Navigating Suboxone Use During Pregnancy Without the Stress
Is Suboxone Safe During Pregnancy? What Every Expectant Mother Should Know
Suboxone in pregnancy is considered safe and is actually recommended by major clinical guidelines — including those from ACOG and SAMHSA — as part of a comprehensive treatment plan for Opioid Use Disorder (OUD).
Here is a quick summary of what the evidence shows:
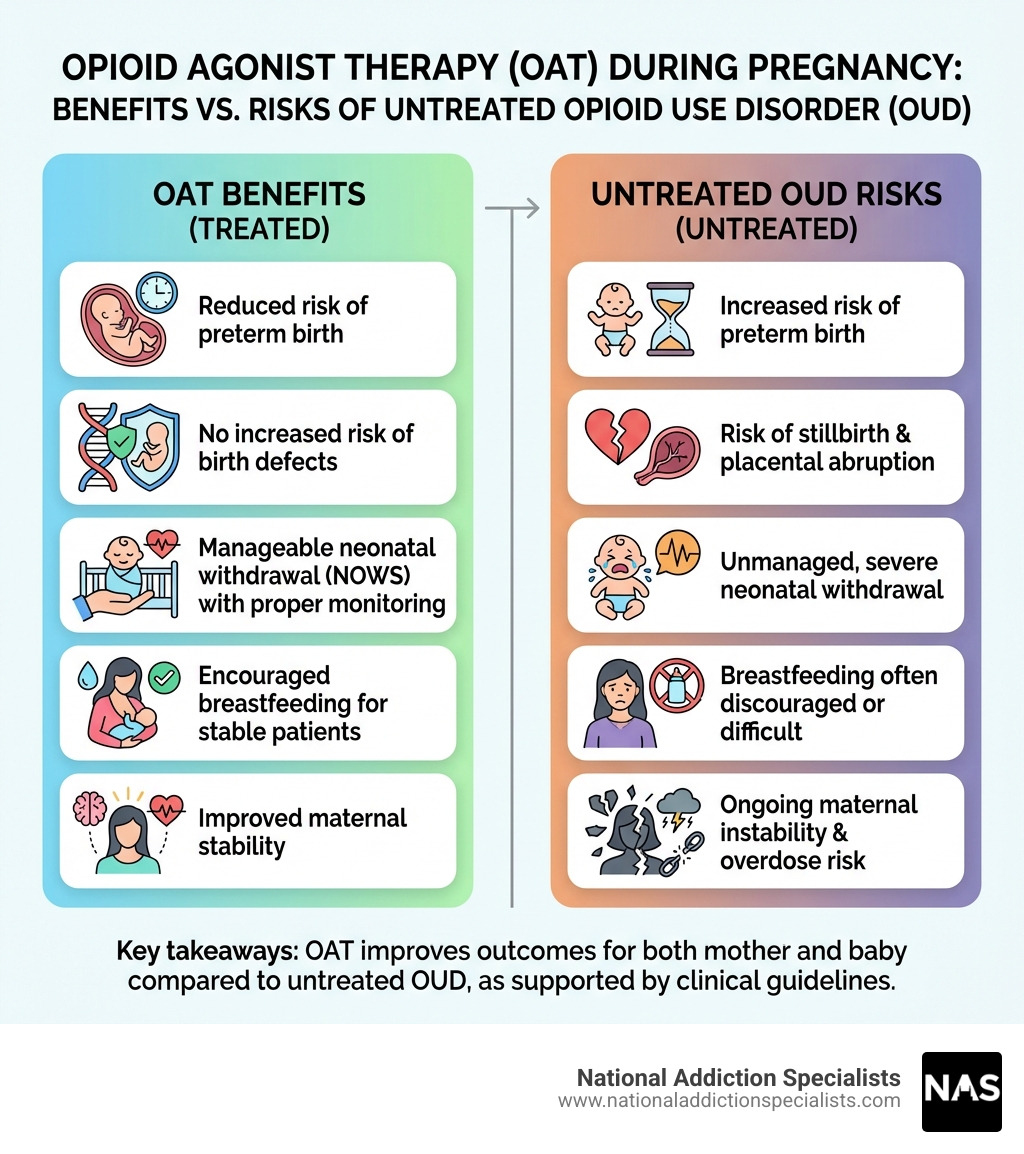
- Safe to use: Suboxone does not increase the risk of birth defects compared to the general population
- Better than no treatment: Untreated OUD carries far greater risks — including preterm birth, stillbirth, and placental abruption — than treated OUD
- NOWS is possible but manageable: Some babies may show signs of withdrawal after birth, but this is monitored and treatable
- Breastfeeding is generally encouraged: Levels of buprenorphine in breast milk are very low and unlikely to harm your baby
- Dose adjustments are normal: Your dose may need to increase during later pregnancy due to faster metabolism
If you are pregnant and managing opioid dependence, you are not alone — and you have real, effective options. Maternal opioid-related diagnoses in the United States more than doubled between 2010 and 2017, rising from 3.5 to 8.2 per 1,000 delivery hospitalizations. Yet many pregnant people still delay or avoid treatment because of fear, stigma, or confusion about what is actually safe for their baby.
