Buprenorphine Tapering Schedules: Finding Your Fast Track to Freedom
Why Fast Suboxone Taper Matters for Your Recovery

A fast Suboxone taper is a shorter, medically supervised process to discontinue buprenorphine/naloxone treatment, typically lasting 3-7 days. Here’s what you need to know:
Key Facts About Fast Suboxone Taper:
- Duration: 3-7 days vs. 28+ days for slower tapers
- Success Rate: 44% achieved opioid-free status at end of fast taper vs. 30% with slow taper
- Medical Supervision: Essential for safety and managing withdrawal
- Withdrawal: Generally mild when done correctly and managed with comfort medications
- Long-term Results: No significant difference in abstinence rates at 3 months compared to slower tapers
If you’re taking Suboxone for opioid use disorder, you might be wondering when and how to stop. Whether you’ve been stable for months, are tired of daily medication, or simply want to move forward without dependence, a taper is the next step.
The good news is that a fast taper can work. Research shows it can be just as effective as a longer taper for many people.
The catch? You absolutely need medical guidance. Quitting cold turkey is dangerous. It can trigger severe withdrawal, increase your relapse risk, and even lead to overdose if you return to opioid use.
A proper taper means gradually reducing your dose under a doctor’s care, giving your body time to adjust while minimizing discomfort.
I’m Dr. Chad Elkin, a board-certified addiction medicine physician and founder of National Addiction Specialists. I’ve helped hundreds of patients successfully complete fast Suboxone taper schedules through personalized telemedicine. In this guide, I’ll walk you through tapering safely and effectively.
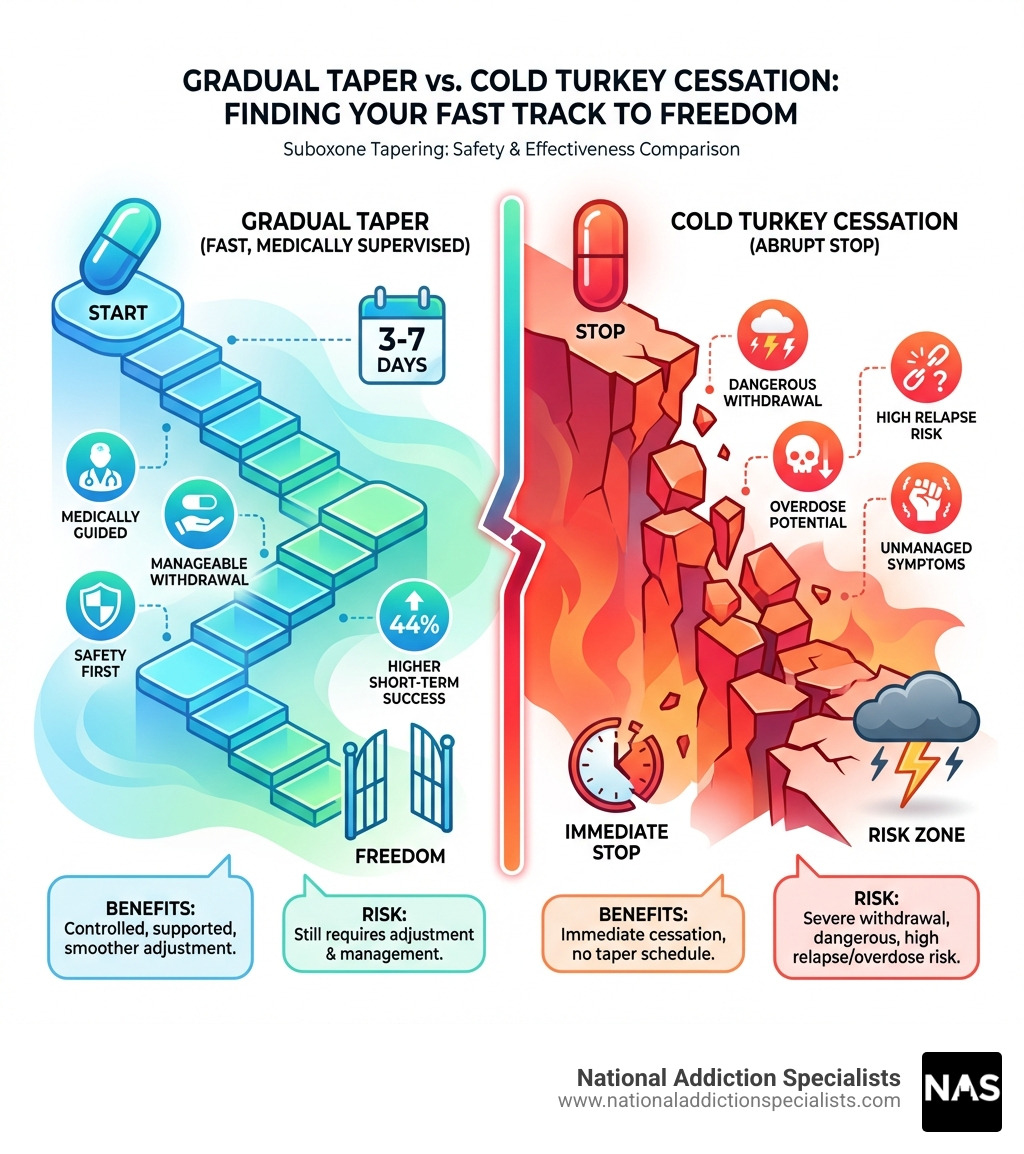
Understanding the Suboxone Taper: Why and How
Suboxone (buprenorphine and naloxone) is a crucial part of medication-assisted treatment (MAT) for opioid use disorder. It helps people overcome dependence on stronger opioids like heroin. Buprenorphine, a partial opioid agonist, alleviates withdrawal symptoms and cravings, allowing for stabilization and therapy. Naloxone is included to deter misuse; it’s inactive when taken as prescribed but causes immediate withdrawal if injected.
While Suboxone is a vital recovery tool, it causes physical dependence, which is different from addiction. Physical dependence means your body has adapted to the medication and will experience withdrawal if it’s stopped suddenly. Addiction involves compulsive drug-seeking despite negative consequences. Tapering off Suboxone addresses this physical dependence.
