How Clonidine Helps You Kick Opiates for Good
What Clonidine Actually Does for Opiate Withdrawal (And Why It Matters)
Clonidine for opiate withdrawal is one of the most widely used non-opioid tools to ease the physical storm of detox — and if you’re trying to stop opiates without replacing one dependency with another, it’s worth understanding how it works.
Here’s a quick answer:
- What it is: Clonidine is a blood pressure medication used off-label to reduce opiate withdrawal symptoms
- How it helps: It calms the overactive nervous system that causes sweating, anxiety, racing heart, and muscle cramps during withdrawal
- What it doesn’t do: It won’t stop cravings, insomnia, or muscle aches completely
- Who uses it: People detoxing from heroin, prescription opioids, or methadone — in both inpatient and outpatient settings
- Key fact: It’s not an opioid, so it carries no opioid dependency risk
Opiate withdrawal isn’t usually life-threatening — but it can feel unbearable. That’s exactly why so many people relapse in the first few days of trying to quit. Clonidine doesn’t make withdrawal easy, but clinical evidence shows it can make it survivable — and even help extend abstinence well beyond the detox window.
I’m Chad Elkin, MD, board-certified in Addiction Medicine, and as the founder of National Addiction Specialists, I’ve used clonidine for opiate withdrawal as part of individualized treatment plans for patients across Tennessee and Virginia. In this guide, I’ll walk you through exactly how it works, what to expect, and how it fits into a complete recovery plan.
Glossary for clonidine for opiate withdrawal:
What is Clonidine and How Does it Work for Opiate Withdrawal?
At its core, clonidine is a medication approved by the FDA primarily to treat high blood pressure (hypertension). It belongs to a class of drugs known as alpha-2 adrenergic agonists. While that sounds like a mouthful, its job is actually quite straightforward: it tells your brain to dial back the “fight or flight” response.
When someone uses opioids for a long time, the brain adjusts by suppressing certain chemicals, like norepinephrine. When the opioids are suddenly removed, the brain overcompensates by flooding the system with norepinephrine. This “adrenergic storm” is responsible for the racing heart, high blood pressure, and intense anxiety that make withdrawal so miserable.
Clonidine works by binding to specific receptors in the brain to inhibit the release of this excess norepinephrine. By calming the sympathetic nervous system, it acts as a chemical brake, slowing down the physical sensations of panic and distress that characterize the early stages of recovery.
Off-Label Use in Addiction Medicine
Even though the off-label use of clonidine for withdrawal isn’t its primary FDA-approved purpose (it’s also used for ADHD and hot flashes), it has been a staple in addiction medicine for decades. We use it specifically to target “autonomic hyperactivity.”