The good news: the clinical picture has shifted significantly. What was once viewed with caution is now supported by a growing body of research showing that staying on Suboxone during pregnancy leads to better outcomes for both mother and child — far better than quitting opioids cold turkey or leaving OUD untreated.
This guide walks you through everything you need to know — from safety data and dosing to breastfeeding and postpartum care — so you can make informed decisions without unnecessary stress.
I’m Chad Elkin, MD, board-certified in Addiction Medicine and founder of National Addiction Specialists, where I have helped many patients navigate suboxone in pregnancy safely as part of individualized, evidence-based care. The guidance in this article reflects current clinical standards and my direct experience treating opioid use disorder across all stages of pregnancy and postpartum recovery.
Understanding Suboxone in Pregnancy: Safety and Guidelines
When we talk about suboxone in pregnancy, we are discussing a combination medication consisting of buprenorphine (a partial opioid agonist) and naloxone (an opioid antagonist). For years, the “gold standard” for pregnant women with Opioid Use Disorder was either methadone or buprenorphine monotherapy (often known by the brand name Subutex). However, clinical practice has evolved.
Current ACOG guidelines and SAMHSA clinical guidance now recognize that the buprenorphine-naloxone combination is a safe and effective option. At National Addiction Specialists, we focus on providing the most up-to-date, evidence-based care to ensure both you and your baby are protected.
To understand why this matters, it helps to know what is Suboxone and how it functions. Unlike full opioids (like heroin or oxycodone), buprenorphine has a “ceiling effect,” meaning it provides stability without the same high risk of respiratory depression or overdose.
The Shift from Monotherapy to Combination Treatment
In the past, doctors often switched pregnant patients from Suboxone to buprenorphine monotherapy because of theoretical concerns that the naloxone component might harm the fetus or cause withdrawal. We now know that when taken sublingually (under the tongue) as directed, very little naloxone enters the bloodstream.
Furthermore, suboxone-use-during-pregnancy is often preferred over monotherapy because the combination product is much less likely to be misused or diverted. This provides an extra layer of safety for the mother and the community. Even Health Canada recently updated its monographs to remove pregnancy as a contraindication for Suboxone, reflecting this modern understanding.
Clinical Evidence and Safety Standards
The data is reassuring. A systematic review of buprenorphine-naloxone safety involving hundreds of mother-infant pairs found no significant difference in birth outcomes, such as head circumference or birth weight, when compared to other treatments.
Crucially, the rate of congenital anomalies (birth defects) in babies exposed to suboxone in pregnancy ranges from 3.2% to 3.5%. This is statistically identical to the rate found in the general population. In other words, taking Suboxone does not increase the risk of physical abnormalities.
| Feature | Suboxone (Buprenorphine/Naloxone) | Buprenorphine Monotherapy |
|---|---|---|
| Safety in Pregnancy | Evidence-based & safe | Evidence-based & safe |
| Abuse Potential | Lower (due to naloxone) | Higher |
| Street Value | Lower | Higher |
| Clinical Preference | Increasing standard of care | Historically used, now less necessary |
Maternal and Neonatal Outcomes: What to Expect
One of the biggest worries for expectant mothers is how their treatment will affect their newborn. While it is true that some babies will experience Neonatal Opioid Withdrawal Syndrome (NOWS), also called Neonatal Abstinence Syndrome (NAS), the outcomes for babies whose mothers are on Suboxone are generally very positive.

Research shows that babies exposed to buprenorphine often have shorter hospital stays and require less medication to treat withdrawal symptoms than those exposed to methadone. Understanding how-does-suboxone-treatment-work helps clarify this; because it is a partial agonist, the physical dependence it creates in the infant is often less intense than full agonists.
Long-term Developmental Considerations
We are often asked about the “long-term” effects. While more research is always being conducted, programs like the CDC’s MAT-LINK surveillance network track children up to age six. So far, the data suggests that most children exposed to MOUD (Medications for Opioid Use Disorder) in utero meet their developmental milestones.
The benefits-of-suboxone-treatment extend far beyond the delivery room. By providing maternal stability, Suboxone reduces the risk of illicit drug use, which is often associated with poor nutrition, lack of prenatal care, and exposure to violence—all factors that have a much larger impact on a child’s long-term health than the medication itself.