Abruptly stopping Suboxone, or quitting “cold turkey,” can lead to a severe and prolonged withdrawal syndrome. Buprenorphine, the active opioid in Suboxone, has a long half-life of about 36 hours. This means it stays in your system for an extended period, leading to a slower onset of withdrawal symptoms that can be long-lasting and uncomfortable if not managed properly.
A gradual taper allows your body and brain to slowly adjust to decreasing amounts of the medication. This smooth transition minimizes the intensity of withdrawal symptoms, making the process more manageable and increasing your chances of a successful outcome.
Why Tapering is Safer Than Quitting Cold Turkey
The idea of quitting “cold turkey” might seem appealing, but for anyone physically dependent on opioids like Suboxone, this approach is incredibly difficult and dangerous.
Opioid withdrawal is challenging. Suddenly stopping sends your system into overdrive, causing symptoms from flu-like discomfort to severe psychological distress like muscle aches, nausea, vomiting, diarrhea, sweating, insomnia, anxiety, and depression. These debilitating symptoms can push individuals back to opioid use for relief.
The risk of relapse is significantly higher when quitting cold turkey. The unbearable discomfort and intense cravings are powerful triggers. If a person relapses after a period of abstinence, their opioid tolerance will have decreased, meaning that taking their previous dose can lead to a fatal overdose. This is why medical professionals strongly advise against unsupervised, abrupt cessation.
Moreover, Suboxone withdrawal is protracted. Unlike withdrawal from short-acting opioids like heroin which may resolve in 10 days, Suboxone withdrawal can begin 12-48 hours after the last dose and last for 20 days or more, especially psychological symptoms. This extended discomfort can be demoralizing without support.
A medically supervised taper, even a fast Suboxone taper, is designed to ease your body off the medication safely. It’s a controlled process that allows us to manage symptoms, adjust your dose, and provide the necessary support to ensure a successful transition and improve long-term outcomes.
A Guide to Your Fast Suboxone Taper: Methods and Schedules
Starting a fast Suboxone taper is a significant step that requires medical supervision for your safety and comfort. We create a personalized taper plan based on your history, dosage, and response. It’s a custom journey, not a one-size-fits-all approach.
