Unlocking Suboxone with Medicare Coverage
Your Path to Recovery with Medicare
Medicare Suboxone coverage is available through multiple pathways, offering hope for those seeking treatment for opioid use disorder. Here’s what you need to know:
Quick Answer: Does Medicare Cover Suboxone?
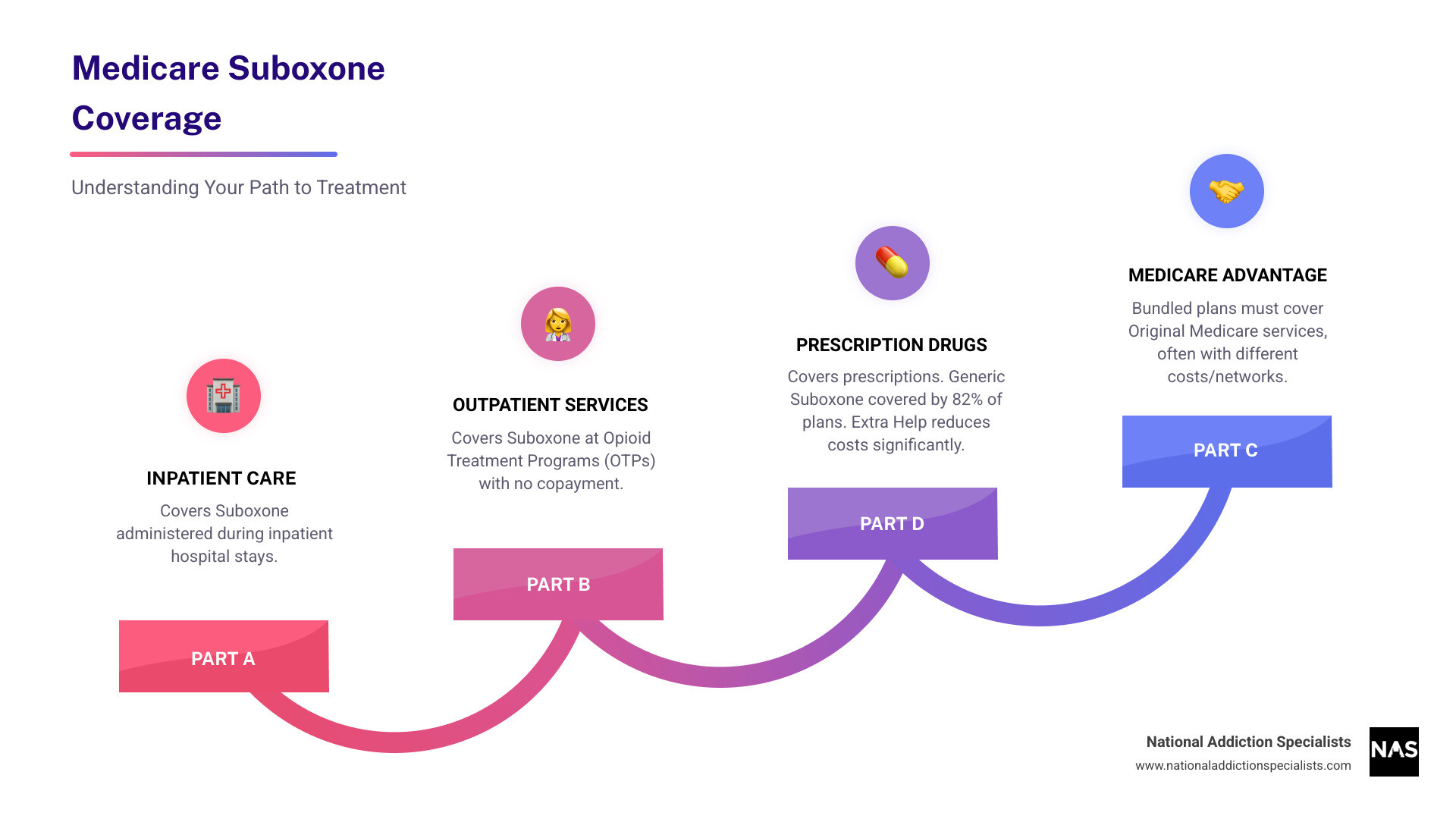
- Medicare Part A: Covers Suboxone during inpatient hospital stays
- Medicare Part B: Covers Suboxone at Opioid Treatment Programs (OTPs) with no copayment
- Medicare Part D: Covers Suboxone prescriptions (generic version covered by 82% of plans)
- Medicare Advantage: Must cover all services that Original Medicare covers
Key Cost Facts:
- Generic Suboxone costs dropped from $99 to $42 (2019-2020)
- With Extra Help program: $4.50 for generic, $11.20 for brand name
- OTP services have no out-of-pocket costs when Medicare-approved
If you’re struggling with opioid addiction, you’re not alone. The opioid crisis affects people from all walks of life, and Medicare recognizes this by covering comprehensive treatment options. Whether you need inpatient care, outpatient counseling, or prescription medications like Suboxone, Medicare provides multiple coverage pathways to help you access the treatment you deserve.