Think of it this way: if your body is an engine redlining during withdrawal, clonidine is the coolant that prevents it from overheating. It bridges the gap between active use and stabilization, providing a non-addictive way to manage the physical symptoms of quitting.
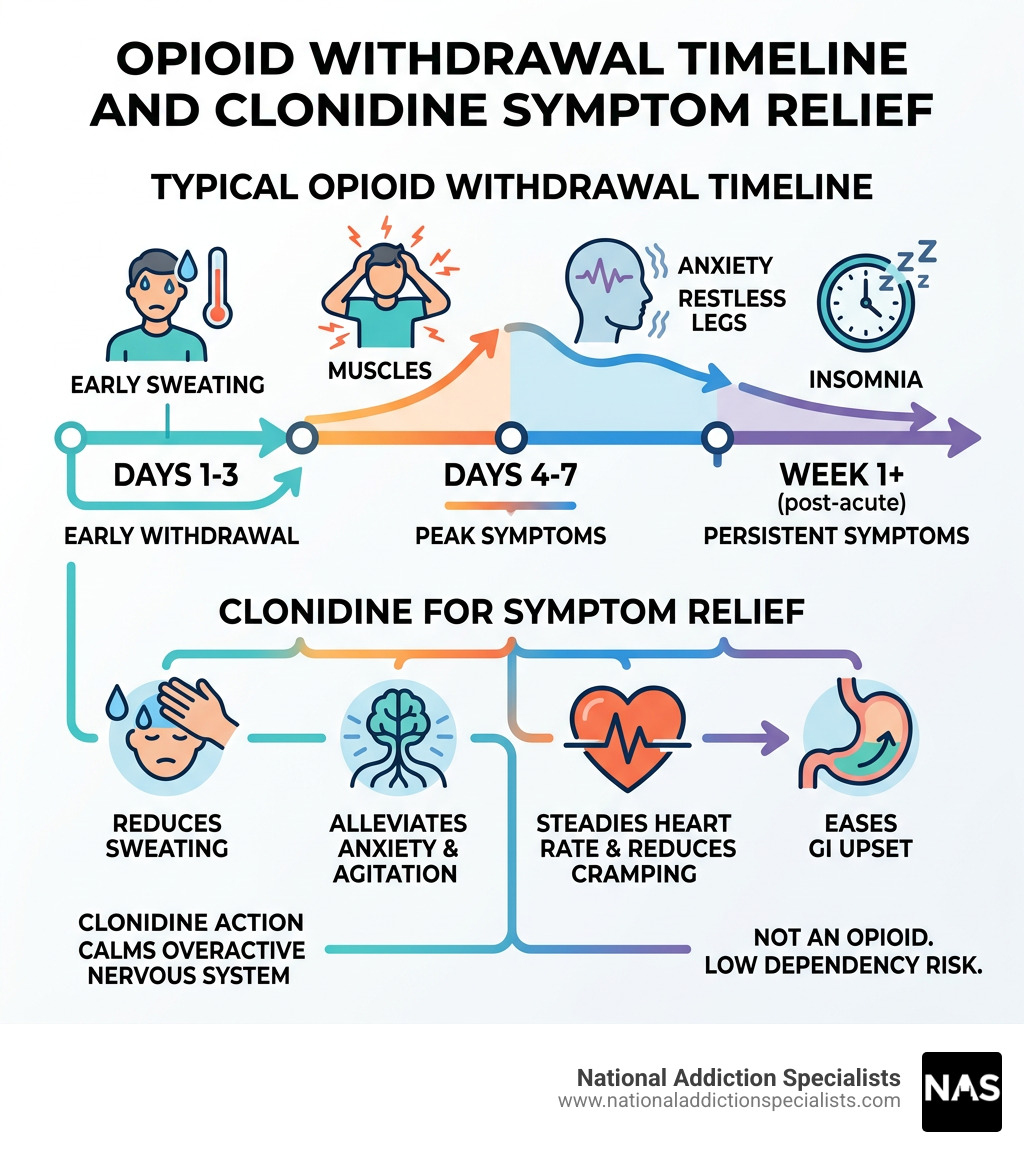
Managing Symptoms: What to Expect During Detox
When you begin the journey of Opioid Withdrawal, your body goes through a predictable but painful set of stages. Short-acting opioids like heroin usually trigger symptoms within 8–24 hours, while long-acting ones like methadone may take up to 48 hours to start.
Clonidine for opiate withdrawal is particularly effective at relieving:
- Excessive sweating and chills
- Runny nose and watery eyes
- High blood pressure and rapid heart rate
- Restlessness and intense anxiety
- Abdominal cramps and diarrhea
By addressing these “wet” symptoms (sweating, tearing, GI issues), clonidine helps you stay hydrated and physically stable enough to focus on the next steps of your recovery.
Limitations of Clonidine for Opiate Withdrawal
It is important to be realistic: clonidine is a powerful tool, but it isn’t a “magic pill” that makes withdrawal disappear. Research and clinical experience show that clonidine is often less effective against:
- Insomnia: You may still struggle to sleep during the first few nights.
- Muscle Aches: While it helps with cramps, deep bone and muscle aches may persist.
- Physical Cravings: Clonidine does not satisfy the brain’s hunger for opioids the way Medication Assisted Treatment (MAT) like Suboxone does.
Because of these limitations, we often use clonidine as one part of a larger toolkit, sometimes combining it with other comfort medications to ensure you are as comfortable as possible.
Dosage, Administration, and Safety Protocols
Safety is our primary concern when prescribing clonidine for opiate withdrawal. Because it was designed to lower blood pressure, taking too much can cause your blood pressure or heart rate to drop to dangerous levels.
Typical administration protocols include:
- Oral Tablets: Available in 0.1 mg, 0.2 mg, and 0.3 mg doses. In an outpatient setting, we usually start with 0.1 mg to 0.2 mg taken several times a day.
- Transdermal Patches: These provide a steady release of medication through the skin over seven days, which can be helpful for maintaining consistent levels in the bloodstream.
- Daily Dosage: Most patients require between 0.5 mg and 1.4 mg per day, with the highest doses usually needed between days two and four of detox.
Clinical guidelines for withdrawal management emphasize that dosing must be individualized. What works for one person might make another feel too dizzy to stand up.
Safety Precautions for Clonidine for Opiate Withdrawal
Before every dose, especially in the early days, it is vital to monitor vital signs. According to Cochrane evidence on alpha2-adrenergic agonists, the most common side effects are sedation (sleepiness), dry mouth, and dizziness.