The convenience of telemedicine, which we offer at National Addiction Specialists in Tennessee and Virginia, makes accessing this crucial medical guidance easier than ever. You can receive expert care, monitoring, and support from the comfort and privacy of your home, removing many barriers that might otherwise prevent you from pursuing a taper.
Different Tapering Approaches
When tapering off Suboxone, we prioritize safe and effective approaches that minimize discomfort.
The most common and expert-recommended method is Direct Tapering. This involves gradually reducing your Suboxone dose over a set period. The pace of reduction is critical to allow your body to adapt without overwhelming withdrawal.
Another method is the Bernese Method, which involves micro-dosing buprenorphine while gradually decreasing your Suboxone dose. This method is often used to transition from full opioid agonists to buprenorphine, or sometimes to taper off buprenorphine itself, aiming for a less uncomfortable process.
However, there are methods we do not recommend due to ineffectiveness or potential harm:
- Titration Tapering: Mixing Suboxone with water and drinking smaller amounts is not recommended because it does not dissolve completely. This makes dosing inconsistent and dangerous.
- Substitute Tapering: Switching to another long-acting opioid to taper off Suboxone is generally unnecessary, as Suboxone itself is long-acting.
Creating a Fast Suboxone Taper Schedule
While “fast,” a fast Suboxone taper is still a carefully managed process, typically completed within 3 to 7 days. This accelerated approach is often suitable for individuals on lower doses, those who have been on Suboxone for a shorter period, or whose health allows for a rapid reduction.
For instance, a case study showed a successful 3-day Suboxone taper:
- Day 1: 4mg/1mg in the morning and 4mg/1mg in the evening (total 8mg/2mg)
- Day 2: 2mg/0.5mg in the morning and 2mg/0.5mg in the evening (total 4mg/1mg)
- Day 3: 2mg/0.5mg in the morning
This patient reported only mild withdrawal symptoms, which were managed with comfort medications.
Another example is a 6-day model seen in research:
- Initial dose: 16 mg/day
- Day one: 12 mg/day
- Day two: 10 mg/day
- Day three: 8 mg/day
- Day four: 4 mg/day
- Day five: 2 mg/day
- Day six: 2 mg/day
These are just examples; your plan will be unique. A general guideline is to reduce your dose by no more than 25% at a time to prevent withdrawal. The key is to listen to your body and communicate with your provider. If symptoms become too intense, we can adjust the schedule by pausing or slowing the taper.
A doctor-prescribed schedule is crucial. Self-tapering is risky and can lead to unnecessary suffering or relapse. We will create a precise plan to guide you through each step of your fast Suboxone taper.
Fast vs. Slow Taper: What Does the Research Say?
The ideal duration of a Suboxone taper is often debated. While many assume a slower taper is better, research challenges this, especially for short-term outcomes.
A notable study on buprenorphine tapering schedules compared the outcomes of a 7-day versus a 28-day taper group. The findings offer valuable insights into the efficacy of different taper durations.
Here’s a comparison of the key outcomes:
| Outcome | Fast Taper (7-day group) | Slow Taper (28-day group) |
|---|---|---|
| Opioid-free urine specimens at end of taper | 44% | 30% |
| Opioid-free urine specimens at 1-month follow-up | 18% | 18% |
| Opioid-free urine specimens at 3-month follow-up | 12% | 13% |
| Medications for withdrawal symptoms used | Fewer | More |
| Clinical withdrawal symptoms (COWS) at 1-month follow-up | Greater | Less |
| Self-reported withdrawal/craving at 1-month follow-up | No difference | No difference |
| Patient satisfaction at 3-month follow-up | Lower | Greater |
This table shows that a fast Suboxone taper (7-day) resulted in a higher percentage of opioid-free urine specimens at the end of the taper compared to a 28-day schedule, challenging the assumption that “slower is always better” for initial cessation.
The Benefits and Risks of a Fast Suboxone Taper
Understanding a fast Suboxone taper involves looking at its potential advantages and disadvantages.
Potential Benefits:
- Higher Initial Opioid-Free Rates: Research shows a 7-day taper resulted in a 44% opioid-free rate at the end, versus 30% for a 28-day taper. A quicker process can provide momentum and a sense of achievement.
- Fewer Comfort Medications Used: The 7-day taper group used fewer medications for withdrawal symptoms, suggesting the experience may be less burdensome for some when closely supervised.