I’m Chad Elkin, MD, a board-certified addiction medicine physician and founder of National Addiction Specialists. I’ve helped countless patients steer Medicare Suboxone coverage to access life-saving treatment. Through my work with organizations like the American Society of Addiction Medicine, I’ve seen how proper coverage removes barriers to recovery.
Must-know Medicare Suboxone coverage terms:
Understanding Suboxone and Its Role in Opioid Addiction Treatment
Suboxone is an FDA-approved medication that has helped millions of people with opioid addiction. Understanding how it works is a key step in the recovery journey.
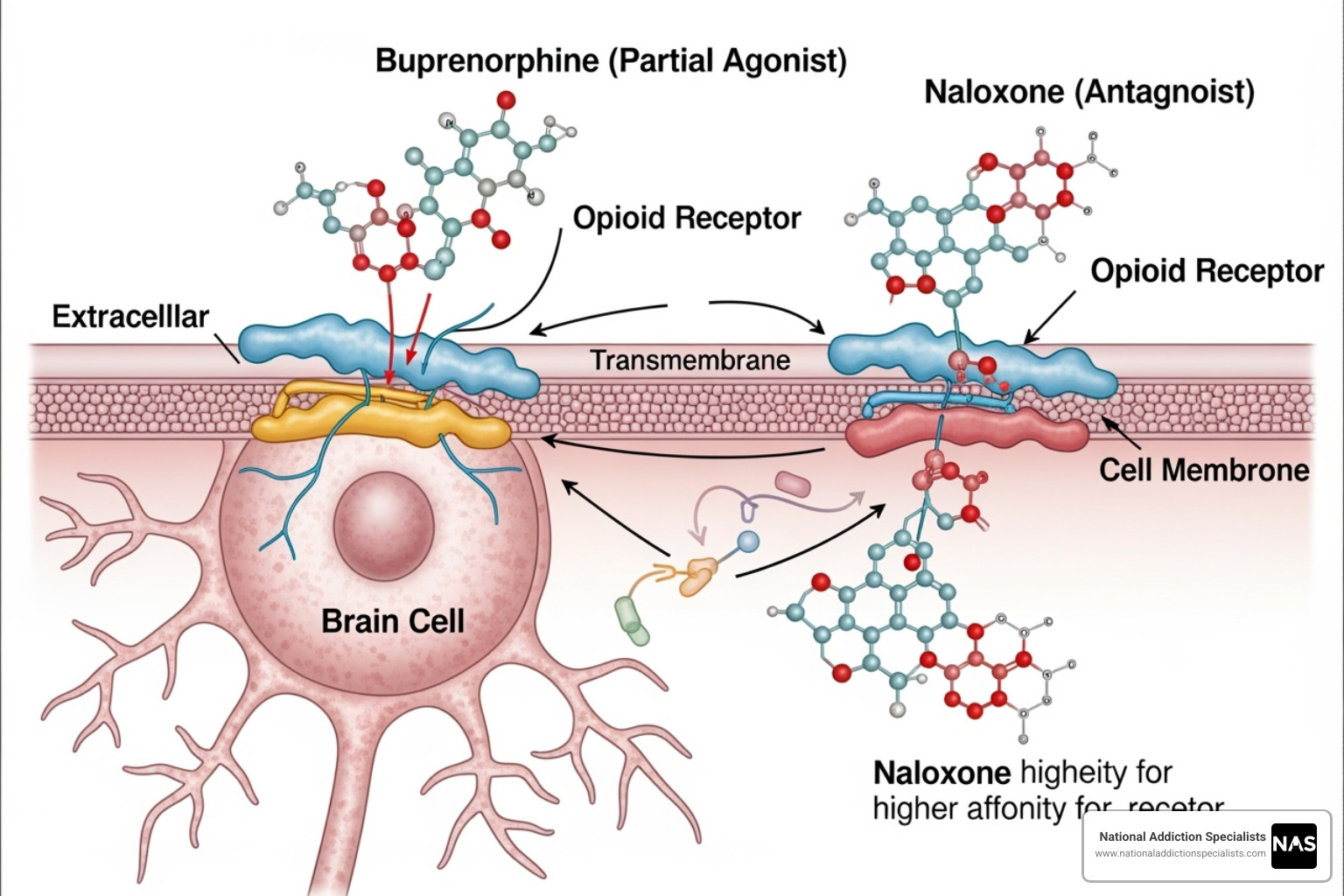
Suboxone is a combination of two medications. The first is buprenorphine, a partial opioid agonist that attaches to the same brain receptors as other opioids. It only partially activates these receptors, which means it can reduce cravings and ease withdrawal symptoms without producing a dangerous high.
