-HELP (4357) for free, 24/7 referrals.
- FindTreatment.gov: A federal site to locate nearby treatment facilities, including the Behavioral Health Treatment Services Locator.
- Buprenorphine and Methadone Locators: SAMHSA provides specific locators like the Buprenorphine Treatment Provider Locator and Treatment Center Locator, Including Methadone Centers.
When evaluating programs, look for individualized plans, a combination of medication and counseling, licensed providers, and a focus on long-term recovery. At National Addiction Specialists, our Online Suboxone Doctors provide this comprehensive care via telemedicine in Tennessee and Virginia.
Overcoming Barriers to Accessing Help for Opioid Addiction
Practical obstacles shouldn’t stop you from getting help for opioid addiction.
- Cost: Most insurance plans, including Medicaid and Medicare, cover addiction treatment. National Addiction Specialists accepts both, making care affordable in Tennessee and Virginia. The Mental Health and Addiction Insurance Help from HHS can clarify your rights.
- Location: Telemedicine eliminates geographic barriers. Our Telemedicine Treatment allows you to get care from home, saving time and travel costs.
- Stigma: OUD is a medical condition, not a moral failing. Treatment is confidential and protected by federal law (42 CFR Part 2). Telemedicine offers an extra layer of privacy, as you can receive care without visiting a clinic.
Emergency Resources and Overdose Prevention
Be prepared for emergencies. Naloxone (Narcan) is a life-saving medication that reverses an opioid overdose. It’s available without a prescription at most pharmacies in Tennessee and Virginia. Everyone with OUD and their loved ones should have it and know how to use it. The CDC has more information on Life-Saving Naloxone.
If you witness an overdose, call 911 immediately and give naloxone if you have it. Good Samaritan Laws in Tennessee and Virginia protect you from drug possession charges when you call for help.
Save these numbers:
- 988 Suicide & Crisis Lifeline: Call or text 988 for 24/7 support.
- SAMHSA’s National Helpline: 1-800-662-HELP (4357) for treatment referrals.
- Disaster Distress Helpline: 1-800-985-5990 for crisis counseling.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Navigating Long-Term Recovery and Wellness
Recovery from opioid use disorder is a lifelong journey toward wellness. With the right help for opioid addiction and ongoing support, long-term recovery is not just possible—it’s happening for thousands of people every day.

Recovery looks different for everyone. Building the right support system and understanding what to expect can make all the difference.
Building a Strong Support System
No one recovers in isolation. Building a strong support system is essential.
- Family and friends: Their encouragement is vital. Loved ones can find guidance on our page about How to Support Someone in Recovery.
- Peer support groups: Groups like Narcotics Anonymous (NA) and SMART Recovery connect you with people who understand your journey, providing accountability and shared experience.
- Professional support: Ongoing therapy helps maintain coping skills. National Addiction Specialists offers long-term support through telemedicine in Tennessee and Virginia.
Special Considerations for Getting Help for Opioid Addiction
Certain situations require specialized help for opioid addiction.
- Pregnancy and breastfeeding: Treating OUD during pregnancy is crucial for the health of both mother and baby. Medications like buprenorphine and methadone are considered safe and are the recommended standard of care. Breastfeeding is also generally safe while on these medications. The ACOG Committee Opinion on Opioid Use and Opioid Use Disorder in Pregnancy offers detailed guidance.
- Pain management: If you’re in recovery, managing pain requires a creative, non-opioid approach. Strategies may include physical therapy, nerve blocks, or non-opioid medications. Open communication with your healthcare team is essential to create a plan that supports your recovery.
What Long-Term Recovery Looks Like
Long-term recovery is about rebuilding your life. Success means more than just freedom from opioids; it’s about improved physical and mental health, stable work, and supportive relationships.
Relapse doesn’t mean failure. It’s a chance to learn and adjust your recovery plan. Our page on Tips to Prevent Addiction Relapse offers helpful strategies.
Continued care is key to maintaining recovery. This includes regular check-ups, counseling, and support groups. National Addiction Specialists provides ongoing telemedicine care in Tennessee and Virginia, accepting Medicaid and Medicare to ensure support is always accessible. Recovery is a journey—keep moving forward, one day at a time.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Conclusion
The most important truth is that help for opioid addiction exists, it works, and it can change your life. Recovery is not just possible—it’s happening every day.
Remember: You are not alone. Millions have walked this path, and caring professionals are ready to help.
At National Addiction Specialists, we believe everyone deserves access to quality care. We provide telemedicine-based Suboxone treatment and counseling throughout Tennessee and Virginia. Our model is convenient, confidential, and effective. We accept Medicaid and Medicare because cost should not be a barrier to recovery.
Taking the first step is the hardest part, but you don’t have to do it alone. Once you reach out, you’ll find support, strength, and proven treatments. Don’t let another day pass. Let us help you start your journey to a healthier life.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