Managing Your Treatment: Dosing and Breastfeeding
Your body undergoes massive changes during pregnancy, and your medication needs to keep up. It is perfectly normal—and often necessary—for your Suboxone dose to change as your pregnancy progresses.
Adjusting Doses for Fetal Growth
As you move into the third trimester, your blood volume increases, and your liver and kidneys process medication more quickly. Additionally, the placenta and the fetus itself begin to metabolize the buprenorphine.
Because of this, many women find they need a higher dose or “split dosing” (taking the medication twice or three times a day instead of once) to avoid suboxone-withdrawal symptoms. If you feel “washy” or start experiencing cravings late in your pregnancy, it isn’t a sign of “relapse”—it’s a sign that your body needs a dose adjustment to maintain a stable environment for your baby.
The Safety of Breastfeeding on Suboxone
We strongly encourage breastfeeding for our patients who are stable on Suboxone and not using illicit substances. The amount of buprenorphine that passes into breast milk is incredibly small—far too low to cause sedation or harm to the baby.
In fact, breastfeeding can actually help reduce the severity of NOWS symptoms in your newborn. The skin-to-skin contact and the tiny amounts of medication in the milk can help soothe the baby and make their transition easier. If you eventually decide to stop breastfeeding, we recommend doing so gradually to prevent the baby from experiencing any alcohol-addiction-during-pregnancy-risks-and-consequences or other withdrawal-like discomforts.
Best Practices for Postpartum Care and Recovery
The “fourth trimester”—the period immediately after birth—is a time of high vulnerability. At National Addiction Specialists, we emphasize that your recovery journey doesn’t end at delivery; it actually enters a critical new phase.
Pain Management During and After Labor
Many women fear that being on Suboxone means they cannot receive pain relief during labor. This is a myth. You can—and should—receive appropriate pain management.
Epidurals and local anesthetics work perfectly fine while you are on Suboxone. For post-delivery pain, especially after a C-section, we work with your obstetrician to use non-opioid options like NSAIDs or acetaminophen. If opioids are absolutely necessary for short-term acute pain, they can be used, but they must be carefully managed by your online-suboxone-doctors and your surgical team.
Support Systems and Harm Reduction
The risk of relapse is statistically highest in the postpartum period due to sleep deprivation, hormonal shifts, and the stress of a new baby. This is why continuing your suboxone-treatment-online is so important.
We also advocate for “rooming-in,” where the baby stays in the room with the mother rather than in the NICU. This has been shown to decrease the need for pharmacological treatment of NOWS and improves maternal-infant bonding.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. Make an Appointment
Frequently Asked Questions about Suboxone in Pregnancy
What are the benefits of Suboxone for the baby during pregnancy?
Using suboxone in pregnancy provides a stable intrauterine environment. It prevents the “cycle of withdrawal” that occurs with short-acting opioids like heroin, which can cause fetal distress or even miscarriage. Babies born to mothers on buprenorphine-based treatments often have higher birth weights and larger head circumferences than those exposed to untreated OUD or methadone. You can find suboxone-doctors-near-me-that-accept-medicaid through our Tennessee and Virginia locations to start this protective care.
Can I start Suboxone in pregnancy if I am currently using heroin?
Yes. In fact, starting treatment as soon as possible is recommended. Withdrawing “cold turkey” while pregnant is dangerous and carries a high risk of relapse and fetal harm. Transitioning to a stable dose of Suboxone under medical supervision is the safest path forward. You can find more scientific guidelines on substance use in pregnancy that support this stabilization approach.
Will my baby have withdrawal from Suboxone in pregnancy?
About 50% of babies exposed to opioids (including OAT) will show signs of withdrawal (NOWS) severe enough to require monitoring or medication. However, this is an expected and treatable condition. Most babies are observed in the hospital for about five days. Using tools like the Finnegan score or the newer “Eat, Sleep, Console” method, doctors can manage these symptoms effectively. For more info about how Suboxone treatment works during this phase, our team is always available to consult.
Conclusion
Navigating suboxone in pregnancy doesn’t have to be a source of stress. The science is clear: choosing treatment is a brave and healthy decision for both you and your baby. By staying on your medication, you are providing the stability your child needs to grow and thrive.
At National Addiction Specialists, we provide confidential, telemedicine-based care across Tennessee and Virginia. We understand the unique challenges of pregnancy and are here to support you with personalized recovery plans that you can access from the comfort of home. We accept Medicaid and Medicare, ensuring that high-quality care is accessible when you need it most.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. Make an Appointment
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.