The second ingredient is naloxone, an opioid blocker that acts as a safety net. If someone tries to misuse Suboxone by injecting it, naloxone blocks the opioid effects and can cause immediate withdrawal.
Suboxone isn’t a cure-all; it works best within a comprehensive treatment plan that includes counseling and therapy. Medicare Suboxone coverage often includes these additional services, addressing the physical, emotional, and psychological aspects of addiction.
To dive deeper into how this medication can transform lives, check out our detailed guide on What is Suboxone?. You might also find it helpful to explore the Benefits of Medication Assisted Treatment to see how this approach fits into your recovery plan.
Common and Serious Side Effects of Suboxone
Like any medication, Suboxone has potential side effects. Most are mild, manageable, and often improve as your body adjusts.
Common side effects you might experience include nausea, headache, and constipation. You might also notice dizziness, drowsiness, sweating, or some numbness in your mouth from the sublingual film or tablets. Staying hydrated and eating smaller meals can help manage these initial symptoms.
However, there are serious side effects that require immediate medical attention. Respiratory distress (slow, shallow, or difficult breathing) is the most concerning and needs emergency care. Allergic reactions like hives, swelling of your face or throat, or difficulty swallowing are also medical emergencies.
Watch for signs of liver problems like dark urine or yellowing of your skin and eyes, and be aware that extreme tiredness combined with dizziness and nausea could signal adrenal gland issues.
Open communication with your healthcare provider is key. Never hesitate to call if something doesn’t feel right. For the complete picture of potential side effects, you can review the official FDA information on Suboxone side effects.
Experiencing side effects doesn’t mean Suboxone isn’t right for you; it might just mean your dosage needs adjusting or you need additional support. Your recovery journey is unique, and your treatment should be too.
How Different Parts of Medicare Cover Suboxone
Understanding Medicare Suboxone coverage is straightforward once broken down. Which part of Medicare covers your Suboxone depends on where and how you receive treatment. Your specific plan also determines your out-of-pocket costs, as some plans have more generous coverage than others. Here’s a breakdown of each part.

Medicare Part A (Hospital Insurance) Coverage
Medicare Part A is your safety net for serious medical situations requiring hospital care. When it comes to Medicare Suboxone coverage, Part A steps in when you need inpatient treatment for opioid use disorder.
If you require hospitalization for severe withdrawal or complications, Part A covers Suboxone prescribed as part of your inpatient treatment plan. This also applies to care at a Medicare-approved skilled nursing facility. Part A treats Suboxone like any other medication you receive during a covered hospital stay—it’s bundled into your overall treatment costs. You will still be responsible for your Part A deductible and any applicable coinsurance for the hospital stay.
Medicare Part B (Medical Insurance) Coverage
Medicare Part B has significantly expanded its coverage for outpatient opioid use disorder treatment in recent years.
The biggest change is coverage for Opioid Treatment Programs (OTPs). These specialized programs provide comprehensive care. When you receive Suboxone at a Medicare-approved OTP, Part B covers the medication, counseling, therapy, and other support services. Crucially, there is often no copayment for these services at a Medicare-approved provider.
Part B also covers doctor visits and counseling sessions where Suboxone is part of your treatment plan. Visits with a psychiatrist, addiction specialist, or primary care doctor for opioid use disorder treatment fall under Part B. In some cases, Part B may cover Suboxone administered in a clinical setting, such as during intensive outpatient programs.
For more details about how Medicare approaches opioid treatment overall, check out our comprehensive guide: Medicare Opioid Treatment.