We generally follow a strict 90/50 mmHg threshold. If your blood pressure drops below 90 systolic (the top number) or 50 diastolic (the bottom number), or if your heart rate becomes too slow (bradycardia), the medication must be held or adjusted. This is why professional medical supervision is so important—trying to dose clonidine on your own can lead to fainting or even more serious heart issues.
Comparing Clonidine to Suboxone and Other Treatments
When choosing a path for recovery, it helps to see how different medications stack up. Clonidine is often compared to lofexidine (the only non-opioid FDA-approved specifically for withdrawal) and buprenorphine (the active ingredient in Suboxone).
| Feature | Clonidine | Lofexidine | Buprenorphine (Suboxone) |
|---|---|---|---|
| Drug Class | Alpha-2 Agonist | Alpha-2 Agonist | Partial Opioid Agonist |
| Opioid Content | None | None | Contains Opioid |
| Cravings Relief | Low | Low | High |
| Prescribing Ease | Non-Scheduled | Non-Scheduled | Scheduled (DEA required) |
| BP Impact | Significant Drop | Mild Drop | Minimal |
Understanding How Suboxone Treatment Works highlights a key difference: Suboxone actually attaches to opioid receptors to stop cravings and withdrawal entirely. Clonidine, however, is non-scheduled, meaning it has no potential for addiction and doesn’t require the same strict federal oversight as opioid-based treatments.
Strategic Utility in Recovery
For many of our patients in Tennessee and Virginia, clonidine serves as a “transitional treatment.” Research on clonidine and naltrexone shows it is excellent for helping patients clear opioids from their system so they can safely start naltrexone (Vivitrol), which requires a person to be 7–10 days “clean” first.
It is a vital part of a comprehensive Opioid Addiction Treatment plan for those who prefer a non-opioid route or who need help bridging the gap between different phases of recovery.
Beyond Detox: Clonidine for Relapse Prevention
One of the most exciting areas of Scientific research on stress decoupling suggests that clonidine’s benefits don’t end when the physical withdrawal stops.
Stress is one of the biggest triggers for relapse. When you get stressed, your brain releases norepinephrine—the same chemical that spikes during withdrawal. This can trigger an intense “need” for opioids to calm down. Studies have shown that low-dose clonidine maintenance can “decouple” stress from cravings. In one study, patients on clonidine stayed abstinent for an average of 34.8 days compared to 25.5 days for those on a placebo.
By keeping the body’s stress response in check, clonidine acts as a safety net. While it’s not a standalone cure, it can be a powerful adjunctive maintenance tool alongside your primary Suboxone Treatment FAQ or counseling sessions.
Frequently Asked Questions
Is clonidine for opiate withdrawal safe for everyone?
Not necessarily. While it is generally safe, people with certain heart conditions, very low baseline blood pressure, or severe kidney disease should be cautious. MedlinePlus safety info also notes that pregnant women should generally avoid opioid withdrawal altogether due to risks to the fetus; in these cases, maintenance therapy is usually the gold standard. Always disclose your full medical history to us before starting.
How long do I take clonidine for opiate withdrawal?
The typical “detox window” for clonidine is 7 to 10 days. We usually start with a higher dose during the peak of withdrawal and then implement a tapering schedule. It is crucial not to stop clonidine abruptly, as this can cause “rebound hypertension”—a sudden, dangerous spike in blood pressure.
Can I use clonidine at home?
Yes, but it requires a plan. At National Addiction Specialists, we provide outpatient protocols that allow you to recover in the comfort of your home in Tennessee or Virginia. To ensure safety, clinical guidelines often recommend limiting outpatient prescriptions to a three-day supply at a time to prevent accidental overdose or misuse. Through our telemedicine platform, we can monitor your progress and adjust your dose without you having to travel to a clinic while you’re feeling unwell.
Conclusion
At National Addiction Specialists, we believe that recovery should be accessible, confidential, and tailored to your life. Whether you are looking for a non-opioid approach using clonidine for opiate withdrawal or a long-term Medication Assisted Treatment Program, we are here to help.
Our telemedicine-based care serves residents throughout Tennessee and Virginia, offering expert medical guidance from the privacy of your own home. We accept Medicaid and Medicare, ensuring that high-quality addiction care is within reach for everyone. You don’t have to suffer through withdrawal alone—let us help you build a personalized plan to reclaim your future.
Make an Appointment to Treat Addiction Please don’t hesitate. Make an appointment today. https://www.nationaladdictionspecialists.com/new-patient-packet/
This article was medically reviewed by: Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment. Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.