- Reduced Overall Treatment Time: A shorter taper is appealing for those eager to move to the next phase of recovery.
Potential Risks:
- Higher Clinical Withdrawal Scores at 1-Month Follow-up: The 7-day group showed greater clinical withdrawal symptoms (COWS scale) at the 1-month follow-up, suggesting the body may still be adjusting.
- Lower Patient Satisfaction at 3 Months: The 28-day taper group reported greater satisfaction at 3 months, possibly due to a more gradual adjustment period.
- Increased Risk of Discomfort if Not Managed Properly: A faster pace requires diligent medical supervision to manage discomfort and adjust the schedule as needed.
Long-Term Outcomes and Success Rates
Reassuringly, the research found no significant differences in opioid abstinence rates at the 1-month and 3-month follow-ups between the 7-day and 28-day groups. This suggests a well-managed fast Suboxone taper can be just as effective for sustained abstinence in the short-to-medium term.
This highlights that the taper is just one part of the journey. Comprehensive post-taper support is vital for long-term success. One option is naltrexone, an opioid antagonist that can be started after buprenorphine has cleared your system. As discussed in guidelines on maintenance and discontinuation of buprenorphine, naltrexone blocks opioid receptors, reducing relapse risk.
Beyond medication, ongoing counseling and behavioral therapy are crucial. These therapies teach coping mechanisms and relapse prevention strategies. Committing to continued support after the taper is key to long-term freedom.
Managing Withdrawal Symptoms During Your Taper
Even with a planned fast Suboxone taper, some withdrawal is normal as your body adjusts. It’s not a sign of failure. These symptoms can be managed with medical support, and our goal is to make the process as comfortable as possible and prevent symptoms from becoming overwhelming.
Common Suboxone Withdrawal Symptoms
Suboxone withdrawal symptoms are similar to those of other opioids but can be prolonged due to buprenorphine’s long half-life. Symptoms can begin 12 to 48 hours after your last dose and persist for up to 20 days or longer for some psychological effects.
Here are common symptoms you might experience, as outlined in withdrawal symptom lists:
Physical Symptoms:
- Muscle aches and joint pain
- Trouble sleeping (insomnia)
- Runny eyes and nose
- Excessive sweating
- Frequent yawning
- Enlarged pupils
- Abdominal cramps and stomach pain
- Diarrhea
- Goosebumps
- Nausea and vomiting
- Lethargy and fatigue
- Headaches
- Fever and chills
Psychological Symptoms:
- Agitation and restlessness
- Anxiety and panic attacks
- Depression and low mood
- Irritability
- Intense drug cravings
- Difficulty concentrating
Physical symptoms are often most acute in the first 72 hours, while psychological symptoms like depression can linger. This is why comprehensive emotional support during tapering is so important.
Strategies for Symptom Management
The cornerstone of managing withdrawal during a fast Suboxone taper is robust medical support. We monitor your symptoms using tools like the Clinical Opiate Withdrawal Scale (COWS) and adjust your plan as needed.
Here are some strategies we employ:
- Comfort Medications: We can prescribe non-opioid medications to target specific symptoms, such as:
- Clonidine: For anxiety, restlessness, and sweating.
- Anti-nausea medications (e.g., promethazine): For nausea and vomiting.
- Anti-diarrhea medications (e.g., loperamide): For digestive upset.
- Over-the-counter pain relievers (e.g., acetaminophen, ibuprofen): For muscle aches.
- Sleep aids (e.g., melatonin): For insomnia. Short-term benzodiazepines may be used with extreme caution due to their addictive potential.
- Adjusting the Taper Schedule: If withdrawal becomes too severe, we can slow down or pause your taper. Your comfort and safety are our top priorities.
- Self-Care Strategies: Healthy self-care practices can significantly ease discomfort:
- Hydration: Drink plenty of water and electrolyte-rich fluids.
- Nutrition: Eat a balanced diet; small, frequent meals can help with nausea.
- Light Exercise: Gentle activities like walking can boost mood.
- Sleep Hygiene: Establish a regular sleep schedule and a relaxing bedtime routine.
- Holistic Approaches: Many find relief through complementary therapies:
- Meditation and Mindfulness: To manage anxiety and cope with discomfort.
- Yoga and Deep Breathing: To reduce tension and promote relaxation.