Medicare Part D (Prescription Drug Coverage) and Medicare Suboxone Coverage
Most people access Medicare Suboxone coverage for home use through Medicare Part D prescription drug plans, either as a standalone plan or as part of a Medicare Advantage plan.
Every Part D plan has a formulary, a list of covered medications organized into tiers that determine your cost.
Generic buprenorphine-naloxone has excellent coverage. As of 2020, 82% of Medicare Part D plans covered the generic film version. In recent years, brand-name Suboxone coverage dropped from 76% of plans in 2019 to 42% in 2020, while generic coverage soared, as plans favor cost-effective options.
Some plans require prior authorization, meaning your doctor must get approval before the plan covers Suboxone. This is a standard process to demonstrate medical necessity.
To understand your specific coverage and costs, check your plan’s formulary. You can find more details on how formularies work on the official Medicare website.
Medicare Part C (Medicare Advantage) Coverage
Medicare Advantage plans bundle all your Medicare benefits. These plans must cover everything that Original Medicare covers, so you are guaranteed access to Medicare Suboxone coverage.
Most Medicare Advantage plans include prescription drug coverage. The trade-off is that you’ll typically need to stay within the plan’s network of doctors, hospitals, and pharmacies. Each plan sets its own formulary and cost-sharing rules, so it’s important to review your specific plan’s coverage for Suboxone and ensure your preferred providers are in-network.
Navigating the Costs of Suboxone with Medicare
Medicare significantly reduces the financial burden of Suboxone treatment, though some out-of-pocket expenses remain. Your exact costs depend on your specific Medicare plan, your choice of brand-name or generic medication, and where you receive treatment.

Understanding Your Potential Out-of-Pocket Costs
In 2024, Medicare costs include premiums, deductibles, copayments, and coinsurance.
For Part B costs, the monthly premium is $174.70 with a $240 annual deductible. Afterward, you typically pay 20% of the Medicare-approved amount. However, if you receive Suboxone at a Medicare-approved Opioid Treatment Program, you won’t have any out-of-pocket costs for those services.
For Part D costs, the average monthly premium is $55.50, with a maximum annual deductible of $545. After your deductible, you pay your plan’s copayment or coinsurance. A 30-day supply of Suboxone without insurance could cost $160 to $570, but with Medicare, these costs drop dramatically.
The Shift from Brand-Name to Generic Suboxone
The increased availability of generic Suboxone has been a game-changer for patients. The median out-of-pocket cost for buprenorphine-naloxone films dropped nearly 60%, from $99 in 2019 to just $42 in 2020.
This dramatic decrease in out-of-pocket costs is due to widespread generic coverage. While brand-name costs have risen slightly, generic alternatives keep expenses affordable. Coverage of generic buprenorphine-naloxone tablets climbed from 68% in 2015 to 85% in 2022.
A 2023 study on generic entry confirms how brand-name cost trends shifted after generics entered the market in 2018. You are now far more likely to find affordable generic options covered by your Part D plan.
Financial Assistance: The Extra Help Program
If money is tight, the Low Income Subsidy (LIS), or Extra Help, can make medication costs manageable.
The 2024 cost limits for those who qualify are remarkable. With Extra Help, the maximum you’d pay for Suboxone is $11.20 for the brand name and just $4.50 for the generic. These reduced drug costs can be life-changing.
Eligibility depends on your income and resources, but it’s worth checking if you qualify. The program helps with monthly premiums, deductibles, and copayments. You can learn more and apply for this program at the official Medicare website: Help with drug costs. Taking advantage of available assistance is a smart way to take control of your recovery.
Comprehensive Medicare Suboxone Coverage for Opioid Use Disorder
Medicare Suboxone coverage is comprehensive, extending beyond medication to include counseling, therapy, and specialized programs. Medicare’s approach supports whole-person healing, which is essential for lasting recovery.
Opioid Treatment Programs (OTPs) and Medicare
Opioid Treatment Programs (OTPs) are specialized facilities designed for people with opioid use disorder.
A key benefit of Medicare is that if you receive treatment at a Medicare-approved OTP, you pay nothing out-of-pocket for those services. This removes a significant financial barrier to accessing care.
OTPs serve as a recovery command center, providing:
- Medication like Suboxone, with guidance on proper use.
- Individual and group counseling to address the emotional side of addiction.
- Drug testing to track progress and ensure accountability.
- Intake activities and regular check-ins to monitor your treatment plan.
- Intensive outpatient program services for more structured support.
- Peer recovery support from others with shared experiences.
Medicare maintains a directory of approved providers. You can search for one near you here: Find Medicare-approved OTPs.
Other Covered Therapies
Beyond OTPs, Medicare covers a toolkit of therapies to support recovery. Individual therapy provides one-on-one time with a mental health professional to address root causes and develop coping strategies.
Group therapy offers peer support and shared wisdom from others in recovery, providing powerful proof that recovery is possible.
Medicare also covers Screening, Brief Intervention, and Referral to Treatment (SBIRT) under Part B, which helps identify and address substance use issues early.
For more intensive support, Medicare covers Intensive Outpatient Programs (IOPs) and Partial Hospitalization Programs (PHPs). These programs offer structured, comprehensive care during the day, including therapy, counseling, and medication management.
This comprehensive approach treats you as a whole person, reflecting the reality that recovery touches every part of your life.
To explore the full range of treatment approaches available, check out our page on Medication Assisted Treatment Options.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Frequently Asked Questions about Medicare and Suboxone
Navigating Medicare Suboxone coverage can be confusing. Here are answers to some of the most common questions.
Is the generic version of Suboxone as effective?
Yes, the generic version of Suboxone (buprenorphine-naloxone) is just as effective as the brand-name version. The FDA requires generic medications to be bioequivalent, meaning they have the same active ingredients and work the same way in the body.
Some patients notice minor differences, such as taste or how a film dissolves. A 2023 study noted that a small number of patients experienced temporary withdrawal or cravings when switching. However, these experiences are not typical. The adjustment period is usually brief, and most patients transition smoothly, enjoying significant cost savings.
If you have concerns after switching, talk to your doctor. A simple dosage adjustment or trying a different generic manufacturer can often resolve any issues.
Do I need prior authorization for Suboxone with Medicare?
Whether you need prior authorization depends on your specific plan. It is a process where your insurance provider verifies that the medication is medically necessary before covering it. Many Medicare Part D and Medicare Advantage plans require it, especially for brand-name drugs.
This is not an attempt to deny treatment. Your doctor’s office will typically handle the paperwork, submitting documentation to explain why you need Suboxone. Most requests are approved within a few days. When choosing a plan, check its formulary to see how it covers buprenorphine-naloxone.
Can I get Suboxone through telehealth with Medicare?
Yes. Medicare has significantly expanded telehealth coverage, which has been a game-changer for people seeking opioid use disorder treatment.
Through telehealth, you can receive counseling, therapy, and your Suboxone prescription from home. This eliminates barriers like travel time, taking time off work, and privacy concerns. Telehealth is particularly beneficial for people in rural areas, eliminating long travel times to see a specialist. The convenience often leads to better treatment adherence and outcomes.
At National Addiction Specialists, we’ve built our practice around telemedicine-based Suboxone treatment. We serve patients throughout Tennessee and Virginia, and we accept both Medicare and Medicaid. If you’re interested in learning more, check out our Telehealth Suboxone Treatment page.
Seeking help for opioid addiction is one of the bravest things you can do. Don’t let concerns about insurance or logistics stop you from getting the treatment you deserve.
Conclusion: Taking the Next Step in Your Recovery
Navigating Medicare Suboxone coverage reveals that Medicare provides strong support for opioid addiction treatment. Whether through Part A, Part B, Part D, or Medicare Advantage, there is a pathway to get the care you need.
The shift to generic Suboxone has dramatically lowered costs, and programs like Extra Help can reduce them even further, to as little as $4.50 for a generic prescription.
The key is to understand your specific plan’s benefits. Contact your plan provider or a healthcare professional to learn about your exact coverage and avoid surprise costs.
Seeking help for opioid use disorder is a sign of strength. It takes courage to start treatment, a step that can save your life and improve the lives of those around you.
At National Addiction Specialists, our mission is to remove barriers to recovery. We provide convenient, confidential telemedicine-based Suboxone treatment right to your home, eliminating worries about travel or time off work. We serve communities throughout Tennessee and Virginia and proudly accept Medicare to ensure quality care is accessible.
Your recovery journey is yours, but you don’t have to walk it alone. We offer personalized treatment plans that fit your life.
Take that brave next step today. Learn more about our Medication-Assisted Treatment program and find out how we can help you reclaim your path to a healthier future. You deserve this chance.
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.