- Journaling: To process feelings and psychological symptoms.
You don’t have to endure this alone. We’re here to guide you through every step.
Make an Appointment to Treat Addiction
Please don’t hesitate. Make an appointment today.
Building Your Support System for a Successful Taper
Tapering off Suboxone is a journey best traveled with a strong support system. Recovery is not a solo endeavor; a network of professionals, peers, and loved ones is crucial for navigating challenges. We empower you with comprehensive support beyond just medication management.
The Crucial Role of Medical Professionals
Your medical provider is your primary guide during the fast Suboxone taper. We will:
- Create a Safe Plan: Develop an individualized, flexible taper schedule based on your needs and health status.
- Monitor Progress: Use regular check-ins to monitor your symptoms and ensure the taper is proceeding safely.
- Manage Complications: Intervene promptly with medications or plan adjustments if severe symptoms arise.
Our telemedicine approach allows you to access this support conveniently from your home in Tennessee or Virginia. We are committed to providing expert care that fits your life. You can find more info about our insurance and pricing to understand how our services can be accessible.
Finding Support Beyond Your Doctor
While medical guidance is paramount, a holistic approach includes various forms of support:
- Therapy and Counseling: Individual therapy helps you develop coping mechanisms, while group therapy provides validation and reduces isolation.
- Peer Support: Connecting with peers who understand your journey is powerful. This includes 12-Step treatment programs like Narcotics Anonymous (NA) and online support communities.
- National Resources: Helplines like SAMHSA’s national helpline offer immediate support and can connect you to local resources.
- Aftercare Planning: A successful taper is about building a sustainable, sober life. We’ll help you develop an aftercare plan with ongoing therapy, support groups, and healthy lifestyle choices to prevent relapse.
Conclusion
Deciding to taper off Suboxone is a significant and empowering step in your recovery journey. While a fast Suboxone taper might sound intimidating, our research and clinical experience show that it can be a highly effective and manageable option for many individuals, especially when conducted under strict medical supervision. It offers a quicker path to being medication-free without compromising your chances of long-term abstinence compared to longer tapers.
The key to success lies in a personalized approach, expert medical guidance, and a robust support system. We understand that every individual’s journey is unique, and we are dedicated to crafting a taper plan that prioritizes your comfort, safety, and long-term sobriety. Whether you are in Brentwood, Tennessee, or Virginia Beach, Virginia, or anywhere else in our service areas, we are here to help.
At National Addiction Specialists, we provide convenient, confidential, and expert telemedicine-based Suboxone treatment, including personalized tapering plans. We accept Medicaid and Medicare, ensuring that quality care is accessible when you need it most.
You’ve come this far, and we’re here to help you take the next step towards lasting freedom.
Start your personalized recovery plan today.
This article was medically reviewed by:
Chad Elkin, MD, DFASAM is a board-certified addiction medicine physician, founder, and Chief Medical Officer of National Addiction Specialists, dedicated to treating substance use disorders. A Distinguished Fellow of the American Society of Addiction Medicine (ASAM), Dr Elkin currently serves as President of the Tennessee Society of Addiction Medicine (TNSAM) and has held various leadership roles within the organization. Dr Elkin chairs ASAM’s Health Technology Subcommittee and is an active member of its Practice Management and Regulatory Affairs Committee, State Advocacy and Legislative Affairs Committee, and other committees. He also serves on the planning committee for the Vanderbilt Mid-South Addiction Conference. Committed to advancing evidence-based policy, Dr Elkin is Chairman of the Tennessee Association of Alcohol, Drug, & Other Addiction Services (TAADAS) Addiction Medicine Council, which collaborates with the TN Department of Mental Health & Substance Abuse Services (TDMHSAS). He has contributed to numerous local, state, and national task forces, helping develop professional guidelines, policies, and laws that align with best practices in addiction medicine. His work focuses on reducing addiction-related harm, combating stigma, and ensuring access to effective treatment.Passionate about the field of addiction medicine, he remains dedicated to shaping policy and enhancing patient care.
Suboxone® and Subutex® are a registered trademark of Indivior UK Limited. Any mention and reference of Suboxone® and Subutex® in this website is for informational purposes only and is not an endorsement or sponsorship by Indivior UK Limited.






